[Content note: food, dieting, obesity]
I.
The Hungry Brain gives off a bit of a Malcolm Gladwell vibe, with its cutesy name and pop-neuroscience style. But don’t be fooled. Stephan Guyenet is no Gladwell-style dilettante. He’s a neuroscientist studying nutrition, with a side job as a nutrition consultant, who spends his spare time blogging about nutrition, tweeting about nutrition, and speaking at nutrition-related conferences. He is very serious about what he does and his book is exactly as good as I would have hoped. Not only does it provide the best introduction to nutrition I’ve ever seen, but it incidentally explains other neuroscience topics better than the books directly about them do.
I first learned about Guyenet’s work from his various debates with Gary Taubes and his supporters, where he usually represents the “scientific consensus” side. He is very careful to emphasize that the consensus doesn’t look anything like Taubes’ caricature of it. The consensus doesn’t believe that obesity is just about weak-willed people voluntarily choosing to eat too much, or that obese people would get thin if they just tried diet and exercise, or that all calories are the same. He writes
The [calories in, calories out] model is the idea that our body weight is determined by voluntary decisions about how much we eat and move, and in order to control our body weight, all we need is a little advice about how many calories to eat and burn, and a little willpower. The primary defining feature of this model is that it assumes that food intake and body fatness are not regulated. This model seems to exist mostly to make lean people feel smug, since it attributes their leanness entirely to wise voluntary decisions and a strong character. I think at this point, few people in the research world believe the CICO model.
[Debate opponent Dr. David] Ludwig and I both agree that it provides a poor fit for the evidence. As an alternative, Ludwig proposes the insulin model, which states that the primary cause of obesity is excessive insulin action on fat cells, which in turn is caused principally by rapidly-digesting carbohydrate. According to this model, too much insulin reduces blood levels of glucose and fatty acids (the two primary circulating metabolic fuels), simultaneously leading to hunger, fatigue, and fat gain. Overeating is caused by a kind of “internal starvation”. There are other versions of the insulin model, but this is the one advocated by Ludwig (and Taubes), so it will be my focus.
But there’s a third model, not mentioned by Ludwig or Taubes, which is the one that predominates in my field. It acknowledges the fact that body weight is regulated, but the regulation happens in the brain, in response to signals from the body that indicate its energy status. Chief among these signals is the hormone leptin, but many others play a role (insulin, ghrelin, glucagon, CCK, GLP-1, glucose, amino acids, etc.)
The Hungry Brain is part of Guyenet’s attempt to explain this third model, and it basically succeeds. But like many “third way” style proposals, it leaves a lot of ambiguity. With CICO, at least you know where you stand – confident that everything is based on willpower and that you can ignore biology completely. And again, with Taubes, you know where you stand – confident that willpower is useless and that low-carb diets will solve everything. The Hungry Brain is a little more complicated, a little harder to get a read on, and at times pretty wishy-washy.
But listening to people’s confidently-asserted simple and elegant ideas was how we got into this mess, so whatever, let’s keep reading.
II.
The Hungry Brain begins with the typical ritual invocation of the obesity epidemic. Did you know there are entire premodern cultures where literally nobody is obese? That in the 1800s, only 5% of Americans were? That the prevalence of obesity has doubled since 1980?
Researchers have been keeping records of how much people eat for a long time, and increased food intake since 1980 perfectly explains increased obesity since 1980 – there is no need to bring in decreased exercise or any other factors. Exercise has decreased since the times when we were all tilling fields ten hours a day, but for most of history, as our exercise decreased, our food intake decreased as well. But for some reason, starting around 1980, the two factors uncoupled, and food intake started to rise despite exercise continuing to decrease.
Guyenet discusses many different reasons this might have happened, including stress-related overeating, poor sleep, and quick prepackaged food. But the ideas he keeps coming back to again and again are food reward and satiety.
In the 1970s, scientists wanted to develop new rat models of obesity. This was harder than it sounded; rats ate only as much as they needed and never got fat. Various groups tried to design various new forms of rat chow with extra fat, extra sugar, et cetera, with only moderate success – sometimes they could get the rats to eat a little too much and gradually become sort of obese, but it was a hard process. Then, almost by accident, someone tried feeding the rats human snack food, and they ballooned up to be as fat as, well, humans. The book:
Palatable human food is the most effective way to cause a normal rat to spontaneously overeat and become obese, and its fattening effect cannot be attributed solely to its fat or sugar content.
So what does cause this fattening effect? I think the book’s answer is “no single factor, but that doesn’t matter, because capitalism is an optimization process that designs foods to be as rewarding as possible, so however many different factors there are, every single one of them will be present in your bag of Doritos”. But to be more scientific about it, the specific things involved are some combination of sweet/salty/umami tastes, certain ratios of fat and sugar, and reinforced preferences for certain flavors.
Modern food isn’t just unusually rewarding, it’s also unusually bad at making us full. The brain has some pretty sophisticated mechanisms to determine when we’ve eaten enough; these usually involve estimating food’s calorie load from its mass and fiber level. But modern food is calorically dense – it contains many more calories than predicted per unit mass – and fiber-poor. This fools the brain into thinking that we’re eating less than we really are, and shuts down the system that would normally make us feel full once we’ve had enough. Simultaneously, the extremely high level of food reward tricks the brain into thinking that this food is especially nutritionally valuable and that it should relax its normal constraints.
Adding to all of this is the so-called “buffet effect”, where people will eat more calories from a variety of foods presented together than they would from any single food alone. My mother likes to talk about her “extra dessert stomach”, ie the thing where you can gorge yourself on a burger and fries until you’re totally full and couldn’t eat another bite – but then mysteriously find room for an ice cream sundae afterwards. This is apparently a real thing that’s been confirmed in scientific experiments, and a major difference between us and our ancestors. The !Kung Bushmen, everyone’s go-to example of an all-natural hunter-gatherer tribe, apparently get 50% of their calories from a single food, the mongongo nut, and another 40% from meat. Meanwhile, we design our meals to include as many unlike foods as possible – for example, a burger with fries, soda, and a milkshake for dessert. This once again causes the brain to relax its usual strict constraints on appetite and let us eat more than we should.
The book sums all of these things up into the idea of “food reward” making some foods “hyperpalatable” and “seducing” the reward mechanism in order to produce a sort of “food addiction” that leads to “cravings”, the “obesity epidemic”, and a profusion of “scare quotes”.
I’m being a little bit harsh here, but only to highlight a fundamental question. Guyenet goes into brilliant detail about things like the exact way the ventral tegmental area of the brain responds to food-related signals, but in the end, it all sounds suspiciously like “food tastes good so we eat a lot of it”. It’s hard to see where exactly this differs from the paradigm that he dismisses as “attributing leanness to wise voluntary decisions and a strong character…to make lean people feel smug”. Yes, food tastes good so we eat a lot of it. And Reddit is fun to read, but if someone browses Reddit ten hours a day and doesn’t do any work then we start speculating about their character, and maybe even feeling smug. This part of the book, taken alone, doesn’t really explain why we shouldn’t be doing that about weight too.
III.
There is only one fat person on the Melanesian island of Kitava – a businessman who spends most of his time in modern urbanized New Guinea, eating Western food. The Kitavans have enough food, and they live a relaxed tropical lifestyle that doesn’t demand excessive exercise. But their bodies match caloric intake to expenditure with impressive precision. So do the !Kung with their mongongo nuts, Inuit with their blubber, et cetera.
And so do Westerners who limit themselves to bland food. In 1965, some scientists locked people in a room where they could only eat nutrient sludge dispensed from a machine. Even though the volunteers had no idea how many calories the nutrient sludge was, they ate exactly enough to maintain their normal weight, proving the existence of a “sixth sense” for food caloric content. Next, they locked morbidly obese people in the same room. They ended up eating only tiny amounts of the nutrient sludge, one or two hundred calories a day, without feeling any hunger. This proved that their bodies “wanted” to lose the excess weight and preferred to simply live off stored fat once removed from the overly-rewarding food environment. After six months on the sludge, a man who weighed 400 lbs at the start of the experiment was down to 200, without consciously trying to reduce his weight.
In a similar experiment going the opposite direction, Ethan Sims got normal-weight prison inmates to eat extraordinary amounts of food – yet most of them still had trouble gaining weight. He had to dial their caloric intake up to 10,000/day – four times more than a normal person – before he was able to successfully make them obese. And after the experiment, he noted that “most of them hardly had any appetite for weeks afterward, and the majority slimmed back down to their normal weight”.
What is going on here? Like so many questions, this one can best be solved by grotesque Frankenstein-style suturing together of the bodies of living creatures.
In the 1940s, scientists discovered that if they damaged the ventromedial hypothalamic nucleus (VMN) of rats, the rats would basically never stop eating, becoming grotesquely obese. They theorized that the VMN was a “satiety center” that gave rats the ability to feel full; without it, they would feel hungry forever. Later on, a strain of mutant rats was discovered that seemed to naturally have the same sort of issue, despite seemingly intact hypothalami. Scientists wondered if there might be a hormonal problem, and so they artificially conjoined these rats to healthy normal rats, sewing together their circulatory systems into a single network. The result: when a VMN-lesioned rat was joined to a normal rat, the VMN-lesioned rat stayed the same, but the normal rat stopped eating and starved to death. When a mutant rat was joined to a normal rat, the normal rat stayed the same and the mutant rat recovered and became normal weight.
The theory they came up with to explain the results was this: fat must produce some kind of satiety hormone, saying “Look, you already have a lot of fat, you can feel full and stop eating now”. The VMN of the hypothalamus must detect this message and tell the brain to feel full and stop eating. So the VMN-lesioned rats, whose detector was mostly damaged, responded by never feeling full, eating more and more food, and secreting more and more (useless) satiety hormone. When they were joined to normal rats, their glut of satiety hormones flooded the normal rats – and their normal brain, suddenly bombarded with “YOU ALREADY HAVE WAY TOO MUCH FAT” messages, stopped eating entirely.
The mutant rats, on the other hand, had lost the ability to produce the satiety hormone. They, too, felt hungry all the time and ate everything. But when they were joined to a normal rat, the normal levels of satiety hormone flowed from the normal rat into the mutant rat, reached the fully-functional detector in their brains, and made them feel full, curing their obesity.
Skip over a lot of scientific infighting and unfortunate priority disputes and patent battles, and it turns out the satiety hormone is real, exists in humans as well, and is called leptin. A few scientists managed to track down some cases of genetic leptin deficiency in humans, our equivalent of the mutant rats, and, well…
Usually they are of normal birth weight and then they’re very, very hungry from the first weeks and months of life. By age one, they have obesity. By age two, they weigh 55-65 pounds, and their obesity only accelerates from there. While a normal child may be about 25% fat, and a typical child with obesity may be 40% fat, leptin-deficient children are up to 60% fat. Farooqi explains that the primary reason leptin-deficient children develop obesity is that they have “an incredible drive to eat”…leptin-deficient children are nearly always hungry, and they almost always want to eat, even shortly after meals. Their appetite is so exaggerated that it’s almost impossible to put them on a diet: if their food is restricted, they find some way to eat, including retrieving stale morsels from the trash can and gnawing on fish sticks directly from the freezer. This is the desperation of starvation […]
Unlike normal teenagers, those with leptin deficiency don’t have much interest in films, dating, or other teenage pursuits. They want to talk about food, about recipes. “Everything they do, think about, talk about, has to do with food” says [Dr.] Farooqi. This shows that the [leptin system] does much more than simply regulate appetite – it’s so deeply rooted in the brain that it has the ability to hijack a broad swath of brain functions, including emotions and cognition.
It’s the leptin-VNM-feedback system (dubbed the “lipostat”) that helps people match their caloric intake to their caloric requirements so impressively. The lipostat is what keeps hunter-gatherers eating exactly the right number of mongongo nuts, and what keeps modern Western overeaters at much closer to the right weight than they could otherwise expect.
The lipostat-brain interface doesn’t just control the raw feeling of hunger, it seems to have a wide range of food-related effects, including some on higher cognition. Ancel Keys (of getting-blamed-for-everything fame) ran the Minnesota Starvation Experiment on some unlucky conscientious objectors to World War II. He starved them until they lost 25% of their body weight, and found that:
Over the course of their weight loss, Keys’s subjects developed a remarkable obsession with food. In addition to their inescapable, gnawing hunger, their conversations, thoughts, fantasies, and dreams revolved around food and eating – part of a phenomenon Keys called “semistarvation neurosis”. They became fascinated by recipes and cookbooks, and some even began collecting cooking utensils. Like leptin-deficient adolescents, their lives revolved around food. Also like leptin-deficient adolescents, they had very low leptin levels due to their semi-starved state.
Unsurprisingly, as soon as the experiment ended, they gorged themselves until they were right back at their pre-experiment weights (but no higher), at which point they lost their weird food obsession.
Just as a well-functioning lipostat is very good at keeping people normal weight, a malfunctioning lipostat is very good at keeping people obese. Fat people seem to have “leptin resistance”, sort of like the VMN-lesioned rats, so that their bodies get confused about how much fat they have. Suppose a healthy person weighs 150 lbs, his body is on board with that, and his lipostat is set to defend a 150 lb set point. Then for some reason he becomes leptin-resistant, so that the brain is only half as good at detecting leptin as it should be. Now he will have to be 300 lbs before his brain “believes” he is the right weight and stops encouraging him to eat more. If he goes down to a “mere” 250 lbs, then he will go into the same semistarvation neurosis as Ancel Keys’ experimental subjects and become desperately obsessed with food until they get back up to 300 again. Or his body will just slow down metabolism until his diet brings him back up. Or any of a bunch of other ways the lipostat has to restore weight when it wants to.
This explains the well-known phenomenon where contestants on The Biggest Loser who lose 200 or 300 pounds for the television camera pretty much always gain it back after the show ends. Even though they’re highly motivated and starting from a good place, their lipostat has seized on their previous weight as the set point it wants to defend, and resisting the lipostat is somewhere between hard and impossible. As far as I know, nobody has taken Amptoons up on their challenge to find a single peer-reviewed study showing any diet that can consistently bring fat people to normal weight and keep them there. After a certain level of lipostat dysregulation, “solving” weight problems by diet and exercise becomes hard-to-impossible, and the people who loudly insist otherwise tend to kind of be jerks.
And alas, it doesn’t seem to work to just inject leptin directly. As per Guyenet
People with garden variety obesity already have high levels of leptin…while leptin therapy does cause some amount of fat loss, it requires enormous doses to be effective – up to forty times the normal circulating amount. Also troubling is the extremely variable response, with some people losing over thirty pounds and others losing little or no weight. This is a far cry from the powerful fat-busting effect of leptin in rodents. [Leptin as] the new miracle weight-loss drug never made it to market.
This disappointment forced the academic and pharmaceutical communities to confront a distressing possibility: the leptin system defends vigorously against weight loss, but not so vigorously against weight gain. “I have always thought, and continue to believe,” explained [leptin expert Rudy] Leibel, “that the leptin hormone is really a mechanism for detecting deficiency, not excess.” It’s not designed to constrain body fatness, perhaps because being too fat is rarely a problem in the wild. Many researchers now believe that while low leptin levels in humans engage a powerful starvation response that promotes fat gain, high leptin levels don’t engage an equally powerful response that promotes fat loss.
Yet something seems to oppose rapid fat gain, as Ethan Sims’ overfeeding studies (and others) have shown. Although leptin clearly defends the lower limit of adiposity, the upper limit may be defended by an additional, unidentified factor – in some people more than others.
This is the other half of the uncomfortable dichotomy that makes me characterize The Hungry Brain as “wishy-washy”. The lipostat is a powerful and essentially involuntary mechanism for getting weight exactly where the brain wants, whether individual dieters are cooperative or not. Here it looks like obesity is nobody’s fault, unrelated to voluntary decisions, and that the standard paradigm really is just an attempt by lean people to feel smug. Practical diet advice starts to look like “inject yourself with quantities of leptin so massive that they overcome your body’s resistance”. How do we connect this with the other half of the book, the half with food reward and satiety and all that?
IV.
With more rat studies!
Dr. Barry Levin fed rats either a healthy-rat-food diet or a hyperpalatable-human-food diet, then starved and overfed them in various ways. He found that the rats defended their obesity set points in the expected manner, but that the same rats defend different set points depending on their diets. Rats on healthy-rat-food defended a low, healthy-for-rats set point; rats on hyperpalatable-human-food defended a higher set point that kept them obese.
That is, suppose you give a rat as much Standardized Food Product as it can eat. It eats until it weighs 8 ounces, and stays that weight for a while. Then you starve it until it only weighs 6 ounces, and it’s pretty upset. Then you let it eat as much as it wants again, and it overeats until it gets back to 8 ounces, then eats normally and maintains that weight.
But suppose you get a rat as many Oreos as it can eat. It eats until it weighs 16 ounces, and stays that weight for a while. Then you starve it until it only weighs 6 ounces. Then you let it eat as much as it wants again, and this time it overeats until it gets back to 16 ounces, and eats normally to maintain that weight.
Something similar seems to happen with humans. A guy named Michel Cabanac ran an experiment in which he put overweight people on two diets. In the first diet, they ate Standardized Food Product, and naturally lost weight since it wasn’t very good and they didn’t eat very much of it. In the second diet, he urged people to eat less until they matched the first group’s weight loss, but to keep eating the same foods as normal – just less of them. The second group reported being hungry and having a lot of trouble dieting; the first group reported not being hungry and not having any trouble at all.
Guyenet concludes:
Calorie-dense, highly rewarding food may favor overeating and weight gain not just because we passively overeat it but also because it turns up the set point of the lipostat. This may be one reason why regularly eating junk food seems to be a fast track to obesity in both animals and humans…focusing the diet on less rewarding foods may make it easier to lose weight and maintain weight loss because the lipostat doesn’t fight it as vigorously. This may be part of the explanation for why all weight-loss diets seem to work to some extent – even those that are based on diametrically opposed principles, such as low-fat, low-carbohydrate, paleo, and vegan diets. Because each diet excludes major reward factors, they may all lower the adiposity set point somewhat.
(this reminds me of the Shangri-La Diet, where people would drink two tablespoons of olive oil in the morning, then find it was easy to diet without getting hungry during the day. People wondered whether maybe the tastelessness of the olive oil had something to do with it. Could it be that the olive oil is temporarily bringing the lipostat down to its “bland food” level?)
Why should some food make the lipostat work better than other food? Guyenet now gets to some of his own research, which is on a type of brain cell called a POMC neuron. These neurons produce various chemicals, including a sort of anti-leptin called Neuropeptide Y, and they seem to be a very fundamental part of the lipostat and hunger system. In fact, if you use superprecise chemical techniques to kill NPY neurons but nothing else, you can cure obesity in rats.
The area of the hypothalamus with POMC neurons seem to be damaged in overweight rats and overweight humans. Microglia and astrocytes, the brain’s damage-management and repair cells, proliferated in appetite-related centers, but nowhere else. Maybe this literal damage corresponds to the metaphorically “damaged” lipostat that’s failing to maintain weight normally, or the “damaged” leptin detector that seems to be misinterpreting the body’s obesity?
In any case, eating normal rat food for long enough appears to heal this damage:
Our results suggest that obese rodents suffer from a mild form of brain injury in an area of the brain that’s critical for regulating food intake and adiposity. Not only that, but the injury response and inflammation that developed when animals were placed on a fattening diet preceded the development of obesity, suggesting that this brain injury could have played a role in the fattening process.
Guyenet isn’t exactly sure what aspect of modern diets cause the injury:
Many researchers have tried to narrow down the mechanisms by which this food causes changes in the hypothalamus and obesity, and they have come up with a number of hypotheses with varying amounts of evidence to support them. Some researchers believe the low fiber content of the diet precipitates inflammation and obesity by its adverse effects on bacterial populations in the gut (the gut microbiota). Others propose that saturated fat is behind the effect, and unsaturated fats like olive oil are less fattening. Still others believe the harmful effects of overeating itself, including the inflammation caused by excess fat and sugar in the bloodstream and in cells, may affect the hypothalamus and gradually increase the set point. In the end, these mechanisms could all be working together to promote obesity. We don’t know all the details yet, but we do know that easy access to refined, calorie-dense, highly rewarding food leads to fat gain and insidious changes in the lipostat in a variety of species, including humans. This is particularly true when the diet offers a wide variety of sensory experiences, such as the hyperfattening “cafeteria diet” we encountered in chapter 1.
Personally, I believe overeating itself probably plays an important role in the process that increases the adiposity set point. In other words, repeated bouts of overeating don’t just make us fat; they make our bodies want to stay fat. This is consistent with the simple observation that in the United States, most of our annual weight gain occurs during the six-week holiday feasting period between Thanksgiving and the new year, and that this extra weight tends to stick with us after the holidays are over…because of some combination of food quantity and quality, holiday feasting ratchets up the adiposity set point of susceptible people a little bit each year, leading us to gradually accumulate and defend a substantial amount of fat. Since we also tend to gain weight at a slower rate during the rest of the year, intermittent periods of overeating outside of the holidays probably contribute as well.
How might this happen? We aren’t entirely sure, but researchers, including Jeff Friedman, have a possible explanation: excess leptin itself may contribute to leptin resistance. To understand how this works, I need to give you an additional piece of information: Leptin doesn’t just correlate with body fat levels; it also responds to short-term changes in calorie intake. So if you overeat for a few days, your leptin level can increase substantially, even if your adiposity has scarcely changed (and after your calorie intake goes back to normal, so does your leptin). As an analogy for how this can cause leptin resistance, imagine listening to music that’s too loud. At first, it’s thunderous, but eventually, you damage your hearing, and the volume drops. Likewise, when we eat too much food over the course of a few days, leptin levels increase sharply, and this may begin to desensitize the brain circuits that respond to leptin. Yet Rudy Leibel’s group has also shown that high leptin levels alone aren’t enough – the hypothalamus also seems to require a second “hit” for high leptin to increase the set point of the lipostat. This second hit could be the brain injury we, and others, have identified in obese rodents and humans.
And he isn’t sure exactly what aspect of the normal rodent diet promotes the healing:
I did do some research in mice suggesting that unrefined, simple food does reverse the brain changes and the obesity. I don’t claim that it’s all attributable to the blandness though– the two diets differed in many respects (palatability, calorie density, fiber content, macronutrient profile, fatty acid profile, content of nonessential nutrients like polyphenols). Also, we don’t know how well the finding applies to humans yet. One of the problems is that it’s very hard to get a group of humans to adhere strictly to a whole food diet for long enough to study its long-term effects on appetite and body fatness. People are very attached to the pleasures of the palate!
But all of this together seems to point to a potential synthesis between the hyperpalatability and lipostat models. For most of human history, the lipostat faced only mild stresses and was able to maintain a normal weight without much trouble. Modern society has been incentivized to produce hyperpalatable, low-satiety food as superstimuli. This modern food is able to overwhelm normal satiety cues and produce short-term overeating. And for some reason this short-term overeating raises the lipostat’s set point (maybe because of brain damage and leptin resistance), causing long-term weight gain in a way that is very difficult to reverse.
V.
But I still have trouble reconciling these two points of view.
A couple of days ago, I walked by an ice cream store. I’d just finished lunch, and I wasn’t very hungry at the time, but it looked like really good ice cream, and it was hot out, so I gave in to temptation and ate a 700 calories sundae. Does this mean:
1. Based on the one pound = 3500 calories heuristic, I have now gained 0.2 lbs. That extra weight will stay with me my whole life, or at least until some day when I diet and eat 700 calories less than my requirement. If I were to eat ice cream like this a hundred times, I would gain twenty pounds.
2. My lipostat adjusts for the 700 extra calories, and causes me to exercise more, or ramp up my metabolism, or burn more brown fat, or eat less later on, or something. I don’t gain any weight, and eating the ice cream was that rarest of all human experiences, a completely guiltless pleasure. I should eat ice cream whenever I feel like it, or else I am committing the sin of denying myself a lawful pleasure.
3. My lipostat will more or less take care of the ice cream today, and I won’t notice the 0.2 pounds on the scale, but it is very gradually doing hard-to-measure damage to my hypothalamus, and if I keep eating ice cream like this, then one day when I’m in my forties I’m going to wake up weighing three hundred pounds, and no diet will ever be able to help me.
4. Not only will I gain 0.2 pounds immediately, but my lipostat will adjust to want to be 0.2 pounds heavier, and I will never lose it, even if I try really hard to diet later.
5. The above scenario is impossible. Even if I think I just ate ice cream because it looked good, in reality I was driven to do it by my lipostat’s quest for caloric balance. Any feeling of choice in the matter is an illusion.
I think the reason this is so confusing is because the real answer is “it could be any one of these, depending on genetics.”
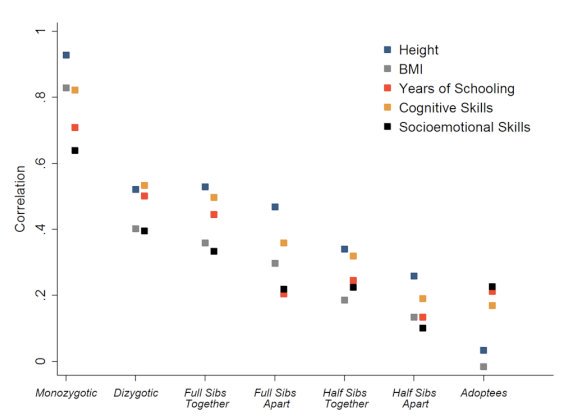
Note the position of the grey squares representing BMI
Right now, within this culture, variation in BMI is mostly genetic. This isn’t to say that non-genetic factors aren’t involved – the difference between 1800s America and 2017 America is non-genetic, and so is the difference between the perfectly-healthy Kitavans on Kitava and the one Kitavan guy who moved to New Guinea. But once everyone alike is exposed to the 2017-American food environment, differences between the people in that environment seem to be really hereditary and not-at-all-related to learned behavior. Guyenet acknowledges this:
Genes explain that friend of yours who seems to eat a lot of food, never exercises, and yet remains lean. Claude Bouchard, a genetics researcher at the Pennington Biomedical Research Center in Baton Rouge, Louisiana, has shown that some people are intrinsically resistant to gaining weight even when they overeat, and that this trait is genetically influenced. Bouchard’s team recruited twelve pairs of identical twins and overfed each person by 1,000 calories per day above his caloric needs, for one hundred days. In other words, each person overate the same food by the same amount, under controlled conditions, for the duration of the study.
If overeating affects everyone the same, then they should all have gained the same amount of weight. Yet Bouchard observed that weight gain ranged from nine to twenty-nine pounds! Identical twins tended to gain the same amount of weight and fat as each other, while unrelated subjects had more divergent responses…Not only do some people have more of a tendency to overeat than others, but some people are intrinsically more resistant to gaining fat even if they do overeat.
The research of James Levine, an endocrinologist who works with the Mayo Clinic and Arizona State University, explains this puzzling phenomenon. In a carefully controlled overfeeding study, his team showed that the primary reason some people readily burn off excess calories is that they ramp up a form of calorie-burning called “non-exercise activity thermogenesis” (NEAT). NEAT is basically a fancy term for fidgeting. When certain people overeat, their brains boost calorie expenditure by making them fidget, change posture frequently, and make other small movements throughout the day. It’s an involuntary process, and Levine’s data show that it can incinerate nearly 700 calories per day. The “most gifted” of Levine’s subjects gained less than a pound of body fat from eating 1,000 extra calories per day for eight weeks. Yet the strength of the response was highly variable, and the “least gifted” of Levine’s subjects didn’t increase NEAT at all, shunting all the excess calories into fat tissue and gaining over nine pounds of body fat…
Together, these studies offer indisputable evidence that genetics plays a central role in obesity and dispatch the idea that obesity is primarily due to acquired psychological traits.
These studies suggest that one way genetics affects obesity is by altering the tolerance level of the lipostat. Genetically privileged people may have very finicky lipostats that immediately burn off any extra calories they eat, and which never become dysregulated. Genetically unlucky people may have weak lipostats which fail to defend against weight gain, or which are too willing to adjust their set point up in the presence of an unhealthy food environment.
So, given how many people seem to have completely different weight-gain-related experiences to each other, the wishy-washyness here might be a feature rather than a bug.
One reason I’ve always found genetics so exciting is that there are all these fields – nutrition is a great example, but this applies at least as much to psychiatry – where everyone has wildly different personal experiences, and where there’s a large and vocal population of people who say that the research is exactly the opposite of their lived experiences. People have tried to shoehorn the experiences to fit the research, with various levels of plausibility and condescendingness. And for some reason, it’s always really hard to generate the hypothesis “people’s different experiences aren’t an illusion; people are genuinely really different”. Once you start looking at genetics, everything sort of falls into place, and ideas which seemed wishy-washy or self-contradictory before are revealed as just reflecting the diversity of nature. People who were previously at each other’s throats disputing different interpretations of the human condition are able to peacefully agree that there are many different human conditions, and that maybe we can all just get along. The Hungry Brain and other good books in its vein offer a vision for how we might one day be able to do that in nutrition science.
VI.
Lest I end on too positive a note, let me reiterate the part where happiness is inherently bad and a sort of neo-Puritan asceticism is the only way to avoid an early grave.
There’s a sort of fatalism to talking about “food reward”. If the enemy were saturated fat, we could just stick with the sugary sweetness of Coca-Cola. If the enemy were carbohydrates, we could go out for steak every night. But what do we do if the enemy is deliciousness itself?
A few weeks ago Guyenet announced The Bland Food Cookbook, a collection of tasteless recipes guaranteed to be low food-reward and so discourage overeating. It was such a natural extension of his philosophy that it took me a whole ten seconds to realize it was an April Fools joke. But why should it be? Shouldn’t this be exactly the sort of thing we’re going for?
I asked him, and he responded that:
If I thought enough people would actually be capable of following the diet, I would consider making such a cookbook non-ironically. The second point I want to make here is that there are many ways to lose weight, and deliberately reducing food reward is only one of them. You could also exercise, eat a low-calorie-density diet, eat a high-protein diet, restrict a macronutrient, restrict animal foods, restrict plant foods, eat nothing but potatoes. Most approaches overlap with a low-reward diet to varying degrees, but I don’t think the low reward value encapsulates everything about why every weight loss strategy works. BTW, low-carb folks often have a knee-jerk reaction to the low-reward thing that goes something like this: “I eat food that’s delicious, such as steaks, bacon, butter, etc. It’s not low in reward.” But it is low reward in the sense that you’re cutting out a broad swath of foods, and an entire macronutrient, that the brain very much wants you to eat. Eating more of a particular category of rewarding food doesn’t completely make up for the fact that you’re cutting out a whole other category of rewarding food that you would avidly consume if you weren’t restricting yourself.
So things aren’t maximally bad. And hunter-gatherers enjoy their healthy diets just fine. And certainly there are things like steak and wine and so on which are traditionally “good food” without being hyperprocessed hyperpalatable junk food. But if you really enjoy a glass of Chardonnay, is that “food reward” in a sense that’s potentially dangerous? Is anything safe? What about mongongo nuts? Is there anywhere we can get them?
At least the consolation of things making a little more sense. One thing that always used to bother me was the so-called “ice cream diet” – that is, if you eat a 700-calorie ice cream sundae for breakfast, lunch, and dinner every day, that’ll be only 2100 calories – around the average person’s daily requirement, and low enough for many people to lose weight. Why wouldn’t you want to do that? The idea of junk food being inherently damaging – while it has a bit of Puritan feel to it – at least fits our intuitions on these sorts of things and gives us a first step towards reconciling the conventional wisdom and the calorie math.
Overall I strongly recommend The Hungry Brain for everything I talk about here and for some other good topics I didn’t even get to (stress, sleep, economics). I would also recommend Guyenet’s other writing, especially his debate with Dr. David Ludwig on the causes of obesity (Part 1, Part 2, Part 3. I also recommend the list of diet tips that Guyenet gives at the end of the book. I won’t give them all away here – he’s been nice enough to me that maybe I should repay him by not reprinting the entire text of his book online for free. But it’s similar to a lot of standard advice for healthy living, albeit with more interesting reasoning behind it. Did you know that exercise might help stabilize the lipostat? Or that protein might do the same? Also, one piece of advice you might not hear anywhere else – potatoes are apparently off-the-charts in terms of satiety factor and may be one of the single best things to diet on.
And speaking of good things to diet on…
(note that this next part is my own opinion, not taken from The Hungry Brain or endorsed by Stephan Guyenet)
Slate Star Codex’s first and most loyal sponsor is MealSquares, a “nutritionally complete” food product sort of like a whole-foods-based, protein-rich, solid version of Soylent (it looks and tastes basically like a scone). I’m having some trouble writing this paragraph, because I want to recommend them as potentially dovetailing with The Hungry Brain‘s philosophy of nutrition without using phrases that might make MealSquares Inc angry at me like “bland”, “low food reward”, or “not hyperpalatable”. I think the best I can come up with is “unlikely to injure your hypothalamus”. So, if you’re looking for an easy way to quit the junk food and try a low-variety diet that’s unlikely to injure your hypothalamus, I recommend MealSquares as worth a look.

















The focus on 1980 is not warranted. That is when the clinical obesity took off…but people don’t just put on 60 pounds all of a sudden. 1945 is a reasonable estimate of when weights started climbing.
Obesity rates took off like they did because it’s an arbitrary BMI cutoff that was at the top end of the bell curve. Since the mid 1900s, mean BMIs increased, and the distribution started to skew right…such that obesity rates remained a small number until the bulkier part of the curve started to cross the 30BMI cutoff in 1980. Couple this with the average age increasing substantially over this time and there you have it.
“potatoes are apparently off-the-charts in terms of satiety factor and may be one of the single best things to diet on”
This contradicts with:
https://www.hsph.harvard.edu/nutritionsource/2014/01/24/the-problem-with-potatoes/
Should I eat potatoes for weight loss or not? I’m confused
The harvard post is severely lacking.
Should you? I bet, yes. But this is an easy test. Boil 500 calories of potatoes and eat them all. Use a LITTLE salt and pepper if you want but nothing else. No butter, cheese, oil, etc.
How full are you now? and in 5 hours?
Oh you couldn’t even finish them? Ok.
How does the nutrient sludge study prove that the body is regulating caloric intake? A behavioral explanation hasn’t been ruled out so far as I can see: The healthy folks were habituated to consume the appropriate amount of calories. The unhealthy folks did not enjoy the sludge and had no reason to overeat given their ability to live off of their excessive body fat. That said, I have been reading Guyenet for years and have lost weight on potatoes and he’s probs right.
The effect of bland food on our appetize is pretty interesting.
Anyone ever had the experience of bland food making them feel nauseous? Happens to me with oatmeal, mostly. I could barely eat two spoons of plain oatmeal without gaging, but add a teaspoon of peanut butter and nutella and it’s one of my go-to snacks. Could it be some extreme form of weight regulating? Or maybe I just really don’t like plain oatmeal, who knows.
Oatmeal is sticky. I suppose that depending on the conformation of your pharynx and esophagus, it may stick to their walls, triggering your gag reflex. If you add a fat ingredient it will act as a lubricant, allowing oatmeal to pass through your upper digestive tract more easily.
Have you come across Chris Kresser’s website? He is good friends with Stephan Guyanet and applies similar rigor when looking at the research. He has more of a Paleo approach, and focuses on general health rather than obesity, but I find him extremely convincing. They did a podcast together a couple of weeks ago.
…someone gets triggered by food?
Maybe, but more likely someone gets hungry.
Although technically I suppose that’s still a “trigger”, only the quale invoked is hunger rather than fear/anger/etc.
Anything can be a trigger. It’s one of the things that is critisized about trigger warnings. You either have to warn of a ridiculouse amount of things or won’t catch the actual triggers at all.
Doesn’t apply to “content warning: food” though; food talk (especially diet talk) is an extremely common trigger for people with eating disorders and any sensible 80/20 list of content warnings would include it.
I do have to wonder what value – these warnings not being part of (as far as I know) a systematic tag system allowing the post to be programmatically hidden from view – it has over “this is a review of a book with ‘hungry’ in the title” or “today’s blog post is called ‘Anorexia and…'”.
Dieting advice is a common trigger for people with eating disorders. Kelsey from theunitofcaring on tumblr has said that she blacklists dieting advice, for instance, so that tag in the top is helpful to her, presumably.
In Scott’s defense, this didn’t say “trigger warning”. I viewed it more as a #hashtag sort of thing so at some point it might be easier to search for all food-related posts at some point in the future.
Hang on – if the frankenrats shared a circulatory system, how come one of them could starve to death? Wouldn’t it have been getting nutrients from the other rat via the shared bloodstream? When we put humans on a nutrient drip they don’t die of starvation.
Actually they do, just very slowly. Don’t ask me how.
I had an uncle who had throat cancer a few years back. He couldn’t eat at all. He would get two huge bags of a nutrient drip a day. It kept him alive for a while but he was nothing but bones and skin (sitting hurt). This went on for a few weeks maybe even one or two months until he died.
The theory behind Seth Roberts’ Shangri-La diet is pretty similar to Guyenet’s view. Seth basically believed that the body uses taste-calorie association to move the set point around so we would get fat in periods of plenty and lose fat in periods of scarcity. This happens because in periods of plenty we tend to eat tastier food. So he recommended that if we want to lose weight we should ingest calories without taste. It’s a pretty similar conclusion to the bland food recommendation. Seth also thought that the obesity epidemic was due to modern foods abusing our proxies for nutrition, and that monosodium glutamate was specially to blame. If anyone is curious here’s Seth’s papers where he describes his theory of set points (but not his diet):
http://media.sethroberts.net/about/whatmakesfoodfattening.pdf
I wonder if it’s possible to gain a bird’s-eye view of nutrition science. How many researchers are there, approximately, in nutrition science? Are they mostly working in university research labs or government organisations or for commercial companies? How many PhDs are produced each year? What are the top journals in the field? Are there giants whom everybody reveres? Is there a college-level or higher textbook that most people agree reflects the consensus in the field?
How often do you cook? I cook all of my dinners and lunches at the weekend (I go to the mensa during the week and the food there is rarely anywhere close to “hyperpalatable”). I never use any pre-made sauces or other stuff that you just warm up.
I actually used to eat a lot more processed foods before I learned to cook. I was not obese or even overweight even before (I am generally not very hungry, I have to actually try to remind myself to eat most of the time), but when I started cooking, a lot of the processed foods gradually started tasting rather bad. I still crave chocolate (mostly with marzipan) on occasion, but I don’t remember when I last bought a bag of chips or something like that. I remember that I felt rather lazy once and bought a patê I used to really like and I was surprised how unappealing the taste was, it is just way to strong. Similarly with various sweets. I used to like all the kinds of chocolate bars and whatnot that one can buy in a supermarket, but when I try them now, they are just way too sweet for me – this is probably why I came to like marzipan instead.
These are not really any actual data but still I wonder whether simply cooking yourself from basic ingredients might not be a big part of it. I generally only buy milk, yogurt, cheese, eggs, (raw) meat, bread/pasta/oatmeal/rice/stuff like that, vegetables and spices when I go shopping (and sometimes beer or wine when I’m cooking something that goes well with it). The closest to processed foods that I buy is pasta and canned tomatoes. Maybe a part of it is the fact that I actually have to cook it and that generally goes against my laziness, but the change of taste that I noticed is interesting. Maybe when you get used to food whose taste is not cranked up to 11, the food whose taste is begins to be just too much. On the other hand, I sort of like putting salt on lemons and just licking that (although I don’t do it all that often), which is about as much as you can amplify salt+sour (I’ve always liked almost anything that tastes sour though).
Great post, Scott.
Anecdote: I lost 80+ pounds over a year on a diet which included 10 fast food meals a week (Egg McMuffins and the occasional chicken sandwich). I gained 15 of it back, but I’m stable here.
It wasn’t hard. Almost everyone who does this when it’s hard fails. I managed to reset my hunger set point by (cutting out artificial sweeteners/magic/willpower/something) and I stopped eating dinner entirely for a long time. (I now snack on veggies or junk food for dinner; if junk, small amounts.)
JRM’s Miracle Diet would, I am sure, sell a lot of books. I doubt it would work for very many people. Things I do think are important, while I’m here:
1. If moderation doesn’t work and you’re a big fat person, try not-moderation.
2. The first rule of Diet Club is don’t talk about Diet Club until people are asking you if you are dying. Then you’ve gone far enough to talk about it. There are clear psychological harms in talking about it before then.
3. Once you get to the talking point, don’t let people tell you you look too thin. They should probably be punched, but if that is illegal in your jurisdiction, do tell them to sod off.
4. Find something that works and is sustainable. If you’re miserable all the time on whatever you are doing, don’t do that.
5. Bariatric surgery (which I did not do, though many people thought I did because I disappeared for two weeks then dropped a mountain of weight) is not shameful. Do what works.
My experience is contra the book’s advice in a lot of ways. But it worked for me. And I still suspect the author is probably right about most or all of it. Hunger set point was certainly a real thing for me.
JRM
Long time lurker, first time poster. Former obesity researcher in Kevin Hall’s lab at the NIH. He’s one of the most well-known obesity researchers who does both detailed mathematical simulations, as well as experiments. In a spat with Taubes since his results didn’t confirm the insulin hypothesis. I’m a co-author on a paper with Hall, and I coded up the initial version of the NIH Body Weight Simulator. Now finishing up a PhD in Computational Biology.
Couple things.
1. You’re mental picture of the ice cream cone is completely off- Hall (and others) have tried to dispel the 3500 calories per pound rule for a long time. Your body is an energy reservoir, so what matters is the long term average flow rates. A one-time bump literally does nothing to your equilibrium state. You can think of it like this- when you add to your body weight, you’re also increasing your RMR, and the energy cost of your normal activity (since you’re heavier). This will over time remove anything in excess of your average intake. At equilibrium, Carson Chow (another co-author) has worked out that a PERMANENT increase of 100 calories to your diet adds about 10 pounds.
Links:
https://sciencehouse.wordpress.com/2010/03/04/obesity-weight-gain-and-a-cookie/
http://calorielab.com/news/2012/05/21/the-new-diet-math/
2. In terms of the options you present, I believe it’s closest to a combination of 2 and 3- you won’t notice the change, and it doesn’t matter. HOWEVER, if your eating habits change to alter your long-term average caloric intake, then the picture changes. See details above.
3. Related to the above, humans appetite is actually quite sensitively tuned in general. The “low grade damage” manifests itself in that over long periods of time, it seems like people who become obese are slightly (~10 calories) above their burn rate- CONSISTENTLY. Thus they are slowly driven upwards, instead of equilibrating at a 1lb heavier (per the math above). This doesn’t obviously deal with child obesity- but Hall and Chow have another paper on that:
Paper:https://sciencehouse.wordpress.com/2013/08/01/new-paper-on-childhood-growth-and-obesity/
https://sciencehouse.wordpress.com/2015/09/10/paper-on-the-effect-of-food-intake-fluctuations-on-body-weight/
4. More of Carson’s commentary on Taubes:
https://sciencehouse.wordpress.com/2015/08/13/a-calorie-is-a-calorie-more-or-less-after-all/
https://sciencehouse.wordpress.com/2016/07/06/low-carb-diet-study-paper-finally-out/
https://sciencehouse.wordpress.com/2015/09/09/the-world-of-gary-taubes/
5. Last point- the dynamics of body weight are such that if you make a permanent intervention, and never deviate, it may take you 1-3 years to fully stabilize- much longer than most people think about. And that’s with no fluctuations! Thus you should work to ensure that whatever you set out to do is sustainable.
Shameless plugs:
https://www.niddk.nih.gov/health-information/health-topics/weight-control/body-weight-planner/Pages/bwp.aspx
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3880593/
One thing that I’ve noticed about diets: people tend to (try to) lose weight on the margins of their lifestyles. They add this or subtract that, but mostly they don’t want to change their lifestyles to accommodate the change in weight. I met a guy on Kilimanjaro and when we reached the bottom and were celebrating with a few beers, he told me he was celebrating losing a bunch of weight. 100lbs or something. I said that’s really great, your new lifestyle must have been hard on your relationships. He got kind of sad. His sister confirmed the overall lifestyle change, including generally, a new support system.
This probably says something about the average weight of a culture. The Western diet is symptomatic of the Western lifestyle – prepackaged and convenient for the busy bee, nevermind that you’ll eat yourself prediabetic. All your friends will be prediabetic too! Somewhere up thread Sailer noted that food was a lot harder to make in the 70’s. People should try and make food difficult again.
I’m thin and smug and eat mostly bland food. But I have good genes and stuff.
Mealsquares are great. They aren’t delicious like a cheeseburger is delicious, but they’re tasty enough that I never mind eating one even though I’m a fatty that loves food. Thanks for reminding me to get more!
For completeness, here’s Gary Taubes on Leptin:
The late Seth Roberts, who was a psychologist at UC Berkeley, developed a diet that was based on breaking the link between flavor and calories. He called it the Shangri La diet (see also this longer article). The diet involves the consumption of flavorless calories (in the form of oil or sugar water) between meals. The flavorless calories act to suppress your appetite.
I tested the diet by performing an n=1 experiment on myself, weighing myself daily for 8-plus years. I found that the diet worked reasonably well. My story and results are outlined here. I’m still following the diet.
Edit: I skimmed Scott’s blog post and missed the part where he mentioned the Shangri La diet. Mea culpa.
The Shangi-La diet is discussed in Scott’s post.
Strange that nobody mentioned the “Selfish Brain” theory that describes how human brain regulating energy fluxes in the organism with itself as highest priority consumer. From Wikipedia:
The German WP page has more details on how a low-reactive stress system is involved in adipositas, societal and individual aspects, and on treatment approaches.
Let’s go back to first principles. Why are we as a society worried so much about diet? Because we have an “epidemic of obesity”. Why is obesity bad? There are two possible answers: (1) obesity is correlated with various negative health conditions, and (2) most people in our society find obesity aesthetically unpleasing. I can’t shake the feeling that, while a lot of lip service is paid to (1), the focus on diet and obesity is often really driven by (2). The current BMI standards are a case in point: A BMI of 25-30 is considered “overweight”, but people with BMIs in that range actually have longer lifespans than those who are “normal weight” (BMI 30). Why is that? If 25-30 is the healthiest range then shouldn’t it be considered “normal” and lower figures be considered “underweight”? Unless this is really, to some extent, an aesthetic (and moral) judgment masquerading as impartial medical advice.
Perhaps we should reconsider whether diet is really the low-hanging fruit when it comes to improving health outcomes in America. Would it make more sense to focus on exercise instead? We have a great deal of evidence that exercise is very important. Excessive sedentarism has been shown to have various negative health effects. There are studies showing that people who exercise regularly, even if they don’t lose weight as a result, generally have better health outcomes. Other studies show that even exercising once a week provides noticeable benefits over not doing so at all. Intuitively, it seems that it would be much easier to convince Americans to exercise more (keeping in mind that any exercise is better than none) than to convince Americans to eat less (or “healthier”) foods. Are we unwittingly making things worse by focusing on diet (which the facts indicate most Americans cannot effectively change) rather than exercise (which there is some reason to believe they can)? Are we inculcating learned helplessness with a plethora of failed diets?
No, you have to stop trusting the media. Read the papers yourself, the media lies about what’s in them.
AFAIK, the “overweight extends lifespan” thing is an artifact of the fact that people tend to lose weight before they die because they are ill. For example, let’s say we have two 75-year-old guys with BMIs of 28. One of them gets cancer, loses weight until his BMI is 20 and then dies. The other guy doesn’t get cancer and survives, but this does not mean that his high BMI is protective.
Right. On his blog Guyenet wrote about two papers that look into just that.
Once you control for smokers (who tend to be skinny) and folks who are sick you get an optimal healthy BMI of 20-22.
Here is Guyenet
In all subjects, as well as current smokers, the lowest mortality level occurred at a body mass index (BMI) of 25, which is on the cusp of overweight. Yet among people who have never smoked, the optimal BMI was 23-24. Among people who had never smoked and who were healthy at baseline, the optimal BMI was 22-23. And among people who had never smoked and were followed up for at least 20 years, the optimal BMI was 20-22! That is quite lean.
The last analysis is a particularly powerful way of avoiding confounding due to existing illness. If you’re recording a person’s weight right now and their risk of death in 20 years, it’s likely that whatever kills them in 20 years is not impacting their weight right now. So you get a cleaner assessment of the impact of BMI on health. This assessment shows that it’s much more dangerous to be obese than to be underweight. You can see that in this graph of BMI vs. mortality from the paper:
http://wholehealthsource.blogspot.com/2016/06/two-huge-new-studies-further-undermine.html
Does anyone know what the ‘relative risk’ measurement they’re using actually means? I have no sense of whether increasing my relative risk of mortality from 1 to 1.5 is something that should be very concerning to me.
Increasing all-cause mortality by 50% takes 4 years off of your life. The opposite, reducing mortality by 1/3, adds 4 years. A Graph from here.
Perhaps this is a silly question, but does a 50% increase in mortality mean going from 1% to 51%, or from 1% to 1.5%?
Relative risk is a ratio.
I thought part of the effect was that people lose weight as a result of cancer, and fat people are more likely to have enough reserves to survive.
Another data point to look into–the diet that got Penn Jillette to lose a massive amount of weight started with two weeks of nothing but unseasoned potatoes. This fits extremely well with the “bland food” hypothesis, and makes me think there’s something there worth trying.
Penn Jillette’s story is really unusual. Possibly he lucked into a first diet that suited him. Possibly his point that sometimes magic takes putting in more work than a normal person can imagine putting into a trick indicates that he has very high conscientiousness, and that made a rather extreme diet easier for him than it would be for most people.
Penn lost weight following Ray Cronise’s advice regimen (which includes: start with a bland food as a reset then eat only unprocessed plant foods with no salt or sugar or meat or oil other than in a “rare and appropriate” context, avoid exercise until you reach your goal weight, subject yourself to mild cold exposure, have a narrow “fed window”). When he did so, two of Penn’s friends (his podcast co-hosts on “Penn’s Sunday School”) did the same thing at about the same time and of that n=3 sample set, one has apparently already (in less than a year) gained back at least half the weight lost – it was too hard to keep to the diet. (He’s trying again, but it’s still very much a work in progress.)
When I saw the title of this post as an email notification, I thought it might be about appetite, but it might also be about the brain’s hunger for sensation which would also be an interesting topic.
How does methylphenadate (ritalin) function as an appetite suppressant? I wonder how it fits into this model.
I remember being distinctly disinterested in food as a youngster while medicated to the point that my neurologist sent me to a dietician who recommended 2 strips of bacon and a bagel with peanut butter every morning to get me back on the right height-weight curve. The medication didn’t affect my appetite until well into the morning (I had trouble eating lunch).
Ritalin is a strong stimulant (similar to adderall, which is basically an amphetamine). Stimulants generally suppress appetite and increase energy output, so are common ingredients in weight loss drugs (caffeine, ephedra, etc.). This is also why college students abuse it to help them study.
My understanding is that stimulants have a paradoxical calming effect on people with ADHD, however.
I haven’t noticed caffeine having a calming effect, but the ritalin could be described that way. I would describe the feeling as as increased impulse control, or a decrease in my desire to act on every thought that entered my mind and an increase in attentiveness to the task at hand.
I am familiar with the appetite suppression properties of stimulants, but I was wondering specifically how the stimulants link into (hijack) a possible leptin feedback loop, or if there is another method through which they have this effect that has been studied.
A lot here, and I can’t say I’m surprised at the conclusion: Either you’re going to be fat, you’re going to be hungry, or you’re going to have to miss out on tasty food.
I’m 5’7″, and I’ve been as high as 170lb (many years ago) and as low as just under 140. I try to keep it under 150 (except when I’m doing a lot of exercise) but in general this means I’m hungry much of the time (in the Western “I want food, I’m getting a headache and feeling out of energy” sense, not true hunger). If someone would come up with a drug which caused the body to not do that and instead just burn some fat between meals, I would be very gratified (and I imagine a lot of dieters would succeed where they would otherwise fail)
I think CICO must be correct, but CO = some horrible differential equation with state variables and including CI as a parameter. The paragraph describing how increased food intake since 1980 explains the obesity seems to confirm a stronger CICO; even if there are people who can eat a lot more and not gain, a change in this mechanism doesn’t explain the increase.
The part about the “buffet effect” makes me want to dance around and yell “in your face, nutritionists”. Always they tell you to have a “balanced” diet, and it turns out this is the worst thing for you. You can’t “balance” a delicious saturated-fat-filled steak by also having a side of kale cooked in olive oil; that just makes it worse. Just eat the steak (or the kale… more steak for me)
Does the book ever come up with an explanation for the change at 1980? I can’t see how Reagan is responsible. The much-maligned Oreo was introduced in 1912. Doritos in 1964. Potato chips in 1817, though bagged ones in the mid-20th century. So what happened in 1980?
I think the balanced diet is more to ensure that you get a wide variety of nutrients and aren’t exposed to much danger if it turns out that one particular food is unhealthy for some reason. I’m not sure that’s intended as weight loss advice.
I load balance between missing tasty food and acclimatizing myself to moderate hunger. I don’t have tasty food in the house ever and I have a disinclination to going out to eat. I also fast once a month with a longer one once a year which seems to reset my hedonic treadmill.
Not fat, not hungry, eat as much as I want of tasty food. Genetic privilege really does exist and we skinny people are not all going about counting calories or refusing to eat Skittles.
Is there any evidence that when someone on a diet plateaus their weight loss, the problem is greater efficiency at using what comes in, vice the more common explanation of a starvation mode?
I have a different perspective on Calories In – Calories Out = Weight Loss. I rearranged the equation as Calories In (from nutrition labels/bomb calorimeter data) – Weight Loss = Something Caloric.
I injured my knee a couple of years ago such that I did no excercise for a 6 week period. I had recently purchased a scale for my new apartment and used the opportunity to try to find what was my Total Daily Energy Expenditure (called Something Caloric in the above equation). I ate approximately 1950 calories every day. My diet was frozen vegetables, chicken, eggs, almonds, spinach, ranch dressing, cheese, Greek yogurt, fruit. I lost about 1.5 lbs a week. I was able to back calculate Something Caloric as about 2700 calories.
I thought at the time that was my TDEE, but now I realize any differences in my real Calories In from what the nutritional labels claimed is also built in, so some other label (Something Caloric) is appropriate. After I had gone from 185 to ~176 I plateaued and then a couple of weeks later fell of the wagon, stopped calorie counting, and quickly went back to 185. Overtime I fell out of good eating habits and rose to about 205 as of a month and change ago. I started using beeminder to set a 2000 calorie limit and started calorie counting again, and am now down to 195. Plotting the linear trend line on my weight shows a loss of about 1.4 lbs a week. This pretty much still lines up with 2700 lbs, so for at least some narrow range of weights I have a good handle on something. When I plateaued at 176 I assumed it was a starvation response, but it could have been a difference in how my body processed what I ate.
So I still find the laws of thermodynamics slightly useful, even if breaking the three components down farther than temporary averages is intractable.
There are multiple different ways of breaking down diets in terms of quantity, quality, macronutrients, and timing; if one diet doesn’t work for you, It is better to switch up and try something else until it works. If low carb doesn’t work, try going full vegan, or go the other way to ketosis. My personal combination that got me from 270 to 185 was low carb, intermittent fasting, absolutely no chocolate or fast food, mostly no other processed/hyperpalatables, p90x, and daily weigh-ins. YMMV.
I think what I most appreciate about what The Hungry Brain has to say (based on the above review) is the link between the basic calories-in-calories-out theory and the body weight set point theory. My problem with the natural set point theory is that it struggles to explain why obesity has risen so significantly in the last 50 years in just about every country that has adopted a western diet and lifestyle. America isn’t even in the top 10 worldwide for obesity any more, so it isn’t a uniquely US problem. The UK is infamous for bland food and yet is not far behind America in obesity (could simply be a different definition of bland though)
The implication from set point theory is that, until the last 50 or so years, millions of people thought they were starving to death their whole lives because their body’s idea of a healthy calorie intake was set higher than could realistically be achieved. Their descendants, inheriting the genetic basis for that set point, could just gorge on McDonalds and so all weigh the 300lbs their body thinks is healthy…. This seems unlikely (and as far as I’m aware, historical records don’t document this). Yet I could believe that greater exposure to calorie-rich foods in childhood could alter the set point – a lot of obese people seem to report being made to eat huge portions as children, or eating junk food more often. Maybe parent will-power is the key?
Another data point. I am about 73.5 inches tall and 66 years old.
My weight has varied a significant amount through my adult life. For a year or two I would gain some weight (perhaps 20 lbs) and then (when I was willing to be hungry) would eliminate it by eating less and exercising more. It gradually got harder, and 15 or 20 years ago it started to rise more. About 5 years ago I weighed 270 lbs and was taking medication to reduce my blood pressure and triglycerides. I was basically following the food pyramid (lots of whole grains and vegetables, modest amounts of fat and protein). I ate very little processed snack foods or meals (now and then a pizza). I ate less than I wanted and told my friends that I was always hungry (which was only a slight exaggeration). On my last check up, my blood glucose was slightly above normal.
At this point I read Good Calories Bad Calories. It seemed to make sense, so I decided to try eliminating almost all carbohydrates and eating all I wanted of other foods. It worked very well for me, and I ended up reading a number of books on diet (such as by Atkins). In about a year and a half I had lost about 70 lbs, had very little hunger, and was off the blood pressure and triglyceride medications. (Some of the reduce blood pressure was probably due to increased exercise, but I lost at least 40 lbs before exercising much.)
Getting to 190 lbs took a little effort and hunger. Getting to 180 lbs took a lot of effort and hunger, and I quickly went back to 190 lbs once I stopped trying. For the last several years I have stayed between 190 and 200 lbs without doing much.
I have reserved The Hungry Brain from my library. Maybe I’ll get a few ideas. (I’d like to lose another 20 lbs or so, but don’t want to be constantly hungry.)
From pharma perspective, an agonist or positive allosteric modulator of leptin receptor would be an excellent remedy for obesity. Unfortunately, this receptor belongs to an almost undruggable family of cytokine receptors. It is very different from conventional CNS targets such as GPCRs, ion channels, transporters etc. Quick search gave only a couple of interleukine receptors antagonists. Interleukin receptors are related to leptin receptors, which is both a bad thing (because their inadvertent activation could trigger massive inflammatory response) and a good thing (because making an antagonist of OB-R is just a few steps away from making antagonist of IL-5 R). However, making an agonist or positive allosteric modulator in general is much harder than making an antagonist – there are much more ways to break a receptor than to force its activation. So I guess anti-obesity drugs utilizing leptin pathway are still far away.
There’s a fun connection between the “food reward” hypothesis and inflammation that would be interesting to explore. It sounds like Guyenet (and most people who discuss inflammatory responses) think of it in terms of blood sugar or blood lipids increasing inflammatory response. Which is probably a major factor, but there’s also evidence that activation of the reward system itself increases immune responsiveness. The researchers involved were thinking about the placebo effect and mood disorders rather than weight change, but it’s a nifty connection.
It doesn’t seem plausible that the rewardingness of food itself causes obesity through this pathway (in part because that suggests that *any* rewarding stimulus should contribute to obesity), but it does suggest that people who find food more rewarding may also have the greatest increase in immune reactivity after consuming it. If inflammation plays a part in the development obesity and/or metabolic syndrome, this response seems like it could exacerbate that process.
For a long time I have assumed that one of the ways our bodies modulate weight is by adjusting what I will call “digestive efficiency”. I don’t really have much education in this area so this could possibly be easily proven wrong by somebody with more domain knowledge in nutrition than I, but nonetheless I am inclined to believe that this is at least partly true for some nutrients. The idea is this: If I eat 100 units of some nutrient, my body will only actually absorb maybe 70 units of that nutrient with the other 30 units being simply passed through the colon and released. But if my body somehow senses that I am deficient in that type of nutrient for some reason, it can choose to invest extra effort and absorb maybe 90 out of 100 units of that nutrient. (like produce higher levels of enzyme related to digesting that nutrient, or stimulating growth of a gut bacteria that assists in digesting that nutrient, or directing extra resources to the type of cell in the small intestine that absorbs that type of nutrient). Likewise, the body can reduce its digestion efficiency if it senses that it has a surplus of that nutrient. If this were true, it would really help smooth long term weight gain from local variations in food consumption. If different people have different set points for digestive efficiency this could also help explain differences between people.
I’ve been thinking about this too. I wonder if some thin people have less efficient digestive systems, and can thus consume a lot of calories without actually absorbing that many. One of my friends growing up ate tons of really unhealthy, calorie-laden food (pizza, chicken nuggets, burgers, chips, soda, etc) and always remained on the edge of looking anorexic. She also never exercised. But when I and most of our other friends ate the same way, we gained a lot of weight.
Was her digestive system simply not processing the food as efficiently? I don’t know the answer, but it’d be good to find out if this is possible.
One possibility, not the only one obviously, is bulimia.
I heard a guy complain that he needed to eat a lot while being thin, and he kept losing girlfriends because they were dieting and found it hard to see him do that.
One of the other guys at the table tore one layer off a napkin, and asked to drape it over the first guys hand. The napkin layer was enough to make a tiny fast tremor visible, and that’s a symptom of hyperthyroidism.
I don’t have a follow-up for the story so far as hyperthyroidism goes, but he did eventually get married.
I’ve gone up and down in weight. I’ve noticed the pattern that when I’m not trying, I go back to a normal upper limit.
I think once you’ve eaten the food that breaks lipostat feedback, your body stores the extra calories as fat. If you heal the lipostat feedback, you lose weight when your body needs energy and is willing to release fat stores. You keep losing weight until your fat cells become completely deflated, but they don’t die. Then, when you run a calorie deficit, your body sends a different signal that says the fat stores are empty, and you feel hunger from a new source, or maybe satisfaction from restoring your existing fat cells. That makes you hungry enough to refill the fat stores.
Regarding MealSquares: I’ve been curious to try them for a while now, but they don’t ship outside of the US “while they are in beta”. That doesn’t sound unreasonable, but the problem is that they’ve been saying that since I know of them, about 2 years I think. Does anybody know if they have plans to ever ship outside the US?
It turns out to be crazy expensive. Contact us via our website if you’d like to place a bulk order that ameliorates the unit cost somewhat.
What if you made them in China and took advantage of whatever allows the Chinese to have free international shipping?
It’s not free, they just ship containers full of products. Also, shipping companies employ huge ships between China and the US, so a fairly small crew is able to move a lot of containers.
Shipping to China is actually cheaper because there is less demand for transportation that way.
It’s possible to buy individual containers and get them shipped by container ship for, IIRC, somewhere in the single-digit thousands of dollars in total. I know people that have successfully imported fairly obscure goods that way, for a fairly small business. But for that to be economical for Romeo, he’d need to be shipping thousands of Mealsquares (tens of thousands, more likely) and they’d need to be shelf-stable enough to survive the voyage (no idea).
I meant free for the customer. If you buy random stuff from ebay, it’s very often free shipping from China.
@Anonymous
The production costs of your products and the shipping tend to be really low compared to the price you pay in the store. The markup is huge.
Free shipping is not free, it’s just part of the markup.
This does explain your excitement about genetics, but the history of the last couple of centuries makes me incredibly skeptical about the idea that genetic explanations will actually somehow help us to accept that people are actually wildly different.
To use an example from one of your earlier links on gender differences, maybe women are genetically, evolutionarily pre-disposed to liking more empathetic play.
It seems to me that the people who believe this have a couple of reactions when they see a woman who likes soccer:
“Genetically, women don’t like soccer, so you must be mistaken when you say you enjoy it” or, as a slightly more sophisticated dismissal, “Women are pre-disposed not to like sports. You might be an outlier, but we can’t be spending our precious resources on women’s sports just to satisfy some tiny minority, when there are a bunch of normal women out there who would be better served by taking home ec classes.”
“Gosh, it would sure be interesting if black people and white people had the same intellectual potential, but science clearly shows they don’t, and pretending like all people are the same and benefit from the same things will just end up breaking society” was an idea that has heavily influenced our treatment of race in the US for most of our history.
History shows pretty conclusively that it is very, very easy for people to take genetic explanations seriously, while still dismissing the importance of outliers, weirdoes, and personal experience. Frequently, genes are used as an excuse to dismiss or ignore lived experiences.
Really, the problem is that people, upon finding out that a character trait is genetic, don’t come to the rational conclusion that the trait should not have moral import, but instead conclude that people possessing the innate character trait are just innately immoral. It took massive amounts of activism and social disapproval to get as far as we have on homosexuality, and no other character trait has gotten that level of attention with that approach.
To tie SSC threads together, this is part of why Charles Murray gets so demonized. His position can be summarized as “some populations genetically trend to lower intelligence or self-control, and therefore we should not treat those differences as indicating morality and should make policy to help people who are genetically disadvantaged. Without grasping that second part, people read “there are differences in intelligence among racial populations” as “black people are less intelligent, less intelligence is bad, so black people are bad.”
One more point in regards to fatness and perceived self-control. There are fat people who do difficult things like getting advanced degrees or finishing triathelons. Culturally speaking, those things DO NOT COUNT compared to being thin.
Depending on the culture, they may count in principle but not be known until a first impression has been firmly established. To the extent that obesity is seen as a moral failing, with or without the possibility of compensatory virtue, it’s right up there with blackness (and very little else) as a “moral failing” that cannot be concealed from would-be critics.
We are, at least in English speaking society, incredibly inconsistent on this point.
It has been very weird for me to watch it become dogma that homosexuality is innate, and therefore cannot, and should not be changed. Because I grew up with people working to break the stigma around mental illness, working to convince people that, say, depression was innate, and therefore it was our obligation to find compassionate ways to change it.
Or, look at the common sentiment of “Boys will be boys”; it is a common idea that boys and men have outsized appetites for sex and violence which they can’t really help or be expected to control, and that, therefore, when they indulge those appetites at the expense of others, those others should quietly tolerate it, because blaming those boys for their innate proclivities would be unfair to them.
Another group of people who in the American imagination have outsized appetites for sex and violence that they can’t really help or be expected to control are black people, but, curiously enough, Americans never really took the attitude that “black people will be black people”; instead, it was considered immoral to allow those appetites to impinge on our society, and we built an enormous, monstrous program of control over black people, which began to perpetuate itself by saying, as I went into above, that essentially black people weren’t capable of existing outside of that system of control.
To lose slavery, or segregation, would be to set anarchy upon the US, as people with an innate drive towards bad behavior would be allowed to fruitlessly indulge in it until the country was a wreck.
Which in a roundabout way leads me to this:
I don’t think that is the only objection that animates people. There is also the fact of, well, all of American history.
The idea that certain people are “genetically disadvantaged” is extremely compatible with all kinds of Brave New Woirld style atrocities.
The idea of genetic disadvantage is fully compatible with many of the more sophisticated moral arguments for US style slavery, which was often cast as a kind of uplift; the innately advantaged white man shared as much of his advantage with the black man as the black man was capable of handling, while using his innate self-control to protect the black man from the worst consequences of his innate wildness and destructiveness.
And if, after all that, the black man still claimed to be miserable? Well, there’s always whips and hot irons.
That dynamic has played out, again and again, throughout the last two centuries. The communist dictatorships had a similar thought process, although the groups were different.
I think it is very reasonable to be extremely on guard against anything that would justify that dynamic once again.
It makes perfect sense to be on guard, yes. This doesn’t justify refusal to look at nuance when it’s offered – just to be very careful about it. So when Murray states along the lines of “some populations genetically trend to lower intelligence or self-control, and therefore we should not treat those differences as indicating morality and should make policy to help people who are genetically disadvantaged,” the person who is properly on guard would engage with that statement in whole and acknowledge that the latter portion is just as important part of his position as the former portion.
(taking this as a high-school thing because colleges mostly don’t have home ec and high schools mostly don’t have women students)
This seems needlessly negative. I’d say something like “if you can get enough girls to field a soccer team year after year, we’ll start one.” What I’d leave unsaid are my expectations that there’d probably be fewer girls who’d sign up for soccer than they would for home ec. Of course, if a given school has enough girls who’re interested in soccer to play as a team together, that’s great. More people getting their harmless preferences fulfilled, modulo ACL tears.
The dismissal of the “willpower theory” is really bad. First, obviously mice don’t have willpower the way we do. So you can’t test willpower-theories of diet on rats. Second, the existence of chemicals and lipostats and bla bla bla don’t disprove willpower theories. In fact it would be very strange if there were brain-processes that had no chemical counterpart. Maybe you believe that willpower doesn’t exist at all and everything is just chemicals, but if the willpower theory were true it would likely be used to explain variation in brain chemistry. For example, being strong-willed would explain why someone didn’t exhibit a broken lipostat the same way that being a clean person explains why your room isn’t messy.
Not that I specifically believe any of that.
What I do believe is that human differences can be attributed to the fact that humans are metagamers. I am not aware of any formal body of literature or communities who discuss this. But humans are biologically and culturally programmed to diversify their skillsets. The reason not everyone tries to become captain of the football team is because this drastically increases the number of “losers” in society. No one cares who the 5th best football player at your high school is. So some people least-able to be alpha-male-football-dude apply to medical school, or law school, or play baseball, etc, and achieve high-status and/or resource-rich positions elsewhere.
This fetish for metagaming is apparent in fantasy RPG tropes with burly warriors, nerdy wizards, and streetsmart rogues. An equal combination of which is needed on any adventure in the fantasy genre.
When questioned about their metagame position, people will say: “oh it’s just my preference”. But this is question-begging because it does not explain how they arrived at their preference or explain why human beings even have heterogeneity of preferences. However it makes sense from a game-theoretic perspective for us to diversify and exploit status ambiguity effects (is a good basketball player any better or worse than a good musician?). Of course we all have opinions about whether such and such careers are “fake”. For example, lawyers are universally derided. But the next time you ask some social justice warrior why they dyed their hair a pale shade of pink, consider that “I just like it”, is a really lousy explanation, and that their desire to shirk social conformity by mutilating their appearance is part of their metagaming algorithm.
Metagaming applies in many subtle ways to the body fat debate. The most obvious is that some people are normal build, but are at risk of dying during famines or diseases. So biology produces “insurance” against starvation by having X% of the population carry extra body mass, at the cost of being less attractive and less mobile. But the whole thing is very complicated because obesity has many effects on physical attractiveness, physical intimidation, etc etc. Back to fantasy tropes, there are jolly fat guys and mean greedy fat guys, both of which incorporate body mass into their metagame choice.
Regardless, getting people to change their weight is likely the same as getting them to change their metagame archetype. Asking why fat people don’t just diet and become thin is like asking why don’t bus drivers just go to college and become doctors. It’s thermodynamically possible but people still don’t do it. Hence the 99% failure to maintain weight loss.
Anyway, I don’t expect anyone to take this seriously. My hope is that there’s just a large body of literature out there discussing this in much more concrete terms that I can be pointed to.
There is some supporting evidence for willpower, anyway: https://www.ncbi.nlm.nih.gov/pubmed/16819526
Not sure if the authors in the OP addressed this, but if not, they should.
What you call metagaming would probably more often be called specialisation, and most likely to be discussed (and praised) by economists.
And this model doesn’t seem to explain the obesity epidemic well at all. Specialising in being fat is both a terrible strategy and becoming more and more saturated.
So you make two points. First, that being fat is a bad strategy. Here’s a very partial list of benefits obesity has for normal people:
1) People expect less of you (slow, stupid, among other fleetingly accurate stereotypes)
2) People feel less threatened by you
3) The fat-pact is a more stable relationship in certain circumstances. It is especially useful to have low sex drive and ambition when you’re poor and living in a dirty neighborhood. Why would your sphere leave you for another sphere? And your sphere can’t leave you for the middle class suburbs because they’re indistinguishably bottom of the barrel. The mere fact that you live at the same residence and seem to get along produces more stability than trying to lose weight and compete for attractive mates.
Conversely, the mainstream assumption is that it’s always better to be more attractive. But being attractive means you can’t make a credible mate for unattractive and low-status people. You have to actively leverage your attractiveness and play this game https://putanumonit.com/2016/02/03/015-dating_1/ And if you play it wrong and wind up in an unstable relationship, you waste a ton of time and resources trying to recoup in your mid 30s.
Second, you say that there are already lots of fat people, so “diversity” arguments are unpersuasive. I agree that we are reducing the standard deviation in body types, but it seems like we’re improving the top 1% of the spectrum (instagram models, male physique competitors, etc) while the average person deteriorates. My hypothesis is that status drops off precipitously with ranking. I’ll use strength as an example. The status of the world’s strongest man is significantly higher than the 7th strongest man (who no one can name). It’s good to be the fittest guy in your crossfit box, but no one knows or cares who the 4th fittest guy is. And even the fittest guy in your crossfit box, you know in your heart of hearts, is a wuss, because you watch crossfit on TV and see dozens of people who could murder him. Is your local guy high status now?
How this relates to an increase in the obesity metagame is that society used to be close-knit, to where being the strongest guy in your village made you #alpha. Now we have youtube and social media showing you that your strong neighbor is actually mediocre. We have the radio and spotify showing you that the best local band is a bug compared to multi-platinum artists.
About the only thing left that can get you status without necessarily being ranked is money. Such that that nth best doctor is still really useful at boosting your social value. But to become a doctor you still have to compete and be “the best” in a relatively large pool of applicants. So a similar logic applies to why most people don’t even try to compete in the first place.
TLDR – the space at the top has shrunk dramatically. So rather than queue up and be the 18978th strongest man, which doesn’t mean anything anymore, people embrace mediocrity and play the losers’ metagame.
I think that you’re underestimating the amount of things that can boost your status without being explicitly ranked. Even if there are thousands of people on Instagram who are way more shredded than you, having nice abs is still a pretty strong status booster. Similarly, being able to play popular music will boost your status in many scenarios, even if you’re just some random guy with a guitar.
I lift weights, and my best deadlift is approximately 50% of the world record. Even though that’s pretty mediocre among serious lifters, it’s enough to give me some ‘gym status’ in a typical gym, to the extent that such a thing exists.
Disagree strongly. They might boost your status when you’re still a kid in college, but eventually people get over the initial novelty of guitar-ab-guy, ask where he’s going, and the answer is nowhere special. The girls are all watching the guy who has a 4.0 and goes to work at Exxon out of the corner of their eyes.
You mean you pull 600 lbs? Or something more nuanced like within a weight class, or powerlifting fed. And I assume raw. If you use straps don’t bother replying >:(
Regardless, between 400 and 600 lbs is quite a bit more than most gym casuals will attempt. But in my experience commercial gyms are microcosms of denial. They don’t reflect the real world and everybody in them is trying as hard as possible to “be real” without doing any real work (see all the half squats and guys who can’t bench anymore cus their shoulder but oh hey I used to bench 405…). No one’s body changes over time and the fact that the strongest guy in the gym gets credit from all the losers in the gym doesn’t extrapolate.
p.s. I’m the strongest guy in my shitty commercial-ish gym and I get no status whatsoever because my existence is proof that everyone else is doing it wrong. They just want to half squat and post “day after leg day” memes lololol.
I have a friend at this gym who gave up strength training and is trying to get abs. I don’t know what he thinks he’ll accomplish. A more attractive mate? Maybe marginally. But it’s a myth that hot girls date hot guys. Most hot girls date high status/wealthy guys. The rate of return on abs for a grown man is quite small.
Personally I love abs though and think they should be prized more. I’m just summarizing what I think everyone else’s opinion is.
Don’t know where you went to school or when, but that’s not how I remember it from Mediocre State. Guitar guy always did well, 4.0 guy… who is he? (the computer lab rats were of course beneath notice, unless they had a guitar)
I’m sure a Goldman-Sachs expense account helps, but don’t forget height. Height always matters.
They’ll notice the 4.0 guys. Ten years later.
Which counts for something, for sure, but that can be a long wait.
UT Austin. Recently.
I’m not talking about the otaku class nerds. They don’t go work for Exxon. I’m talking about the guys who get 4.0’s and max out on internships and networking and…
Girls know who those guys are.
Too true.
Alpha f***s beta bucks? The red pill meme wants you to think young women are just gratuitous thotties min-maxing according to their SMV. In reality, attractive young women are consciously trying to predict who will come out on top and snag them early. Attractiveness is a competition, and is completely wasted sleeping around (which any moderately attractive woman can do just as easily). Plus fooling around reduces your SMV. Obviously rich men have their pick and don’t want the roasties.
I think I misunderstood “work for Exxon”. I thought you meant guys making a 4.0 and working long hours at the gas station to try to make ends meet. They existed (and were a separate class from the computer lab rats) but certainly weren’t noticed by hot women (not that they had the time to do anything about it).
Now I think you mean the guys with good social skills who go to work for Exxon in a white collar role right after college. They existed too, I had some roommates in that class. But it’s the good social skills (and the adequate-to-good looks), not the grades (which generally weren’t 4.0, but were good), that worked for them.
My experience differs from yours on this point, but I’m still in my twenties. Perhaps the relative importance of different factors changes with age.
My PR is 555, raw, no straps. It’s almost exactly 50% of the overall record if you count strapped strongman deadlifts; more like 55% of the record based on powerlifting competition. If we’re talking weight class, I think it’s 62% of the record (in the 220 class). As an aside, I do actually use straps now, since I’m not a competitive powerlifter, and I find that a mixed grip often aggravates an old back injury.
My perception is that it’s probably easier for a lot of people to significantly improve their attractiveness than to significantly improve their wealth/status. From my perspective, I see my life choices determining whether I’m going to be middle class or upper middle class, but probably not much beyond that. I’d have to screw up pretty badly to end up poor, and I’m exceedingly unlikely to break into the “rich enough to attract women just by being rich” tier. In terms of status, I’m not even sure I would know how to improve that in a noticeable way. However, I think I could reasonably end up at any attractiveness level between unkempt obese mess and fairly jacked, lean, and well-groomed. Maybe being attractive and in good shape isn’t as useful as being wealthy, but I think it’s a lot more achievable, at least for me.
Well I’m in my late 20’s so I can’t exactly offer a wealth of data you don’t have.
That’s pretty good! Would not have guessed the SSC comments section would represent so many standard deviations above the norm for physical strength.
Reconsider competitive powerlifting. I.e. showing up to meets and such. I don’t know how much you care about status and the jazz we’re talking about, but it elevates you from being a gym rat to someone who goes out and “does something real”. For example, nerd who squats in his garage vs. “omg is that the olympics??”
Are you sure about that? You’re only locked in if you do the college –> 9to5 job routine. If you’re willing to work long stressful hours you can work for an investment bank. Otherwise you could go to a good law school, pick the right field/firm, and be making low-mid six figures within 5 years. The path to wealth is fairly obvious. You just have to aim directly at it and also be willing to make costly up-front sacrifices.
I’m not willing at the moment, partially since I wasted 5.5 years of my life getting a doctoral degree playing manchild. But “what it would take” seems clear and achievable.
Or idk. Maybe you think earning $250,000/year is “upper middle class”. I don’t know. Getting legit rich in your 30s and 40s is something there’s no recipe for.
And that is exactly why it does not contribute much to status. Because some variant of “athletic” is easily achievable for almost everyone.
I would not advise anyone to count on this.
“you know, Donnie, nobody gives a damn about your squat”
(the entire Mopeilitywod archive is also a case in point)
Alpha f***s beta bucks? The red pill meme wants you to think
This has nothing to do with that. I came of age before all that crap. I believed that women would value long-term value. They do, but it takes, well, a long time.
Thank you! It’s important to balance out all the navel-gazing and philosophical discussion with picking up heavy pieces of metal.
I would like to compete, but recurrent injuries have held me back in the past. If I can ever get reasonably healthy, I’ll probably give it a go.
My honest self-assessment is that I don’t think I would be successful in those areas. I tend to function very badly if I don’t get enough sleep, and prolonged periods of high stress usually lead to me getting sick all the time. If I thought there was a higher chance of success, I might be inclined to try one of those paths.
I’ll also throw in some kudos. 550 is a damn respectable lift.
Now, you two are stronger than I am, so this has me wondering. A point that Scott brushed up against in the previous post that doesn’t get enough airtime is that effect size varies by population.
So, VolumeWarrior finds that strength and physical form don’t help much in terms of status, whereas I find the exact opposite. What is the economic situation like around where you live?
The reason I ask is because I currently live in an oil city that is absolutely flooded with money. Guys with 8th grade educations pulling in $100-250k/year aren’t uncommon here, and it’s unlike any other environment I’ve seen in the sense that rich people look like homeless rednecks. Around here there are a lot more guys making 100k+ gross than there are guys with solid abs. I could see the situation being reversed somewhere jobs are hard to come by and decent earnings are rare, all this essentially boiling down to comparative local advantage.
The status of the world’s strongest man is significantly higher than the 7th strongest man (who no one can name).
Nor do I know who the world’s strongest man is, nor care. I imagine only those interested in strength contests would know this immediately, and in that sphere doubtless being No. 7 (with the spur to work your way up to No. 1) is a big deal, since everyone is comparing themselves to everyone else competing to be World’s Strongest Man, and the fandom (I presume there is one, there’s a fandom for everything) is intense about “Is No. 7 really better than No. 8? Can he overtake No. 5?”.
But what is real about it? All this number quoting you do about lifting so many pounds of weight – what does it mean? How much work can you do? How strong are you really?
I mean, I can get an idea of strength from “can lift so many bales of hay in a day, can plough a field, lift a calf, chop this much wood” and so on – but gym muscles, even Olympic Gold Medal Weightlifting muscles, aren’t for anything but a highly artificial environment where the weights are created and stacked according to a system and there’s all the machinery for pulling and what have you, and the accompanying diets and whey powders and supplements and bulking up and cutting down and it’s all as false as the spray-on tan and hair extensions of models (or porn actresses, I may be getting confused here). It’s not muscles for working, it’s muscles for display.
I generally think men really into lifting etc. aren’t doing it for attractiveness to women (hence why you’re so dismissive about the guy no longer concentrating on ‘strength’ workouts but getting abs), they’re doing it for other men: not in a sexual attractiveness or even competitiveness way, but the same reason women go on drastic diets and worry about fashion: being judged by other women, held to standards of a certain circle or sphere of lifestyle, everyone having a standard that is deemed to be the most desirable and wanting to achieve that, and not really caring about the sexual appeal to the other gender (I imagine men, for instance, don’t give a damn about is a woman wearing this season’s or last season’s in-fashion shade of red lipstick).
Men who bulk up muscles for that fake gym strength are doing it for the approval of other men who are interested in that element of sport or appearance or whatever you’d call it.
Women like six-pack abs for the look of it and neither know nor care if you can benchpress 300 or 600 lbs.
And being able to benchpress by gym machinery 600 lbs means damn-all on “can you use that strength for hard physical labour as on a farm, oil rig or building site”.
As far as I can tell, weight lifting and bodybuilding are different subcultures, though both are very artificial.
Bodybuilding seems much weirder to me.
Maybe I’ve missed something, but I don’t think many people switch from one to the other.
Video of a weight lifter who wouldn’t stand a chance as a bodybuilder:
https://www.youtube.com/watch?v=nSV3sLjZqDk
Just for the record, there’s no machinery involved in the major lifting sports (powerlifting and weightlifting). There’s a bar with weights, and in some cases, there’s a rack that you take the bar out of before you lift. When I do a deadlift (one of the competitive lifts in powerlifting), I am literally just picking up a heavy piece of metal off the floor. I recognize that it’s easier to pick up a straight piece of metal than it is to pick up a bale of hay, but I think there’s a pretty strong correlation between people who can pick up heavy pieces of straight metal and people who can pick up heavy bales of hay.
Donnie was a pretty respectable bodybuilder back in the day, and I believe Mark has been on stage as well.
Not to rag on you too hard here, but I definitely notice a trend that a lot of the people who have ‘tried exercise and it just doesn’t work for me!’ sure take a lot of pride in not knowing anything about how to train.
As for tangible goals, you’d be surprised if you actually talked to some of these lifters. Funny that you mention porn actresses, because that’s exactly the field in which I lift to stay competitive. My “Real” work metric is that I expect myself to be able to lift any woman with whom I would consider sleeping/working over my head without having to strain so hard it interrupts my Swayze impression.
More seriously, during my day job as a paramedic I’m the one who has to frequently carry obese patients up and down flights of stairs. And one of the first things you learn on car is that skinny people don’t get sick. where I live (Which is in Canada, mind you, where our population is a little lighter than the states on average), city paramedics have a median career length on the ambulance of just under 5 years, with back injuries being the leading cause. I don’t actually know many current paramedics who don’t lift, because that’s just asking to get hurt.
I think you might be projecting some things onto a population you don’t really understand here.
Interesting. So even though being fat has adverse effects on health and well-being, none of those really matter in terms of genetic fitness? You’ll still be alive long enough for your grand-children to become adults, at which point you may as well die.
This strategy is also being selected subconsciously, since most fat people don’t like being fat very much.
Why is this a better strategy than being thin? There’s a huge space between apex physique and healthy, which is where almost everyone existed 70 years ago.
A strongman not being particularly attractive to women is pretty well-known in those groups. The understanding is most women desire the Brad Pitt in Fight Club look. Once people start thinking about getting into Olympic level bodybuilding, they’re not doing it to “be hot” anymore.
Why are women getting fat at the same rate as men? In terms of social status, being fat is way worse for women.
I suspect the answer to these question is: Playing the winners’ metagame is a lot harder than just being thin. Most people are too non-agentic to follow even basic rules like “include vegetables in your diet” let alone all the increasingly complex dating advice. So fat-pacting with another loser and creating a stable family of losers is a better strategy.
But this model still doesn’t seem to have any predictive power. This loser class should have existed 70 years ago, but they weren’t fat then. Being fat might be a good predictor of being in that class, but this model doesn’t explain why. Guyenet’s theory that modern food is too easy and tasty and screwing up our body’s normal self-regulating mechanisms does.
I’m not sure I’m completely convinced by the connection between metagame character creation and body shape, but the idea that humans create multiple hierarchies to obfuscate status and facilitate social cohesion has been discussed on ribbonfarm, eg here.
The intersection between your system and willpower is complex: some people predisposed to avoirdupois consciously decide to become bards and learn to negotiate with shopkeepers, but more passive individuals saturate the niche and are relegated to NPC status.
Ribbonfarm is precisely where I got the idea, and I’m re-reading the Gervais principle now (actually before I saw your post!). But I can’t find many of Ribbonfarm’s more exciting ideas explored elsewhere. For example, the section on arrested development.
Walking around the supermarket, it is extremely easy to think of everyone else as NPCs.
A friend of mine told me that it takes the brain a little while to notice that it has eaten enough. In other words, half a hamburger might be enough to fill you up, but you might not feel full until about 15 or 20 minutes after you eat it, and since you aren’t feeling full directly after eating that first hamburger half, you eat the rest of it.
I have noticed that portion control is easier for me when I eat slowly and deliberately, taking small bites and having stimulating conversation.
It does make me wonder if different eating habits could partially account for obesity; maybe in the past we were more pre-disposed to having a few slow, deliberate meals rather than cramming lunch down so we could get back to work or silently eating pizza in front of the TV?
n++: that’s the same thing my mom (a professional dietitian) would tell me when I was growing up.
Isn’t food reward at least to some degree socially constructed. I typically dislike arguments of this form but in this case I think it’s warranted.There are studies about how the fancy wine bottle makes the 2-buck-chuck taste great. Beyond that some foods get coded to produce disgust in some cultures but not in others. Could we change the culture to make our bland foods taste better? In japan sweet foods and drinks are associated with childhood, and considered embarrassing for adults.
Is capitalism good at making us eat food we are vulnerable to? or is it good at making us think we like that food?
Could our brains response change based on our beliefs, can a bad food be rendered good via placebo effect?
This is supremely fascinating to me. I am one of those people that can eat and eat without gaining much weight despite living a mostly sedentary lifestyle. I eat much smaller meals than most people. My mother is the same way, she only eats about 1.5 meals per day. We both have Tourette’s Syndrome which causes us to twitch and fidget a lot throughout the day. So now I’m wondering if an over-fidgety nature and low caloric intake are highly related. My father can gain weight easily and does not have Tourette’s Syndrome.
That is interesting. I’ve always been very thin, don’t think I eat significantly more or less than average, and have exercised in amounts ranging from almost none to moderate with no discernible impact. I also fidget a lot, but I can’t believe it comes to anywhere near 700 calories a day; that’s the equivalent of running 4 miles for a 180 pound person according to this.
Well, take as a random number 500 calories per day. If you’re awake 16 hours a day, then that means you would only need to burn an extra 30 calories an hour from moving around to make up the difference. That’s less than the difference between standing and sitting down as a point of comparison (which is also a very effective weight loss technique).
I dislike the discrete argument that ‘diet and exercise’ either work or they do not work.
It would be useful to set up boundary conditions, then admit that there is some nonlinear function mapping them.
If you give me any obese person, I don’t care who, and I put them on a 700 calorie per day diet of vegetables and chicken, and force them to walk or swim (or whatever) for a year, they will lose weight. That is where the strictness of physics takes over.
If I *asked* them to do this, and made them promise, they probably wouldn’t. The overwhelming urge to cheat on the diet would overwhelm them. Is this ‘diet and exercise’ failing? Or is it some other factor that prevents individuals from committing to diet and exercise? In which case, we should be explicit about it. Whether it is ‘their fault’ or not is am ambiguous value statement. However, we can note that it is remarkably hard for humans (particularly with brains compromised from junk-food hacking) to override the temptation to defect on a spartan diet and exercise.
This is exactly what the military does in boot camp. If someone is overweight, they get reduced rations. If someone is underweight, they get extra rations. And then they move around a lot all day long. It works pretty damn well, and those people aren’t even obese.
“Diet and exercise” is the communism of weight loss:
“It doesn’t work!”
“It doesn’t work because people don’t do it properly!”
“Well, if people can’t do it properly it doesn’t work!”
“The method’s fine, if only people would behave better!”
It works for some people. Communism just plain doesn’t work.
Imagine if it were that communism somehow magically worked for like twenty percent of countries that tried it. Then its status as something that can work in certain circumstances would be much, much stronger than the status quo, in which it never works.
Cuba’s still plugging along.
So does Venezuela and Best Korea. Your point?
Something similar to communism seems to work fine for eusocial species. The reason it doesn’t work for humans is that we have our own children rather than all of us supporting our sister, who reproduces for the whole group, so it is not in an individual human’s best interest (in an evolutionary sense) to give up the products of their labor to support the children birthed by strangers.
If the children other people produced were just as related to us as our own children (and especially if this was coupled with some of us being in a non-reproductive caste and thus only being capable of reproducing through supporting our reproductive biological sisters/brothers), communism would probably work fine.
Of course, no human population has a eusocial reproductive system. But I wanted to point out that it’s not impossible to get communism to work with living beings. It’s just impossible to get it to work for species that would have to go against their own evolutionary interests to live in a communist system.
Overall, sure, you have a point. Reminds me of that entomologist who said, about communism, something to the effect of, “wonderful idea, wrong species”.
Unless the strangers are, in fact, rather closely related all considered. Welfare seems popular and workable in monoethnic states, whereas support is low and abuse high in multiethnic states.
… And the highest performing countries demonstrably used communism to reach levels of achievement and prosperity that the other countries had previously thought to be impossible, while continually competing to commune harder and reliably breaking records year after year through the use of novel new communing techniques.
Seeing as how approximately everyone who says “diet and exercise” then expounds at great length about diet and either doesn’t mention exercise again or offers a brief, standard rationalization about why it’s not really part of the program, I think the “it hasn’t been tried” faction has a somewhat stronger case here.
My take on it is that exercise is important, but you have to discard all the popular health advice about how just a little bit of exercise is helpful. If you want exercise to noticeably impact your weight, you have to do a good deal of it at high intensity. And of course not eat it all back.
I’ll throw in another data point.
I eat what and as much as I please, subject to mild money constraints (I haven’t had sushi lately) and some mild restriction of complex carbs.
I’m 4′ 11″. I weigh 165 pounds. In other words, obese, but I’ll never be used to illustrate “the obesity problem”. What proportion of people are as fat as the people in those photographs? Under a percent, I bet.
I’m down from 185 pounds. Ten pounds got lost surprisingly quickly and easily after I ecame aware of tension around my ribs near my breastbone and released it. I thought this would just lower anxiety, but I also became more aware of satiety.
I’m not sure how I lost the other 10 pounds.
I’m also not sure why I’m not fatter. It’s possible that, since I don’t like saltiness, I’m just not the sort of person the junk food manufacterers are gunning for, but I’m not that crazy about sweet junk food. Even the Tasy Cake Chocolate Junior, my favorite thing along those lines, only gets me to eat something less than one per week.
It’s also possible that I’m more sensitive to feeling overstuffed than a lot of people. I’m not seeing a lot of research about when and why fat people don’t eat as much as possible.
Interesting. In the last couple years, I’ve begun to carry tension in various places. It started with my face which, after a few weeks, resulted in my eyelids twitching uncontrollably. It took me another few weeks to understand the problem and release it, but then the tension moved to my abdomen, and it’s been harder to squelch there. I’m buying this book you linked, thanks. 🙂
So, this lines up with something I’ve been pondering a lot lately and doesn’t sit right with me. I have a friend who is a biological determinist and doesn’t believe in free will at all. When we have ethics debates, my position is usually that free will is a useful concept to define and use in moral theorizing, even if it isn’t real. But I’ve been bothered by this, especially because the more I research and read about neurological feedback, it really does seem like “regulated by neurochemical control loops in the hypothalamus” and “controlled by conscious thought” aren’t as different as everyone would like them to be. This last surfaced for me when I read a Facebook post by a different friend advocating for support for people with mental illness, using the slogan ‘chemical not character’ – i.e. someone with a mental illness doesn’t have some kind of character flaw or moral failure, but rather a physiological (i.e. chemical) medical condition. I thought this was a good slogan, but I realized that this could apply to all of our consciousness. There really is no difference between character and chemical, and reading about the hunger feedback loops deeply disturbs me, because it makes this equivocation really obvious.
I don’t know how to resolve any of this. If anyone has further reading on this topic, please send it my way.
‘chemical not character’ [ … ] I thought this was a good slogan, but I realized that this could apply to all of our consciousness.
You are in danger to start liking the books by Peter Watts, esp. “Blindsight”.
This question has been on my mind for all of my adult life, and I haven’t been able to “resolve” it in any way that makes the difficulty go away. I don’t think it’s possible. The real answer, as far as a I can see, is what you’ve already said: there is no clear difference between “chemical” and “character”, they’re just different models we apply to the world, sometimes one model is more justified, sometimes the other (“get used to it” is my best tip).
Free will as a concept works well when applied to a human as a whole, viewed from outside, but dissolves into incoherence where you start to look inside the causal mechanisms of decision making. It reminds me of the quote “If this happens by itself in the brain, where am I? Am I out of the loop? – No, you’re not out of the loop, you are the loop.”
Elbow Room and The Problem of the Soul are good books.
I have pretty much the same beliefs as your friend (that free will doesn’t exist and human behavior is entirely biologically determined, with small exceptions for when people, say, get hit brutally in the head and become brain damaged, in which case a tiny amount of environmental determinism is the cause of the person’s outcomes post-brain-damaging).
I wish I had some good reading to recommend you, but I don’t. I just wanted to post this so you’d know that there’s at least one other person out there who believes this and still goes on living their life as normal. Though I don’t believe in any kind of free will, it’s still useful to pretend it exists when you’re making small choices in your life, such as deciding where to go to dinner. I’ll usually think of it as “I decided to go to restaurant X” instead of “The neurochemicals in my brain lead me to desire food from restaurant X more than from other restaurants on this particular day based upon some calculation involving satiety, the recency of having been there, and the general taste of the food,” even though the second one is what I believe is actually happening.
The !Kung Bushmen, everyone’s go-to example of an all-natural hunter-gatherer tribe, apparently get 50% of their calories from a single food, the mongongo nut, and another 40% from meat.
Does this seem odd to anyone else, or is it just my assumption that “hunter-gatherer” meant a wide range of non-meat foods (berries, fruits, pulses, whatever can be harvested in the wild)?
50% of your food intake from one source doesn’t seem very diverse, given that the remaining range of non-meat food sources only come to 10%. So how are the hunter-gatherers all that different to farmers growing one staple crop, if they are relying on one particular food? How does that jibe with all the things I’ve seen about the hunter-gatherer lifestyle being superior and early farmers having worse nutrition and health as seen by their skeletons, etc?
(It also seems to me that if anything happens to the nut, like bad droughts or blight, the !Kung are in trouble, unless they cope with that by upping the amounts of other vegetable food sources they consume).
Purely a guess, but it might be because nuts tend to be more easily stored. Even if you’re hunter-gathering rather than farming, you still need to have surplus storage to even out the down times. Also, my limited understanding is that hunter-gatherers don’t actually spend that much time on food acquisition. A few hours a day. If they were spending 10 hours a day already to scrape by, they’d have no margin for error in bad times. So if a blight hits the nuts, they’d have room to up their hunting or foraging to more hours for survival.
https://en.wikipedia.org/wiki/Mongongo#Nutrition
Mongongo nuts have a fairly complete nutritional profile. Plus 40% of the rest of their diet is coming from meat. I’m guessing a bit here, but I would assume early farmers relied on staple crops that had much worse nutritional profiles, especially grains which were mostly carbs. And they probably didn’t get 40% of their diet from meat. Plus it’s likely that early farmers went through more periods of famine when crops failed or what not.
Next food fad!
Honestly, “damn, now I want to try a mongongo nut” was my first reaction to this article.
They look kind of like walnuts.
Now that you can get goji berries in CVS (a major drug store chain), it’s definitely time for something new.
Looks like you can source them from Cameroon for $200/ton- very affordable!
Unfortunately I can’t find a way to buy less than a ton, so you might be stuck going full !Kung for a few years.
Coordinating the sale of a ton of mongogo nuts is exactly what Kickstarter is for.
I looked into it since we are always on the lookout for more and better ingredients even if unusual. But they are extremely similar to almonds, nutritionally.
Alright that settles it. Going on the almond and steak diet.
I expect the !Kung eat more of the animal than the muscle meat.
This clickbait website predicted mongongo nuts to be the next food craze two years ago. For some reason it didn’t catch on.
They ALSO said that mongongo nuts are like kopi luwak, only with elephants instead of civets. Given that people do buy kopi luwak, I don’t think that would be much of a deterrent.
Th Wikipedia article does say that collecting the nuts from elephant dung is a thing, but more as a labor saving device than some special property it’s supposed to imbue the nut with (unlike kopi luwak). My impression is that just grabbing them off the plant is more common.
And following from my earlier post for what it is worth as a heavy smoker of 20 years with several failed attempts to give up I read Carr’s book on the subject and on putting it down never even considered smoking again. Once you get your head straight, addiction becomes much easier to handle. This guy really does understand addiction from the point of view of the addict rather than from the point of view of the scientist. Ah well, I am sounding like a advert so I am sure I am convincing nobody.
What exactly does it mean to “get your head straight”?
I read Allen Carr’s ‘Easyway to Lose Weight’ and I think his approach cuts through it all. He makes the point our bodies know exactly what to eat. How can scientists do better? If you eat what you were designed to eat (caveman diet thinking) you will enjoy it better than processed stuff because evolution evolved you to like the food that is best for you. Any other conclusion is bizarre. But modern food confuses us so we need to get our heads straight. Once we get our heads straight and stick to the right kind of foods we can totally enjoy our food and stay the right weight. The science of food may be very interesting but it just confuses people. So get your head straight, understand what you really enjoy and it genuinely becomes easy.
I don’t know. Maybe I can use his system to stay at the right weight once I get there, but for me it doesn’t work to lose weight (I tried for several months). Carr’s books about smoking and alcohol are awesome though, thanks to those I’m 20+ years smoke-free and 8 months alcohol-free now. I wish I’d discovered the second book earlier!
The establishment doesn’t believe that obesity is just about weak-willed people voluntarily choosing to eat too much, or that obese people would get thin if they just tried diet and exercise, or that all calories are the same.
Pardon me while I grope around on the floor; my eyes rolled so hard at this they fell out of my sockets and rolled under the table.
Oh really? This isn’t the establishment view? I’ve got a consultant cardiologist at our university (hah! so-called! but this is a digression) hospital who has a different opinion, and this is a direct quote when I was getting into it with him about the diet and exercise thing and that yes, honestly, I was doing that but I had problems sticking to a diet:
“Did you ever see a fat hunger striker?”
Now I may possibly be putting words into his mouth but what I took away from that was: if people can starve themselves to death, then plainly willpower is not the problem when it comes to cutting back on food (you fat lazy tub of lard who prefers to lie around stuffing your face with junk food rather than diet and exercise). (And the worst thing about that whole encounter, where I admit I threw a tantrum and stalked off in a huff, was that I only turned up because I got a letter calling me to the outpatient clinic. I don’t have heart problems, despite the dire warnings about obesity and heart attack! stroke! so I have no idea why I was there in the first place, apart from being insulted to my face).
Every single medical person I’ve interacted with has done the diet and exercise spiel. I think Scott even mentioned in past posts about doing it himself: the obligatory “you know you’re overweight? you know you should lose weight for the sake of your health? have you tried diet and exercise?” lecture.
As to the rest of it, diets are only half the problem. When you lose weight, that’s the first half. Keeping it off is the second, and to do that, there’s no going back to ‘eating like a normal person’. You will, for the rest of your life, have to do the calorie counting, portion measuring, juggling with ‘if I have a glass of wine at the birthday party how many calories are in that and how do I make up for them? What do I cut from my meal plans for the succeeding three days to offset the splurge of calories?’ and making lists of what foods you can and can’t eat, on top of the exercise plan.
Someone who only has a few pounds to lose can go “Whoa, I’m starting to pack on the chub, better cut back on the grub!” and afterwards resume ‘normal’ eating. People with a lot of weight to lose can’t do that.
The ice-cream example would be vastly different if Scott had been accompanied by someone (or had the voice in his head) saying “Are you sure you really need that ice-cream? Because you just had lunch, you know, and this isn’t in your diet allowance”.
That’s actually the worst thing about being visibly fat (not the few pounds over but really fat): that if you’re not eating at a social occasion, people leap to the conclusion that you’re dieting (because why else wouldn’t you be stuffing your fat face, it can’t be simply that you’re not hungry) and even worse ‘congratulate’ you in a smarmy manner.
“Oh, you’re so good! Sticking to the diet! I wouldn’t be able to resist temptation!”
What that really means is “I’m not a porker so I don’t have to watch my weight so I can afford to indulge in a bit of excess or a treat now and again. Not like you, fatty, who plainly is not eating because you’re on a diet because you need to be on a diet”.
I’ve changed my use of “establishment” to “scientific consensus”
Thanks! I don’t intend to be mean to doctors, it’s just that one particular encounter really got my blood boiling (and, as I’ve said, I’m blue in the face listening to the “have you tried diet and exercise?” advice, which is part of why I got snarky with the cardiologist in the first place: wow, I have never heard this before, I never considered dieting and exercising in order to lose weight, what revolutionary life-changing advice!)
I find it surprising that scientists had a hard time making rats obese, since in my experience as a pet owner it’s very easy to make cats and dogs obese. Is modern pet food also hyperpalatable, or do rats just have better regulatory mechanisms than cats and dogs?
That struck me too. But I think you’ll find that most overweight pets don’t get obese from dog / cat food; it’s usually some combination of table scraps and pet treats. I suspect pet treats might be the pet equivalent of hyperpalatable food (even if the kibble is not).
Pet observations also definitely suggest that very rigid simplistic CICO is not quite right. I know a family with two german shepherds, a male and a female. They are both fed literally the same amount each meal. They both get the exact same exercise (walked at the same time, etc.) The male has a full-body tire and weighs 140 lbs. The female weighs 70 lbs. Now, the female also defecates literally 8-10 times per day, and the male no more than twice, so it’s obvious that something in the gut is not processing calories the same way. (I know that the thermodynamics-level CICO is correct, but it is clear evidence that what actually counts as a “calorie in” and a “calorie out” are not the same from pet to pet).
> (I know that the thermodynamics-level CICO is correct, but it is clear evidence that what actually counts as a “calorie in” and a “calorie out” are not the same from pet to pet).
I appreciate this clarification. I think, if nothing else, this thread has made it clear that CICO means a lot of different things to a lot of different people, and so should probably be dissolved as a phrase into its possible meanings, for clarity
It strikes me as the type of thing where the relative ease or difficulty of measurement has shaped the whole concept. You can pretty carefully measure the chemical energy available by oxidation of food with a calorimeter. So we measure the food prior to ingestion and call it “calories in.” We call it that even though what we’re really after is the chemical energy actually absorbed and released into the body after ingestion and digestion, because that’s really difficult to measure individually. Similarly, you can measure the minimum output of a body (turning a cycle wheel, moving 100 kg up X stairs) pretty easily. So we measure that and call it “calories out,” even though we’re really after the amount of chemical energy released by a certain set of chemical reactions inside the body, including resting metabolic reactions, because that is very hard to measure.
And most of the time for most people that’s pretty good. It works fine for me; I must be close enough to average that the measurable is a decent proxy for the desired measurement. So I find CICO utterly banal on one level – no one can gain 2 kg from eating 1 kg of food, mass and energy are conserved. The hard question is just how big the error bars can be between the proxy measurables and each individual’s set of actual measurements. Seems from the article, and anecdotal experience of others, that those deviations can be pretty large.
That’s what annoys me about “you’re claiming you can violate thermodynamics!” if you say calorie counting was not particularly effective.
Sure, thermodynamics are involved at the base level, but we’re talking biology here; there’s a lot that goes on between shoving food down your gullet and the actual conversion of chemical energy. The idea that the actual thermodynamics involved match easily to the numbers on the cookie box and the FitBit is a distorting oversimplification. In reality that relationship definitely varies from individual to individual, and also doesn’t seem to be constant over time even in the same individual.
FWIW anecdotally I was able to lose weight by calorie counting, but had to be well below the recommended caloric intake level to stay on-plan (e.g. a meal tracker, based on current weight, sex, and BMI, recommended I eat something like 1800 calories a day to lose 1.5 lbs a week. I could only achieve that weight loss rate by averaging 1500 calories a day). At first I thought I was cheating somewhere, but even being very strict gave the same result.
I agree although think you’ve still only captured part of what people can interpret CICO to mean. I’ve seen many responses that construe discussion of CICO as unproductive or wrong because it puts the focus on determining the correct energy intake, and they believe that most of the difficulty in losing weight for people has little to do with the difficulty in determining how much to eat, and lots to do with the difficulty in actually eating that amount.
And to be sure, there is a lot of difficulty in that.
Wait really? Either I do not have a good understanding of when a cat is obese or my experience directly contradicts yours. My Family has owned +20 cats over the years and there were only two that I would classify as fat.
The first one clearly had an eating disorder where she ate whenever she could and begged for food at all times, the other was jealous when she wasn’t alone in the house anymore and attempted to “steal” the food of the newcomer (she became normal again when the newcomer died). All the others pretty much selfregulated completely, which often resulted in 1/4 of cat food to be frown out. I must admit though that we usually were kinda stingy with treats.
We have a very weird cat who refuses to eat anything other than dry cat food. Even treats that are very similar are suspect. She’ll occasionally lap at milk, but otherwise turns down any offered scraps. Needless to say, not obese.
Our dog probably would get fat if we allowed him to. He will wolf down whatever is in his bowl, and will eat just about any “human food” if offered. On the other hand our family’s previous dog (same breed) was always very thin, and we’d just leave out a full bowl of food. He’d eat when he was hungry. Got to lick plates and for some reason loved a bowl of frosted mini wheats (no milk) every morning. Pets can be weird too.
An indoor surgically neutered cat or dog (esp a dog) is more activity constrained than a rodent in a cage under the conditions they did the experiments under.
My experience (n=1) is that my dog will self regulate fine with dog food, but will always eat more of almost all kinds of regular food.
Much like with dieting oneself, the trouble is not having him overeat his bland food, but rather preventing him from getting the good stuff.
Anecdote: I have had many pet rats, and about half of them easily became obese eating a standard pet rat diet, while the other half did not. I don’t know if this means anything, but my albino rats were much more prone to obesity than my rats with other fur and eye colors. The majority of them got fat, while the majority of the other kinds of rats did not. All of these rats were female and lived together, eating the exact same food.
I am surprised that they haven’t figured out some kind of hyperpotent leptin-analog drug that targets and binds to the leptin receptor. Vaguely similar things exist for all kinds of hormones and neurotransmitters.
Even if leptin injections are an inefficient mode of weight control, it still seems to suggest a promising pathway, especially in people who have lost the weight and want to keep it off.
A few typos of “letpin” rather than “leptin”.
Does anyone know of research that attempts to distinguish between a ‘body weight set point’ and a ‘body fat set point’? For those of us who enjoy lifting weights, those two concepts would have very different implications.
Since it’s called lipostat, it is supposed to be a fat set point. The obvious guess is that we have a separate muscle set point, how much muscle the body thinks it needs, based exercise.
But why does exercise reduce fat? If you had a constant caloric intake, exercise consumes those calories, both directly and by creating hungry muscles. But the whole point is that you don’t, that it’s controlled by hunger. I don’t know the literature, or even what this book says, but Scott alludes to this topic once: “Did you know that exercise might help stabilize the lipostat?”
Note: This is a drive-by comment, I will not have time to come back for the debate
The book is great and this is a good review of it. Few notes:
1: I found nothing in the book that contradicts CICO, it’s just a very good explanation of why people tend to eat more than they run. (which is good as any theory that contradicts thermodynamics is suspect.)
2: If you assume that the lipostat works on lipids and that the easiest way to kick it out of bounds is to supplement and/or substitute sugars for fat it is also compatible with a low-carb diet.
3: All of this is pretty much standard operating procedure in exercise nutrition and I find it annoying to notice that the people who fail at making dieters thinner never ever bothers to consult the people that succeed at fuelling Chris Froome to ride a bicycle really fast. The principles are the same, you just want to do the opposite.
4: Speaking of which; the only gripe I have with the book is the use of the word “bland”. The absolutely most efficient way of maximising calorie uptake is through maltodextrin which is utterly tasteless. Conversely, I’m willing to put good money on that if I whip you up a chocolate soufflé with molten honey-and-hazelnut filling and salted caramel topping*, you will not come at me with the word “bland”, but neither will you be able to eat excessive amounts. A more correct expression would be “not junkfood”
*: I will freely admit to having a totally unreasonable food budget; I eat at Michelin starred restaurants regularly enough that there are at least three where the staff knows me by name and I cook to a quite fair standard at home too. (‘Modernist cuisine’ is the best book ever.)
> If you assume that the lipostat works on lipids and that the easiest way to kick it out of bounds is to supplement and/or substitute sugars for fat it is also compatible with a low-carb diet.
The lipostat is named such because of its proposed effects on body fat, not because it is proposed to be set by consumed fats. In making your assumption, you’ve assumed the effectiveness of a low-card diet, so concluding compatibility with that diet is begging the question.
I like Guyenet, but I disagree that his characterization of CICO should be the right one. Spinning it as something to do with willpower is just argumentative and seems more like a smug way to dismiss that lean people may have conscious strategies to stay lean. We have an executive function and it can override automatic regulation.
In fact, when he talks elsewhere in his book about how every diet works as long as it removes something, he’s implicitly acknowledging that CICO works. When he offers services as a diet consultant, he’s acknowledging that executive function strategies can overcome instincts.
The problem is when you say stuff like CICO isn’t true, normal people aren’t relating to CICO with this hyper-nuanced, protect-peoples’-feelings definition that Guyenet is using. They just think it means that somehow calories are mostly divorced from fatness, and that’s pretty darn confusing so they just follow some fad or give up!
This issue came up on the NY Times health blog one time, and that gets a lot of comments, and a couple medical researchers and doctors chimed in saying that diet interventions don’t work, and that’s why they don’t push diet recommendations very hard these days. There are even studies to back this claim up. What’s so odd, though, is I don’t know many people with diabetes, but I used to know 3 people with diabetes: My dad, my cousin’s husband, and my coworker. They all reversed their diabetes by changing their diet–mainly reducing calories–and heavily resisted the drugs pushed on them. Regardless of what the studies say, I think people do change their diets when they have the information and incentives.
I agree. This really needs to be added to the post somewhere because way too many sources bury this very simple and well-researched point that for the average person the difference between diets is negligible. This is why a fairly standard recommendation is that the best diet is the diet that you’ll stick to. There is some evidence that low-carb diets are slightly superior, particularly in terms of body fat percentage, but if someone is severely obese, they’re mostly going to lose body fat when they lose weight anyway.
A couple selected papers:
Johnston, B. C., Kanters, S., Bandayrel, K., Wu, P., Naji, F., Siemieniuk, R. A., … & Jansen, J. P. (2014). Comparison of weight loss among named diet programs in overweight and obese adults: a meta-analysis. Jama, 312(9), 923-933.
http://jamanetwork.com/journals/jama/fullarticle/1900510
Pagoto, S. L., & Appelhans, B. M. (2013). A call for an end to the diet debates. Jama, 310(7), 687-688.
http://jamanetwork.com/journals/jama/article-abstract/1730520
I knew we’d get an officially approved euphemism, but that was quicker than I expected.
I’ll stick with Muggle Realism. 😉
Is home-cooked food every likely to damage you’re hypothalamus? Spaghetti carbonara seems like a superstimulus to me, but it’s not as ruthlessly optimized as Doritos.
I’m buying a blender and a mix of various staples.
That might ruin your blender.
Not according to the Internet! And the Internet never lies, as we all know.
Just be careful not to open a portal to an alternate universe.
1.Is the gladwell comparison illustrative enough to open with like that? The article seems like it could be relevant to a lot of people, and ‘gladwell is a joke obviously’ maybe could alienate some people who could otherwise benefit. Or really most any form of “[name] is a joke” at all, if readers don’t know who “[name]” is.
2. How strongly does BMI correlate with being overweight? It’s a comparison of mass to height, so could it be that over/underweightness cancels out on average, centering things around people’s genetic stocky/thin build?
3. ?Eating less could be worth trying if you are fidgetier than you’d like. (or exercising, but that’s already a standard recommendation for that)
A handful of things I have heard in my life that may or may not be true.
1. People who run in the evening lose more weight than those that run in the evening as those that run in the morning adjust and eat more throughout the day.
2. People with sleep problems often gain weight.
3. People with weight problems often develop sleep problems.
I wonder if there is a sleep mechanism for resetting the our responses to food. This would make sense to me as if I don’t eat for 6+ hours during the day I am starving, but if I eat dinner at 7pm and breakfast at 8am I am usually somewhat hungry, but am not ravenous.
Lack of sleep inhibits production of anabolic hormone(s?) and human growth hormone so that fat production is prioritised at the cost of muscle production and makes weight loss very difficult. This is such a basic fact of exercise physiology that I am perpetually annoyed that nobody seems to take it into account….
I think Scott Sonnon does.
3) could simply be due to purely mechanical factors like the excess fat increasing the strain of respiration (leaving aside the issue of obesity contributing to sleep apnea), increased pressure on teder points and joints rendering beds that are comfy for an average person uncomfortable for an overweight one, etc etc.
Why is it then that I’m consistently able to lose weight only by nutrition and exercise every time I decide to do so?
My weight has been up and down all my life and it always went up when I decided to eat whatever I wanted and abandon exercise, and it ALWAYS came back down in a very predictable and regular manner, when I started watching my calories and start exercise. I have the spreadsheets to prove it (I’m quite an organized person) with beautiful correlation between calorie deficit and weight loss.
In my personal experience of 15+ years weight loss and gain are 100% controlled by rigorous control of diet and exercise.
I have advised friends on my method before and I always noticed, that when they failed to get the results I’m getting was because they vastly underestimated their calorie intake and ended up eating way more than the plan.
Did you miss the whole part about how “everyone is probably different”?could be you just have a particularly weak set point. Also, “its more complicated than CICO” doesn’t mean that strict calorie restriction won’t cause weight loss – it will, no one is physically incapable of starving.
“Everyone is probably different” seems obviously true for hunger, but it’s not obviously the dominant factor in why people fail to lose weight when”trying”. OP’s claim that he noticed people not tracking their calories accurately or cheating should be accepted without convincing evidence that he’s wrong.
Although hunger is highly variable and I have no doubt it makes losing weight for some people much easier, I highly doubt most people are defeated by their body refusing to lose weight rather than the fact that being hungry really sucks. I used to cut weight for wrestling in high school. Almost everyone in wrestling did. Some kids came into wrestling really fat. They inevitably lost a lot of weight even if they didn’t reach the ultra thin point. It’s doable, it just sucks really, really hard. That level of exercise and diet is probably one of the hardest things I’ve done in my life. If you really, really need to be in shape fast we can make it happen, it’ll just take a couple hours a day of exercise and your diet being taken completely out of your control.
A more plausible hypothesis than highly variable setpoints in metabolic efficiency is that almost no one rigorously tracks their calories in and out every single day without cheating. If actual metabolic efficiency was the main explanation rather than hunger being not well tuned for our modern diet, obesity wouldn’t have increased across the world in concert with a massive explosion in tasty snack foods and a decrease in the number of manual labor type jobs. Even most good research on people has to be taken with huge grains of salt because people can and will too easily cheat unless you have a camera watching them 24/7.
So the question is, why can high school wrestlers do what the rest of us cannot?
@suntzuanime
This doesn’t seem so mysterious to me: as a personal example, the amount of leisure time and mental energy I had to change things about my life was infinitely higher in high school and college vs in the workforce. Hell, I’ve had a direct comparison recently: I took a sabbatical, a few months of which were just spent doing nothing structured, and I barely even had to think about eating a perfect diet. Now that I’m back at work, I have a million little factors eating away at my ideal diet: Eating enough vegetables/fruit is tougher when you have less time to do groceries and cook every meal from scratch, time commitments I don’t control mean sometime I have a blood sugar crash and just really feel like a burger and fries, long days at work mean I have less mental energy to resist said burger and fries, etc.
I think this is important: though, technically, it’s cheaper and less time-consuming to be thin (after all, buying food and eating it is more expensive and time-consuming than not buying food and not eating), practically speaking, it takes more money, time, and/or willpower in our society today to eat healthfully.
In such a context, one paradoxically expects the idle rich to be the thinnest and the busy poor to be the fattest, as I think is roughly the case in America today.
I was really only objecting to the OP’s tone, which came off as a smug rejection of the evidence summarized in Scott’s post with a simple “how can all that be true when this worked for me?”, particularly the “every time I decide to” part.
Balazs’ “beautiful correlation” may not work as well for others – if the setpoint hypothesis is correct, similar calorie deficits will not result in identical weight loss for all people, and for the same person, a calorie deficit that works for the first 10 lbs might not work for the next 10 if the body really does self-regulate by e.g. fidgeting more or less (or willpower-wise, maintaining the same calorie deficit after the first 10 lbs might be much harder).
The limitation of the “spreadsheet” approach is that it typically only tracks “food intake” and “extra exercise”. The majority of “calories out” are not covered by that, and thus need to be guessed at and tuned for each individual, and may need to be recalibrated over time.
Conventional wisdom in the lifting community is that you need to do a bit of trial and error to figure out your baseline calorie consumption, because bodies are different and some of the parameters are hard to determine directly, but that it’s pretty stable over time and, once identified, can be tweaked as needed for a bulk or cut cycle.
Calories-in calories-out is correct insofar as, if you stop eating, you won’t produce energy out of nowhere. Where people disagree on is how much willpower it takes to get there. Clearly there are individuals who through luck or more perseverance have managed to permanently lose weight through dieting – some of them write books about it.
But there’s also a population of people who keep failing at it. If you do something drastic like put them in the army they do lose the weight, but they can’t do it if they’re the ones in charge. Hypothetically, declaring fatness as 100% voluntary calories-in-calories-out and then accepting the implications (fat people are of inferior character) will even help some of them bridge the motivation gap. But we don’t want to implement fat-shaming in our culture for a multitude of reasons, and if we find a cure that removes the motivation barrier to dieting it would be superior to a societal approach anyway.
Ultimately the research is about reducing nebulous concepts like “willpower” and “desire to eat” into their constituent biological parts or at least finding levers to manipulate them. Leptin is an example of a biological grounding for hunger, hyperpalatable and bland foods are examples for levers. Some people have more willpower than hunger, others the reverse, you’re in the former group. If you accept that we’re all rooted in physics and have no free choice about anything anyway, the only reason to blame the latter group for their predicament is if the pain is worth the gain, and I don’t think it is.
Sure, but “calories-in calories-out” smuggles in a couple other assumptions – that the number of “calories in” that a given food item can be converted to is predictable (or even constant*), and that the number of “calories out” a given activity consumes is predictable (and though not constant, within a narrow enough range that people claiming to have an especially “fast/slow” metabolism, or that it depends on diet, are looked at with extreme skepticism)
And, yes, either one of these (typically ‘calories in’) can be forced constant by smuggling all variability onto the other, but that doesn’t actually make it more useful for predicting real-world consequences of dietary or activity choices.
I agree with CICO in general, but these assumptions are intrinsic enough to the claim that I don’t think it’s appropriate to characterize objections to it as being about ‘producing energy out of nowhere’ (or dumping it to nowhere. If nothing else, the “calories” [i.e. energy-bearing compounds such as fats, carbs, proteins] may be excreted undigested)
*And also identical to the numbers, calculated by obscure means, that appear on food labels. What if, say, the reason “low-carb” diets are successful is because the ‘calories in’ associated with carbs is underestimated, or those associated with fats or proteins are overestimated?
I’m not a fan of the CICO narrative (though admittedly that was the only one that I could find success in in terms of my own weight loss), but I don’t think those are assumptions that CICO smuggles in. It’s not necessary that “calories in” or “calories out” are constant or even particularly predictable – just that “calories in” have some maximum value, and “calories out” have some minimum value. That is, it may be possible that a candy bar doesn’t have exactly the 180 Calories it claims to. But what we know about physics and biology tells us that the number of Calories that a person consumes from it can’t exceed some multiple of the mass of that candy bar. Likewise, that 400 Calories your Fitbit told you you burned during your workout might not be accurate, but what we know about physics tells us that your physical motions required you to expend some minimum amount of energy, as determined by how much force you exerted on your body parts, over how much distance.
And yes, these do posit a certain level of predictableness to the “calories in” and “calories out,” but only the amount of predictableness justified by assuming that the conservation of energy is a principle that we can rely on. And weight loss comes from decreasing that maximum “calories in” and increasing the minimum “calories out.”
At least, that’s how I thought about it when taking on the CICO mindset.
To put your point a little differently, there are two different questions that CICO might answer. One is “how can we predict how rapidly someone will gain or lose weight.” Random 832’s points imply that there is no rigorous way of doing it from calories in or calories out, although it might turn out that there was a simple relationship.
The other question is “how can someone lose weight?” Straightforward physical arguments tell us that if someone reduces calories in by enough while maintaining his activities, he will lose weight. So the claim “I cannot lose weight whatever I do” has to be false.
It might still be true that “I do not have enough willpower to lose weight.” It might even be true that “The things I would have to do to lose weight would have other and very bad consequences for me.” But there is a change in behavior that, if it occurred, would result in weight loss.
My main concern is that I’ve seen CICO used to dismiss the possibility that changes in the composition of someone’s diet can have an effect beyond the measurable change of what the “calories” they end up eating under their new diet add up to. “Just keep eating cake, just don’t eat as much of it” doesn’t seem particularly likely to be a better answer than “change what you eat”.
random832:
That’s a fair concern. Certainly, there are more things to consider when it comes to general health than just weight, and it’s very possible to get from obese to regular weight while resulting in net harm to one’s health.
From what I see, though, the opposite is more of a problem; that people don’t value calories enough and overemphasize “eating the right foods,” which seems to often result in people just eating the same amount of calories as before, just made up of different foods, and wondering why they’re not losing weight. And one’s weight really is a pretty good indicator of one’s health for the most part, when it comes to big swings like from 30 BMI down to 25 or something like that.
In my personal experience, I was taught growing up that eating a variety of foods was healthy. This wasn’t the cause by any means, but listening to that advice, I ended up with BMI at around 32 by the time I was 22. Then when I started following the CICO model, I got down to BMI of about 24 in about a year, just by eating less. It’s not like my diet was extremely unhealthy to begin with but I didn’t really change its composition, and 2 of the more common foods I ate, almost on a daily basis during that time, was bacon and Pop Tarts – just very little of them. And I was definitely much healthier at a BMI of 24 than at 32.
So in my personal experience, I do think “Just keep eating cake, just don’t eat as much of it” can be very good advice.
FWIW this has been my experience as well. I currently at 42 am the same weight as I was as a High School Wrestler.
But it does not come naturally to me (my father is overweight as are my siblings). It requires constant vigilance. Twice (right after I went to college and right after I got married) my weight ballooned up to 40lbs heavier than I am now. Both times I lost the weight by counting calories and I have kept the weight off for over 10 years, by simply weighing myself every morning and if my weight gets over a certain point I start cutting back how much I eat. If that does not work I start rigorously counting calories.
This method has always produced the expected results FOR ME. And my mother taught me this method well before the low fat crazy which I always knew was BS.
I do think there is something to the set point theory, but in my experience (again for me) you can reset your set point down by dieting. Once I have been at a goal weight for a while I don’t have to work that hard at dieting. I do structure my life to avoid junk foods though.
Oh well just another anecdote.
40 pounds might just be within your set point range. I don’t think anyone would argue you can’t lose and keep off SOME amount of weight. But say at some point you ballooned up 100 pounds over what you were, I don’t think it would be realistic to lose and keep off all 100 pounds. And as the article points out your lipostat may vary from others’. I for one have a ceiling of about 150 pounds. A few times in my life I have hired a personal trainer for several months and been able to slowly build up muscle weight. If I stop exercising for a few weeks I lose the muscle very quickly. So I could gain and keep weight if I dedicated my life to doing so. I assume the experience for obese people is similar. If they truly dedicate a lot of time and money to losing weight it CAN be done. But you have to stay vigilant for the rest of your life. The body wants to return to that set point eventually and if you slack for even a week the process will begin.
But as others have mentioned how does the set point theory reconcile with the change in obesity rates over time? What has driven set points higher since the 1980’s?
I guess you can argue that increase calorie intake at an early point in life is ratcheting up folks set point and then the body works really hard to defend that point. But that still is an argument that the obesity problem is driven by folks eating too many calories (and to a lesser extent not getting enough activity).
I thought one of the points of this article was that we don’t know exactly what’s driving the rate up but it’s something to do with an increased prevalence of junk food. My best guess would be these “empty calories” aren’t modifying the liopstat like they’re supposed to, so you’re gaining weight that the body doesn’t recognize.
But the rise in obesity has been accompanied by a rise in calories consumed. Maybe junk food not modifying lipostat is the reason people consume more calories in the presence of junk food. But it is hard to see how increased calories is not a major driver.
BTW here is Guyenet himself on the topic.
What caused the obesity epidemic? As I’ve noted in my writing and talks, the obesity epidemic was paralleled by an increase in daily calorie intake that was sufficiently large to fully account for it.
http://wholehealthsource.blogspot.com/2014/04/calorie-intake-and-us-obesity-epidemic.html
I, personally, have no trouble believing that increased calorie consumption fully accounts for the obesity epidemic.
Question is: what’s causing us to consume more calories than in the past, assuming people of 100 years ago didn’t have way better will power than us (though that may not be a given, and they may have also been scratching more of their addiction “itches” with tobacco and alcohol)?
@onyomi
I think companies have just gotten better at creating hyperpalatable foods that interact with our brains like cocaine does and make us want to consume more and more.
I mean, fast food and chain restaurants existed pre-1980s but they weren’t as ubiquitous and there wasn’t as wide a variety.
onyomi: This article is very illuminating:
https://mobile.nytimes.com/2013/02/24/magazine/the-extraordinary-science-of-junk-food.html
@Scarecrowboat
Thanks for the link.
I had heard, of course, about food scientists, taste tests, etc. but it’s kind of frightening when one realizes that, by exhaustively testing every variable to determine which recipes consumers would most enjoy, food companies were, unintentionally (in the sense of, not meaning to make people fat, though intentionally in the sense of wanting people to buy more) creating the most addictive possible food.
Though it also gives me a glimmer of hope and raises a question:
Couldn’t there be an equally impressive “diet Manhattan project” where we exhaustively test all the variables that lead to satiety relative to calories and come up with something like a meal square which almost all consumers agree makes them feel super full and satisfied despite not having a lot of calories?
There would be huge profit in it too: “eat one square for breakfast, don’t do anything else different, lose weight; if you need to lose a lot of weight, eat one for lunch too.” That is, if we can optimize food to trick us into thinking we’ve had fewer calories than we really have, why can’t we optimize food to trick us into thinking we’ve eaten more than we really have?
Such a food might taste mega-bland, perhaps, but I’d rather eat say, a really bland breakfast than attempt to calorie count or otherwise exercise restraint around delicious foods when I feel I’d like to eat more.
*Such foods probably already exist to some degree: I recall reading about an experiment where people were asked to eat a large bowl of oatmeal, I think, every day, and otherwise make no special effort to lose weight. I think people did lose weight, not because oatmeal has no calories, of course, but because it was more filing and satiating, relative to the number of calories it has, than most other things people were eating. Can we invent “super oatmeal”?
Why money? Eating less costs less, not more. What would have to be dedicated is mental effort.
Yeah, I’ve always been puzzled by the “eating healthy/losing weight is expensive” perception. Fresh fruits and vegetables are not prohibitively expensive (though I guess it depends on the type you’re buying.) Neither are things like beans and lentils, or eggs.
I mean, yes, it’s probably a bit more expensive than subsisting entirely on ramen and Oreos, but what I think of as a reasonable and healthy diet seems like it would actually cost less than eating fast food every night.
Maybe when people say stuff like “eating healthy is expensive” they’re thinking of expensive, prepackaged brand-name diet foods.
My own experience: I used to weigh 205 pounds. I started dieting, with pretty careful calorie-counting, and lost weight much faster than I expected down to 180 pounds. After 180 I lost weight much less quickly than I predicted, even though I was using the same math and calorie-counting ability both times.
I definitely don’t think diets are useless, but they seem very finicky about when they do or don’t work.
That’s nothing. I used to be 8 lbs and I haven’t had any luck getting anywhere near that over the past 20 years!
I don’t think CICO is some kind of perfect math that works the same for everyone at every weight.
But if you want to lose weight the big thing to do is eat less and calories are a pretty good measurement of how much you are eating.
For some people less might be 2000 calories for others it might be 1200.
Even if CICO is not a perfect math, I think the main argument is that it’s far too simplistic to be useful for lots of people.
For instance say you are normally eating ~2500 calories a day, but you’re a bit overweight and want to drop 20 lbs. So you cut your intake down to ~1500 calories. At first you lose some weight, but soon through less fidgeting or some other conservation strategy your body adjusts its basal metabolic rate down and you plateau. So you’re eating less and feeling hungry but going no where. Sure, you can cut your calories even further or exercise even more (though the amount of calories burnt in exercise is almost a joke compared to your basal rate), but I think at this point most people get frustrated/angry and give up.
CICO is valid in a theoretical sense, but it’s basically useless and even discouraging for a lot of people when put into practice.
I have seen it work for enough people to conclude that it is far from useless. Everyone I have known who has seriously tracked and limited their calories has lost weight n=~6.
Most people who are overweight are eating more than the amount of calories typically recommended for the average person but think they aren’t.
Actually tracking what you eat for a month can be eye opening and can give you a better idea of what you should be eating to stay at your desired weight.
I do believe that for some folks due to metabolism that they have it harder than others, but I don’t think he proportions of those people have changed drastically since 1980. Yet the portion of people overweight has increased and the reason is that people are simply eating more calories. For most people who want to weigh less the answer is eat less calories. How hard it is to achieve that probably varies from person to person.
From Stephan Guyenet himself http://wholehealthsource.blogspot.com/2012/06/calories-still-matter.html
Yes, but the point is that people are eating more calories for a reason that can’t be placed entirely at the feet of willpower or even conscious decision.
Under conditions where there is no “hyperpalatable” food sources available, pretty much everyone will consume only as many calories as they need without having to meticulously pay attention to their diet.
I don’t doubt plenty of people with enough willpower can watch their calories and consciously balance their consumption. But we really shouldn’t have to, and if we understood what was happening in the underlying biological system we could possibly protect against it better.
For an extreme (and possibly unfair) analogy, there’s people out there who can do heroin casually and with some willpower they can still be functional members of society. That’s not the case for a lot of people. Should we be telling addicts that they need to start counting the grams of heroin they do each week and to willpower themselves to a healthy relationship with the drug?
Obviously not. We tell them to do no drugs at all, and then we do our best to incentivize that. Depending on how bad the problem is, we’ll probably offer them carrots if they stop, we may try scaring the shit out of them if we have to, and we may even lock them up under close supervision if things get real desperate.
What probably won’t get them to quit heroin is telling them it’s not their fault they’re addicted to heroin and there is unfortunately no way to resist it’s sweet siren call but at some point in the future maybe we’ll have a method that hacks their brain.
It’s interesting and useful to research ways to manipulate the brain and body, but until someone has a more usable idea that is proven to work, we just have to buckle down, tell people who want to lose weight they are going to have to do it the hard way, and support them through their ordeal even if there are occasional steps back as long as they are overall improving. Even if someone loses less weight than they wanted and goes from 250 to 225 instead of 250 to 200, that’s still probably an improvement and worth encouragement. No need to let the perfect be the enemy of the good.
I know it also helps to have a culture that encourages exercise and healthy eating etc. but that’s also long run and probably harder than hacking our hunger.
Of course, if people don’t want to lose weight that’s also their prerogative.
I feel the bolded bit is an empty statement. We shouldn’t have to watch people die either, but it’s going to happen for the foreseeable future, so best to learn how to deal with it. Because we don’t know if hacking our hunger without side effects is 5 years out, 50 years out, or 500 years out.
I feel like somebody should point out here that aside from legal risk, the chief negative health effect of being continuously addicted to legal heroin (preferably in pill form) is constipation. If we care about the welfare of heroin addicts, the best practical solution to their problems is to fully legalize the drug and its paraphernalia. Near as I can tell, it’s puritanism (and a lot of misinformation pushed by the usual sort of Baptist/Bootlegger coalition) that prevents this.
I feel like somebody should point out here that aside from legal risk, the chief negative health effect of being continuously addicted to legal heroin (preferably in pill form) is constipation.
Really? It’s entirely possible that I’ve just been brainwashed by the media but I had the impression that heroin is the type of thing that people tend to OD on and die. Or is that more a risk with the injection method?
I mean, I also don’t doubt there are many people who take it for years and remain functional or even successful. But whenever I hear about someone dying from an accidental drug overdose it seems like it’s always heroin or prescription painkillers.
A lot of opiate ODs in my area are from inconsistent street doses. You would avoid that with consistent legal doses.
There’s also deliberate suicide; I don’t know how those are separated from accidetal OD.
A lot of prescription painkiller ODs are actually from the poison that the government puts in the painkillers to kill you if you take too much, rather than from the opiates. So it would be nice if the government stopped doing that.
@suntzuanime:
Yeah. To be fair, the acetaminophen content of a Vicodin pill is medicine. It merely happens to be a medicine that will destroy your liver if you take too much.
@Hyzenthlay:
Because paraphernalia is outlawed, people share needles and re-use needles which might be dirty or blunt or infected. Because use and sale is illegal people use those needles to shoot up in unsafe places. Both of those lead to a risk of HIV, infections, vein damage etcetera that would go away if you could easily get clean cheap needles and buy a cheap reliable known dose and get help administering it in the equivalent of a pot cafe.
Because the drug is illegal it is very expensive and hard to get in a consistent known potency level, so people can accidentally take too much or go too long without it and go through bad withdrawal. Or they might take other drug combinations to make up for not being able to get enough good enough heroin. They might then die due to a bad drug combination (including say, alcohol and pot) and have the death automatically blamed on heroin because in the popular mind that’s the most dangerous drug they had recently taken.
Part of the reason people shoot up is that the drug is so expensive – it’s more efficient per unit dose. Shooting up causes the level in the bloodstream to change very suddenly. Taking pills is much more safe but some of the active ingredient is destroyed by stomach acid or takes longer to digest. (One of the founders of Johns Hopkins was a heroin addict.)
One reference I like on this stuff is Licit and Illicit Drugs by the editors of Consumer Reports.
Because the drug is illegal it is very expensive and hard to get in a consistent known potency level, so people can accidentally take too much or go too long without it and go through bad withdrawal.
Makes sense. I guess someone could argue that making it illegal cuts down on the number of people who try it in the first place (though whether that’s true, I don’t know), but with most drugs, it seems like laws just worsen whatever problems they’re trying to solve.
Yes, I went through a period where I was noticeably “fat” in high school (don’t remember the actual weight). In retrospect it was obvious why it happened: I was eating the school lunch every day, which consisted of burger, fries, cookie, etc. I started bringing my own, very light lunch and/or skipping lunch, as well as starting a new martial arts class.
I pretty quickly got back down to what is normal for me, i.e. not “skinny,” but not noticeably fat, but continuation of that exact same plan would not result in me going from “average” to “six-pack abs.”
Similarly, right now, if I get much above 160 lbs. I can get back to 160 fairly easily with intermittent fasting, but it’s extremely difficult for me to get, and stay below that level.
Sounds about right. Losing the last few pounds is extra-difficult for most people.
Requesting link to the paper on this one:
“Next, they locked morbidly obese people in the same room. They ended up eating only tiny amounts of the nutrient sludge, one or two hundred calories a day, without feeling any hunger.”
I wonder if there’s a business idea there for “eat as much as you want” nutrient diet paste.
Or “eat as much as you want” fat-camps where you can eat as much of Generic Feed Product as you want but only Generic Feed Product.
Citizen! You will report to Dormitory Cafeteria 87A for your daily serving of Generic Feed Product! Remember! The Computer Is Your Friend!
Update: Dormitory Access Corridor 472J currently under repair due to Commie Mutant sabotage. Please reroute all traffic to and from Dormitory Cafeteria 87A through Violet Sector Alberta.
All clones Clearance Indigo and below please stop briefly at the Discipline Booths available at all Dormitory Cafeteria entrances prior to your meal.
Remember! The Computer Is Your Friend!
On a more serious note, I think it’s important to note just how much the success of that was dependent upon locking them in a room for months.
Helping people attain weight loss and muscle gain goals is relatively easy when you have complete control over them AND every aspect of their environment 24/7 for an extended period of time. That’s how I gained nearly 40 pounds of muscle in 9 weeks at Army Basic, and I’m sure that if I could afford to send myself to a Total Lockdown Fat Camp for 9 months I could drop quite a bit of the extremely excess weight I put on after getting out of the military.
The more pointed question is how to help people trying to control that lipostat and manage those hunger signals when they’re adults with credit cards and cars and ubiquitous access to hypercaloric, hypertasty foodstuffs.
CITIZENS! Traffic is now routing through Dormitory Access Corridor 472K, as it was before sabotage. Note that traffic never routed through Dormitory Access Corridor 472J. There never was a Dormitory Access Corridor 472J. If there was, or if there ever had been, it would not currently be full of nuclear sludge due to a meltdown in Safe Fun Times Reactor A92. As has well been established, the SFTR model is faultless.
I think the key is finding ways to metaphorically lock yourself in a room for months. I’ve made it as low as 160, down from an all-time high of over 230, and that’s counting muscle gain. I’ve gained and lost fat since then. Currently, I’m down about 20-25lbs since the beginning of the year. The common factor between times I’ve successfully dieted for fat loss is that there has to be some external motivator/enforcement mechanism, of one kind or another.
Maybe ten years ago I read an NYT review of the Atkins diet and it said that when Atkins came out, the makers of Dextatrim threw in the towel. They had known about low-carb diets for years, but now that it was public, they figured people would no longer need to buy appetite suppressants.
I’m not interested in trying it, but now I am curious if it would actually work, and I don’t remember seeing any Dextatrim ads on tv or products on the shelves.
Dexatrim still exists. It’s primary ingredients are: caffeine, more caffeine, ginseng, and DHEA (aka androstenolone, a steroid).
It’s gotten a lot less marketing, not because of Atkins, but because 1) the FDA sent them letter about making false drug claims, 2) a string of stories came about people taking it and getting heart palpitations, high blood pressure, etc., and 3) DHEA was added to the anti-doping lists for many sports. So they have scaled back their marketing significantly, and now talk about being an herbal supplement to support natural metabolic health, etc.
This can’t possibly be real, can it?
BBC did something of a replication in a documentary: “Why Are Thin People Not Fat” (summary). Results more-or-less replicated and are in line with everything in Scott’s
summaryreview.I bet I could make any prison inmate gain weight if I (and he) wanted to. I was a “hard-gainer” my whole life, even though I thought I had tried hard at times to eat a lot of food. I would always weigh 150 lbs at 5′ 11″.
Then I discovered the Gallon of Milk a Day diet. For a month I drank a quart of milk after every meal, 3 meals a day — so, not even a gallon. I gained 22 lbs in a month.
I’d be very suspicious of the methods of any study claiming you can’t gain weight by overeating. Researchers have a hard time controlling food intake for a bunch of people. It’s really hard to overeat if you don’t have the appetite for it. It’s like torture. The researchers were able to torture a bunch of people? I doubt it. More likely the inmates were scraping food into the trash or some other methodology flaw.
No one ever says, man, I drank a gallon of milk a day and I didn’t gain any weight! The history of modern athletics is people moving their weight up and down at will with calories. You’ll never (ok, maybe rare outliers) find a case study of someone being coached one-on-one to gain weight who couldn’t do so.
I think it can. When I was in college I was trying to build muscle, so I spent a few months straight eating about 2000 extra calories per day in the form of ice cream protein shakes, and gained maybe ten pounds over the whole period. I lost it all very quickly when I stopped overeating. My personal experiences have taught me that calories in = calories out is complete bullshit.
2000 extra calories per day in; how many extra calories per day out and how did you measure that? If you’re going to dismiss the laws of thermodynamics as “complete bullshit”, you could at least try to address both sides of the equation, and if your were trying to build muscle I’m guessing you weren’t living the couch potato lifestyle.
Not to mention that the body isn’t some kind of matter-antimatter, super-efficient furnace. You may well be taking in a lot of calories, but how many of them are used to any productive purpose is anybody’s guess.
Interesting, you make the same point that I just added, but you seem to be interpreting it in the opposite direction. Yes, the body is not a perfect fuel converter, so CICO is definitely false in that particular sense.
I’ve never heard anyone assert that CICO actually secretly means CIBCE=EFBSF (Calories Into the Bloodstream as Chemical Energy = Calories Either Burned or Stored as Fat), but maybe I’m mistaking the meaning.
So far as I know, the formula is:
Intake = Burn + Storage + Waste.
All four vary considerably among humans.
Calories can be “stored” as muscle instead of fat. Or other tissues, but that’s I think a rare and minor thing.
At the other end of the equation, calories in the mouth either go into the bloodstream or come out the rectum, and any great excess of the latter is usually pretty obvious.
So, calories go in, and for this purpose we’ll count only the ones that cross the gut wall. Conservation of energy is applied. Where, other than being “burned”, being converted into fat at 9 kcal/gm, or converted into muscle at 5 kcal/gm, do you imagine they are going?
Asking where, how, and why they are being burned, may lead to useful insight. Denying that they are, won’t.
any great excess of the latter is usually pretty obvious.
I doubt most people put their poop through a bomb calorimeter or even on a scale. An extra couple ounces of waste, or waste with not-fully processed macronutrients, would add up over time without being particularly noticeable.
One of the things that happens to food calories is that they get turned into heat– I believe it’s some 80% to 85%.
A tiny uptick in your average internal temperature would also be unnoticeable, but would potentially be a big source of additional calorie use.
Did you read the link I provided? I’m trying to be delicate here, but Orlistat is a drug that causes your gut to not process 30-35% of the fat calories taken in as food, and if you’re eating a high-fat diet, I don’t think you’ll need a bomb calorimeter to notice the results.
If one person leaves 15% of their caloric intake in the gut and another 20%, that might be a reason why one of them gains weight and the other doesn’t. It’s also something you might learn about if you carefully examine the terms in CICO but not if you just wave your hands and say “metabolisms differ”.
If we’re talking an extra two thousand calories a day, that’s not a few ounces of extra waste, and it’s not likely passing through the gut unnoticed. But if that does happen with any regularity, we should be able to quantify and understand it.
I really think both sides of the CICO “debate” are being strawmanned/motte-and-baileyed here. This seems obvious enough that I wonder why you’re getting so vehement about it (maybe vehemence burns excess calories?)
I mean, what’s your goal here, to prove moridinamael’s anecdote a lie?
Nobody here actually thinks that the calories you consume or burn through activity have zero impact on your weight, and likewise your “CICO, but I and O are significantly variable from person to person and timepoint to timepoint” is not what most people are arguing against when they say “CICO is bullshit”.
We aren’t even mentioning the possibility of what gut bacteria might or might not do with the calories in the gut. You won’t notice calories consumed by gut bacteria and excreted as gut bacteria plus gut bacteria waste.
I am agnostic as to whether he believes his claim. But the claim that any human body can make 2000 kcal/day vanish into the aether, is both false and poisonous to any hope of understanding or solving the problem at hand. So, yes, I want moridinamael to admit that he has spoken falsely or be broadly understood to have spoken falsely and not in a pedantic nobody-really-cares manner. Do I need to call him a “thermodynamic denialist”?
More generally, I want handwaving of the form, “maybe the bacteria ate it”, to be understood as little better than “vanished into the aether” unless expressed with some respect for quantitative analysis. How large can the proposed effect plausibly be, how could it be measured, how could it be changed?
> We aren’t even mentioning the possibility of what gut bacteria might or might not do with the calories in the gut. You won’t notice calories consumed by gut bacteria and excreted as gut bacteria plus gut bacteria waste.
I don’t think this is correct. Unless you gained pounds of bacteria, this would still net out in your poop, which is already one of the factors under discussion. I’ve seen multiple numbers (30%, 55%[1]), but a large portion of your poop by weight is in fact dead bacteria.
[1] https://www.ncbi.nlm.nih.gov/pubmed/7359576
@Virbie:
Yes, a large amount of your poop is bacteria, that was my point. The bacteria cannot be converted to weight gain, as they will leave your digestive track in relatively short order.
If we arbitrarily prevent calories from being absorbed you get all sorts weird effects in the gut, as the bacteria also don’t simply take up those calories automatically. But if the bacteria regulate themselves (yes, this is a handwave) to consume those calories, they still never make it to the bloodstream, and you won’t notice now many more ounces your poop weighs.
You’ll presumably notice gross changes composition and consistency.
And, numbers. The average person (well, the average astronaut-type person; I have strange references) excretes 650 grams of feces per day, containing about 800 kcal/day in purely thermodynamic terms but of which maybe half is plausibly digestible. So if the baseline human consumes 2500 kcal/day, but we’ve got this one guy who packs away 3500 kcal/day without gaining weight and another who says he’s on a 1500 kcal/day diet but can’t lose a pound, how do we attribute this to “gut bacteria (handwave)?” Guy #1 is pooping three times as much as normal, almost four extra pounds per day, and not noticing? And Guy #2 has to be at Negative Poo to make this work.
But this is basic enough science that either the nutritionists have taken the measurements and done the math, or the whole field is bunk. I’d like to see those numbers, if they exist.
sighhhhhh
Okay. As I understand it, the popular conception of CICO that is most frequently promulgated suggests very strongly that the most import knobs controlling weight loss and weight gain – to the practical exclusion of all other factors – is how many calories you’re eating, and how many calories you’re burning via exercise.
So if I eat an ice cream protein shake the size of my head every single day for 2-3 months, and I don’t exercise at commensurately heroic levels, and I gain only ten or so pounds, then I would say that the popular conception of CICO is indeed bullshit.
Yes, it’s obviously true that some combination of the dozen of other factors mentioned in this thread caused my body to still honor the laws of thermodynamics. (Or, actually, just the law of conservation of energy, which is more fundamental.) I think it likely that all the factors Scott goes into in the OP come into play. Some inner regulatory systems caused my body to do all kinds of different things to keep me from gaining weight. And none of things looked like me intentionally upping my exercise to burn calories.
This is simply not what people are discussing when they refer to CICO as a heuristic.
I’m going to tap out here because it’s obvious that this is largely an argument about how people are implicitly defining terms and it’s not too interesting. My original goal was to provide anecdata that you can indeed eat “a ton” and excercise “not so much” and not gain much weight due to mysterious physiological reasons that are usually not discussed. In fact, I was trying to provide evidence for exactly what John Schilling is saying. I guess I just did a bad job of it.
A quick Googling suggests that 2000 calories per day of excess burn is roughly the amount you might expect from an Olympic athlete working unusually hard. In contrast, I was doing about an hour of weight training, roughly five days a week.
There is probably room for some kind of narrative where I was subconsciously eating less throughout the day to offset the caloric bolus of my evening ice cream shake. But I don’t think that’s true because I was trying to force myself to eat more for all my meals.
Of course, I did actually end up gaining weight, but the amount of weight I gained was so minor (and mostly “lean”) compared to the lifestyle change that I couldn’t help but doubt CICO.
All of this set aside, the human body is not a bomb calorimeter. The body does not take in food and oxygen and perfectly combust it into heat energy and carbon dust. There are an endless array of things that may keep your body from properly absorbing the nutrients you eat. Gut flora issues, intestinal absorption issues, general digestive inefficiency, lack of dietary fiber, metabolic diseases, parasites … Any and all of the above can make it so that 2000 calories of food in your mouth does not equal 2000 calories of energy moving from your digestive tract into your bloodstream. And downstream from that, there are other knobs that control how your body prefers to store the chemical energy that it does retain.
So, in that particular sense, a rigorous interpretation of CICO certainly is bullshit, because it’s only a “thermodynamic” issue if you ignore the important factor of absorptivity.
There’s a motte-and-bailey thing going on here. Yes, eating more calories will directionally cause you to gain weight, unless you have something really unusual wrong with you. No, the body is not going to gain anything like the precise delta of mass implicit in the excess calories you’re eating unless you’re unusually efficient at nutrient absorption.
But that’s part of the point. CI/CO is certainly part of it, I doubt moridinamael is saying it isn’t; but without mentioning feedback mechanisms upregulating subconscious movement and metabolic changes the theory is misleadingly oversimplified.
I’m extremely thankful for my genetic endowment in this area. I’m the type of person that will forget to eat, and then wonder why I seem to have an agitated stomach before trying to remember if I’ve eaten. On a typical day, I’ll go around 12 hours between meals, (lunch is such a waste of time) and that doesn’t feel like a burden.
The other side of that though is that the lean side of my family (where I assume such relevant genes largely came from) also tends to be sensitive to bad food or bad diets. Most of my family would feel a little sick after a fatty meal composed entirely of fried chicken tenders, wings, or other such foods; and ice cream, cake, or candy on an empty stomach would also be unpleasant. My mother has also told me of how my grandmother would like to make cakes and pies, and yet even with five children in the house, they’d often go bad before anyone chose to finish them. This sort of thing makes me wonder if part of the operation of that weight set-point is tied to the same instinctual avoidance of foods that have become associated with nausea, or other elements of the disgust response.
…Or my family may just be composed of dirty mutants. My mother was able to serve my family broccoli and other green vegetables with nary a complaint, and I liked eating brussels sprouts raw and freshly picked from the stalk. I was mystified as to what people didn’t like about cruciferous vegetables until I found out how some people are particularly sensitive to certain bitter flavors in them. Over-sensitivity to bitter flavors is really maladaptive in the modern environment–And I blame that tendency for the unfortunate reluctance of people to appreciate the rich complexity of a glass of gin-and-bitters.
My appetite setpoint is so low that I will reliably get bad headaches from low blood sugar long before my body lets me know that I should eat. I have to force myself to eat by the clock to avoid this. I do not ever feel “hungry” unless I don’t eat for like 20 hours. So it’s not all rosy on this side of the leptin-privilege-fence!
MealSquares are not available in the EU, but Joylent is a reasonably priced alternative to Soylent that ships from the Netherlands.
[edit] They have a second benefit: they are very boring food, and also trivial to prepare. (“Take shaker, fill half with powder, fill up with water, shake.” Or for the bars, “unpack bar, eat.”) As such, they’re great at leveraging laziness against appetite.
Counterpoint to this:
I tried Joylent and found that it was not merely bland, but actively unpleasant. I had to mix it with milk just to be able to choke it down. Ymmv, but I’d much prefer something in a solid form.
For the record, I find nothing unpleasant about the taste of Joylent. My impression depends on how hungry I am at the moment: when I feel hungry, Joylent tastes good, when I am not hungry, it tastes neutral.
I guess, different people, different taste.
There are also Joylent bars.
Question(s): How does gastric bypass fit into all of this? As far as I know, it is very effective even for long term weight loss. Is drastically reduced stomach volume something that even the mighty lipostat must ultimately bow to?
As a side note, I lost roughly 60 pounds in 2013-2014 with a combination of exercise, giving up sugary drinks and reducing meal portions. I’ve since gained about 10 lbs back and while I’m not exactly struggling, losing it in the first place was definitely easier than keeping more from coming back (even while training for a half marathon as I currently am).
I seem to recall something about gastric bypass also causing some changes in microbiota, which, if they were experimentally prevented from happening in mice, would result in the mice eventually regaining weight despite a bypass surgery.
In other words, it’s possible that gastric bypass works long term for some less well-understood reason than just “lower stomach volume,” such as a mysterious change in microbiome it tends to cause.
I personally think it’s a point in favor of my “rapid, substantial weight loss is actually more effective, long-term” than attempting a very gradual change, which apparently some studies also support. If, for example, the key point is getting down to a low enough weight, long enough that the body readjusts its set point, then the key is just to get down there, by hook or by crook. Extreme measures like fasting, “eat nothing but potatoes for two weeks,” etc. may actually be better for achieving this than “slow and steady.”
That said, it does seem like “lifestyle changes” of the sort you mention are often more effective for people: not trying to eat the same foods but a little less (although you say you did this too; I, personally, find eating a little food psychologically harder than eating no food at all…); instead taking up a new exercise regimen, entirely cutting out certain foods like sugary sodas, etc. Seems to be easier psychologically.
All said and done, as the title of the book implies, it’s ultimately our pretty variable brains we’re trying to manage here, so picking a way to readjust your set point which is psychologically tolerable to you personally may be more important than anything else.
See http://onlinelibrary.wiley.com/doi/10.1002/oby.21400/abstract and http://wholehealthsource.blogspot.com/2011/07/how-does-gastric-bypass-surgery-cause.html
When I was child, my mother would often deliberately buy flavours of snacks that us kids didn’t like as much as the others. When asked why, she said (paraphrased) that “otherwise we’d eat them all”. This seemed crazy and possibly sadistic at the time, but makes some sense in the light of food reward and not overeating (which may well have been the intuition behind it).
Since we’re both anonymous you could be one of my siblings.
Typo: wife variety -> wide variety
canot, letpin x2
I thought it was funnier that way.
I was downvoted down to hell on reddit once for talking about weight homeostasis as a given… which is been my experience all my life. I don’t actively watch what I eat… my weight fluctuates very little. For Americans apparently if you’re not actively calorie counting then you will irremediably spiral into obesity.
I do cook for myself, avoid sugar, exercise and practice a sort of intermittent fasting but these are all things I’ve arrived at spontaneously, rather than as a deliberate self imposed regimen. I’m too lazy to cook twice a day (Or even every day) so I’ll make dinner once, or make a large helping that will last a few days, I let my inner satiety meter decide portions and it seems to work out so far.
I notice I tend to get fatter or thinner when I’m living with other people and lose control of food production and portioning. I also had a group of friends over last weekend and they bought a lot of food and we made meat rich barbecue… I had an urge to eat salads then next few days.
Also clearing out the sugary stuff they’d purchased I again noticed how I react to sugary foods… I like the taste of sugar fine but the aftertaste it leaves in my mouth is bleh…
I have a similar experience. The point at which I got my weight down was when the kids were at college and my wife was out of town for about six weeks taking care of her mother. That made sticking to a one meal a day and that meal not very large pattern much easier.
I’m 40 and have always maintained weight despite eating about two full bags of Doritos per week. I used to think I was some kind of freak, then I tried calorie tracking and found that every time I binged on 3500 calories of ribs one day, the next day I would skip a meal without even noticing it. And that my regular diet, with its fruits and vegetables, was not supplying me with 2700 calories a day, so I needed those 3500 calories to catch up.
I do the food variety thing, 3-5 courses per meal, but I do it really slowly while surfing the net, quizzing my satiety mechanism about whether I will or will not wake up hungry for a midnight snack if I don’t go back for something more.
One interesting thing was when my body recomposed at age 38 after I got a new job. I suddenly had visible abs with no new exercise, due to not having time to relax and eat I guess, and that change stuck even when I got back to my old routine.
> I’m 40 and have always maintained weight despite eating about two full bags of Doritos per week. I used to think I was some kind of freak
This is like, 280 Calories out of 14000. I could imagine even the weakest homeostatic impulse nudging you to balance out 2% a week (hell, even just being slightly next hungry the next morning would do it for me).
I assume Noumenon72 means grocery store bags, not vending machine bags.
I was hoping you would explore a bit more the societal implications of Guyenet’s model being correct, namely that IF hyperpalatble foods do cause a mild form of brain damage that impair’s normal decision making capabilities, does it follow that there should be a governmental response against those foods? Such as a tax or even a ban? Drugs would be an analogy here, or alcohol. For pretense of knowledge reason’s I’m not entirely sure of the answer to this, maybe obesity is entirely explained by sugar intake but it doesn’t really impair decision making that much and fat people are fat because they’re lazy, but I think it’s a question that’s important enough to devote some research time into it.
Another aspect of this is related to your Parable of Talents post. How much of obesity then is caused by the obese person’s own failings versus aspects which once established are almost impossible to counteract? Maybe trying to lose weight for obese people is like trying to hold your breath underwater. If low-IQ people aren’t to be blamed by something they couldn’t have controlled, maybe obese people aren’t as well. Perhaps more empathy is required. Or, again, fat people are just lazy, but from Guyenet’s book, Sylvia Tara’s, and my own look at some of the newest research, this idea that fat people aren’t to be blamed (at least 100 %) for their own obesity seems correct. The disclaimer here is that I am overweight myself and currently losing weight (20 pounds since September, hoping to keep it down with a combination of IF, HIT training, and not eating hyperpalable foods) [though in a first person perspective I do think I should be blamed for it, I did want to eat all those fries didn’t I? Though I would think I had some sort of choice wouldn’t I…].
How much suffering is being caused by lack of belief updating between the medical community and government officials? By television personalities and magazine articles? Coleman’s parabiosis experiments and Friedman’s discovery of leptin happened some time ago but knowledge of it doesn’t seem to have trickled down well enough.
Because you would throw up after the second one?! I literally gagged a bit at the thought of that. Oh man.
Otherwise, really good review with a good structure. I like how your section on how to reconcile the two halves of the book was timed exactly for when I started thinking “but how do you reconcile those two things?”
I was surprised by this study and am still having trouble reconciling it with my worldview:
So these people had lipostats that had adjusted to an extremely high set point, but this set point was so dependent on the type of food easily available to them that when locked in a room with only gross food, they could eat minimally and not even feel hunger? But presumably if they were out in the world and had cabinets full of nutrient sludge but knew that delicious junk food existed out in the supermarket that they could drive to, they would start feeling hunger again… so the lipostat is not only affected by how delicious the food you’ve previously eaten is, or how delicious the food that you can smell/see nearby is, but by your knowledge of whether it’s possible for you to obtain more delicious food. That’s really weird to me. But I’m very tired, maybe it will make more sense in the morning.
This matches my experience – if I only have bland food left in the fridge, or just stuff I have eaten a lot of recently, I can go sort of hungry for a long while and it doesn’t really bother me, up until the point I get super hungry and will either eat that mediocre food or go get something nicer. Whereas if I have some snacks nearby, I find even mild hunger fairly irritating.
So maybe that’s what “hyperpalatable” really means – food you’ll eat even when you’re not hungry, just because you’re bored and it’s there?
Anecdotally, I actually lost about 15 pounds when I went to college because I was on a meal plan and in a dorm with no kitchen, and therefore rarely had snack foods laying around. Despite the all-you-can eat (for 2-3 meals a day) cafeteria with not stellar but still tasty food (including a little soft serve cone most nights), eating till I was full but only a few times a day, vs constant bored snacking at home, resulted in me eating less overall.
That could also explain how people stayed thinner before despite super-rich foods… it was rich, but not convenient.
I just don’t buy snacks for the home. This has worked very very well for me and I highly recommend it: my diet preferences line up pretty perfectly with my ideal diet. The possible downside being that I just performed an end-run around having to actually have willpower…
I don’t keep food at home that can be eaten without preparation. The closest I can come to a “quick snack” is a slice of toast, and even that requires at least planning and setting portion size a few minutes in advance rather than just reaching into a bag of chips.
And after losing about seventy pounds, I rebounded ten when I took a job where there are vending machines just down the hall.
And mine. I’ve found that I was losing weight when I had only a tiny fridge, and bought enough food for one day only, every day. But when I have a smorgasbord of various delicacies stored up, I’ll gradually go through them even if I’m not really hungry.
Although now I think about it, there’s a lot of stuff about diets not working long term. Has anyone tracked this including *why* people fall off a diet?
Do they keep eating the same amount but put on weight anyway? (Probably not?)
Do they get hungrier and hungrier until they can’t stand it? (This is what “diets don’t work” would predict.)
Do they get bored of the monotony, go back to eating a normal variety of food, and *then* find they can’t restrict the amount any more. (That would fit the theory in this article.)
The nutrient paste thing makes it sound like “eating a boring diet” could work. I could easily imagine that — I keep giving in to wanting food variety, but I could easily imagine eating meal squares and eating one or two nice meals a week, if the standardised food product was easy. But other indications suggest maybe it doesn’t.
I have an anecdote about this.
I (thanks to a weight loss competition at work) started eating a pretty standard set of meals (chicken, spinich, an apple, and a greek yogurt) for lunch and dinner (and I would not eat any of the snacks/donuts people brought into the office). In addition was going to crossfit 4 to 6 times a week. I lost 50ish pounds and was in much better shape. About 8ish months into my diet push, my girlfriend broke up with me and as a result I began going out much more on weeknights (which meant I was not able to go to the gym) and I got out of my habit of cooking my meals for the week on the weekend and I started eating out (and drinking) more in the evening and no longer bringing my healthy lunch to work.
I am trying to get back into it, but once I broke the healthy habit it is much harder…anecdotally I have heard of similar reasons, you break the diet/exercise habit for one reason or another (vacation, injury/illness, the holidays, etc.) and suddenly it is really hard to get back into it.
While we are on anecdotal data, this time on individual variation.
If I want to lose weight, it’s pretty simple–one meal a day, and make that reasonably light. That got me from about 200 to about 185 some years back. To stay there, I eat one meal a day, not especially light, plus some occasional nibbling–on the two days a week I teach I usually buy myself an apple fritter in the afternoon.
Hunger, for me, isn’t a relevant constraint–I may start feeling a little hungry in the morning but if I ignore it the hunger goes away. The two things that make keeping my weight down or getting it lower difficult are the tendency to eat as an excuse to take a break in what I am doing and the fact that I enjoy eating.
My wife, on the other hand, gets seriously shaky and indecisive if she goes without eating for too long, where my standard pattern would be much too long for her.
The second most weight I’ve ever lost was when I was living a healthy and well-adjusted lifestyle for several months with regular exercise and good sleep and strict calorie counting.
The most weight I’ve ever lost was when I was living an unhealthy and poorly-adjusted lifestyle for several months because of bad anxiety. I would order my favorite foods and stop eating after a few bites, because even though it tasted delicious I just didn’t want it. I had a messed-up sleep schedule and fidgeted constantly and ran back and forth around my house.
Now that I’m feeling better I’ve gained about half of the weight back, but I seem to have a new set point about ten pounds below where it had been since I was teenager. I eat the ice cream and cookie dough I love and somehow still haven’t broken past the barrier. It’s honestly kinda weird.
From personal experience, its declining motivation. When I look at the mirror and dislike what I see, I become motivated for change. The motivation helps me restrict my diet. As I loose weight, I become more satisfied with my appearance, and less motivated to deprive myself of tacos.
More anecdote: Boring diet would work for me, but only insofar as it was 100% standardized.
For this category of thing, it has to be “I will eat x grams of nutrient paste and nothing else for breakfast every single morning period,” so that there is no decision to make whatsoever. If I can enforce that for a while via willpower, it just becomes a habit and I don’t think about it anymore.
But if I allow any kind of decision, I am very clever at mobilizing a pattern of reasonable “one-time only” justifications that result in slowly moving away from my plan. Allowing a skipped breakfast due to lateness (with tasty snack to make up later) will result in me unconsciously contriving to be late more and more frequently. Generally, allowing any exception for [reason] will result in a much greater incidence of [reason] and situations similar to [reason] in the future. Allowing small exceptions will be used as mental justification for allowing larger exceptions later.
This worked for me to quit smoking. After dozens of failed attempts at rationing nicotine via various devices or plans, I took the opportunity of moving house to simply 100% quit nicotine cold turkey period. Which turned out to be much more effective than any of the half-measures (though still difficult and unpleasant – don’t smoke). Worked for exercise too.
Wow. OK, firstly, yes, that comes closer to sounding like a decent summary of the expert wisdom that actually sounds like it plausibly fits what’s going on I’ve heard for ages.
Several times you mention “very tasty” or “deliciousness”. Were there more details on that? Because some things, like variety, definitely sound to play into food-reward and also general enjoyment. But are they actually the same thing. How much of the reward value is conscious enjoyment, and how much is subconscious stuff. Like, some food is more-ish, and other you really value afterwards and those don’t need to be exactly the same.
I’m amused that Gladwell’s reputation is so poor around these parts nowadays that we basically use him as a byword for dilletante.
I knew history would absolve my decision to make Standardized Food Squares bland, but I assumed the recognition would be posthumous. How sweet to see it in my lifetime, but not so sweet as to encourage gorging on the validation.
Given ai concerns in addition, it looks like tuning reward loops might be the conflict that defines the century.
I take it your romeo of romeo at StandardizedFoodSquares.com? Looking forward to my first shipment!
One thing that always bothered me about the data on CICO, is that obesity is reported as a fraction of population being obese (or overweight), while calorie intake and exercise is reported as an average. It is not hard to imagine a situation where the obesity fraction increases while average calorie intake decreases, even if the CICO-model is true. In my experience, using such data to debunk CICO is pretty common, and to me it smacks of scientific dishonesty. But perhaps I am being ungenerous, is there a reason for doing it this way?
(And of course, people are notoriously inaccurate and in many cases they downright lie when surveyed about eating habits. But that’s another story.)
E.g. http://www.huffingtonpost.com/2013/03/07/calorie-intake-decreasing-consume-fewer-obesity_n_2824771.html. But in reality, obesity seems to be pretty well correlated to average calorie intake.
Related, people underreport what they eat by as much as fifty percent(!), so the apparent decline in calorie intake is probably not real. Underreporting could be a result of shame, but perhaps it reflects different eating patterns, with more between-meals snacking (which is easier to forget about)?
https://www.ft.com/content/2d1e9a02-5b43-11e6-8d05-4eaa66292c32
Small stuff adds up but is forgotten, and people are not aware of caloric content. “Merely a salad” often includes bacon or cheese strips and a tasty sauce with much sugar which don’t make it into awareness as ‘calories’.
Well, a good Cobb Salad at a restaurant can run as high as 1400 Calories. There is still a lot to be said for portion sizes and education about the Calories present in your meals. Although our host may reject the strong CICO hypothesis out of hand, Calories remain a useful tool for measuring intake.
(Plus, I don’t know how we get away with calling chicken strips and a sugary vinaigrette over a bed of lettuce and spinach a “salad”)
I didn’t realize until I started tracking, which is a lot easier with a smart phone.
What would be even easier would be if I could just take a picture of the food, and then software (perhaps with remote human assistance) could figure out just how big that pork chop or bowl of cereal is, within 5%.
The ideal — for weight loss, although not for privacy necessarily — would be an intelligent agent hooked up to Google Glass that monitors what I eat and helps me plan when to eat. If I say “I’m hungry” it can say “okay, eat an apple” or “wait an hour and eat your standard sandwich. I’ve already talked with the smart fridge to make sure there is lunch meat available.”
Left to its own devices, my body is very good about making up excuses that I need to eat. A coach that says “don’t worry about that, I’m monitoring things instead, I promise it will be okay” would help with willpower.
I don’t think people underreport their consumption out of malice, or are in any way deliberately lying, even as a form of ego-protection. I don’t think shame has much to do with it. There are too many people who too consistently underreport. There are so many people who flat out seem unaware that they are overeating. Like being obese was just an affliction that snuck up on them in their late twenties, a curse detached from all of their eating habits, targeted at some mythical “metabolism”.
I think those people ate rather normally — until they became saited. Maybe only slightly overeating in their teens. Just that the ammount of food it took to sate them increased over time as they built up tolerances to leptin. Throw in the stress of grad school/white collar work, and the endocrine affects of binge drinking, and you have someone in their late twenties who is well into the obese catagory.
@Siah Sargus :
In Fit Or Fat, Covert Bailey had a plausible-seeming theory about that. He thinks what happens (especially with guys) is that as they age they gradually get more sedentary or eat more or both such that they are becoming less fit, but there is a long time delay between that change and visibly “getting fat”. You could go a couple years merely getting less fit, putting more fat on in places where it’s hard to notice. Getting more “marbled”. It’s only once that process passes some threshold that you start to get a visible “beer gut”, and by the time that happens there’s no immediately prior change in behavior. At the time you go from being invisibly fat to visibly fat, there’s no trigger to explain it – it just “snuck up on you”.
I think there’s likely an element of ego protection for a lot of people at least in that most people don’t investigate their calorie intake. Most people estimate without investigating, and in my experience, many show a level of anxiety around rigorously investigating which suggests that on some level they’re aware their estimates could be way off.
Charles Duhigg’s The Power of Habit mentions that in studies on dieting, apparently keeping a food journal was the most effective intervention of all. I’m guessing a factor is how most people just don’t grasp how many calories they’re taking in throughout the day, and keeping a journal remedies that.
I’ll excerpt his cited sources:
“4.24 Then, in 2009 a group of researchers J. F. Hollis et al., “Weight Loss During the Intensive Intervention Phase of the Weight-Loss Maintenance Trial,” American Journal of Preventative Medicine 35 (2008): 118–26.
See also L. P. Svetkey et al., “Comparison of Strategies for Sustaining Weight Loss, the Weight Loss Maintenance Randomized Controlled Trial,” JAMA 299 (2008): 1139–48;
A. Fitch and J. Bock, “Effective Dietary Therapies for Pediatric Obesity Treatment,” Reviews in Endocrine and Metabolic Disorders 10 (2009): 231–36;
D. Engstrom, “Eating Mindfully and Cultivating Satisfaction: Modifying Eating Patterns in a Bariatric Surgery Patient,” Bariatric Nursing and Surgical Patient Care 2 (2007): 245–50;
J. R. Peters et al., “Eating Pattern Assessment Tool: A Simple Instrument for Assessing Dietary Fat and Cholesterol Intake,” Journal of the American Dietetic Association 94 (1994): 1008–13;
S. M. Rebro et al., “The Effect of Keeping Food Records on Eating Patterns,” Journal of the American Dietetic Association 98 (1998): 1163–65.
4.25 “After a while, the journal” For more on weight loss studies, see R. R. Wing and James O. Hill, “Successful Weight Loss Maintenance,” Annual Reviewof Nutrition 21 (2001): 323–41;
M. L. Klem et al., “A Descriptive Study of Individuals Successful at Long-Term Maintenance of Substantial Weight Loss,” American Journal of Clinical Nutrition 66 (1997): 239–46;
M. J. Mahoney, N. G. Moura, and T. C. Wade, “Relative Efficacy of Self-Reward, SelfPunishment, and Self-Monitoring Techniques for Weight Loss,” Journal of Consulting and Clinical Psychology 40 (1973): 404–7;
M. J. Franz et al., “Weight Loss Outcomes: A Systematic Review and Meta-Analysis of Weight-Loss Clinical Trials with a Minimum 1-Year Follow-up,” Journal of the American Dietetic Association 107 (2007): 1755–67;
A. DelParigi et al., “Successful Dieters Have Increased Neural Activity in Cortical Areas Involved in the Control of Behavior,” International Journal of Obesity 31 (2007): 440–48.”
This is my cue to anecdotally report that the following variation has been working well for me: my wife and I made a pact that before eating or drinking anything, we take a picture of it and send it to a WhatsApp group for just the two of us. I could never convince myself to keep a food journal (awkwardness, trivial inconveniences), but this is just 3-4 clicks on the phone that’s always with me. It’s working pretty well so far to motivate me to avoid second helpings and to stay on my diet.
This highlights the problems with using vague terms like “establishment” which equivocates between the views of top researchers and the often outdated or misunderstood conventional wisdom habitually pushed around by educators, practitioners and the educated public. Information transmission from the ivory tower to the public square, from top researchers to the merely well-informed, is much more indirect and buggy than we think – so they mustn’t be conflated.
What Gary Taubes et al. protest against might not be the consensus among nutrition scientists, but it certainly is alive and well (slightly less well now, but that’s partly because of people like him) in the public arena. Lots of direction-pushing narratives like that seem to come about as a corrective to what’s already out there. The problem is, if people disagree about what’s “already out there” (which is increasingly the case) they’re going to interpret a corrective narrative in different ways – if you come across a narrative meant as a counterweight to another one, without absorbing the other one first, it’s going to appear ridiculously lopsided and partial (a typical example is Ayn Rand’s philosophy, and postmodernism as a reaction against modernism and premodernism). I think both “it’s all CICO and willpower” and “it’s all insulin resistance” should be seen somewhat in this light.
Hell yes. This is the thing I want to shout from the rooftops (and did just yesterday). And it’s not just nutrition, this applies to everything (and with other kinds of difference, not just genetics). One-size-fits-all as the default assumption is doing a lot of damage in many places, and we’d do better if we could keep “people are different” as the default assumption instead.
For many years I’ve been telling people online that drinking echinacea tea when I feel a cold coming on often helps me avoid the cold. But I can’t recall anybody ever responding with a thank you email for such a great tip about echinacea. Presumably, it simply doesn’t work for most people the way it works for me.
On the other hand, I didn’t come up with the echinacea idea completely out of the blue, and Whole Foods continues to stock echinacea tea.
So echinacea probably works for some quite small percentage of the population the way it works for me and doesn’t work for most people.
I find that a lot of people seem to feel that that idea that some things work for some people and not for other people is Not Science. To be Science, the feeling goes, something has to work for everybody or nobody.
But say I came up with a diet that works great for 3% of the population, while making 3% fatter, and not having any effect on 94%. To a lot of people, that seems like Not Science. But it could be pretty helpful for 10 million Americans.
There are some fields, such as cancer-fighting regimens and psychiatric drugs, where the problems are so severe that scientists look for any upside even if the net is not statistically significantly positive. But we don’t seem to apply that mindset to diet.
@Sailer
Theoretically you could measure that scientifically. Assuming that every population has a X% of people who gain weight and Y% who lose weight, you’d be able to measure X+3% and Y+3% given a big enough sample and control group.
However, this is not true:
Unless you can actually figure out in advance or during the diet whether someone is part of that 3% that benefits.
The main reason is probably that people don’t stick to diets very reliably, so almost all of the outcomes will be random noise.
A major problem is that the study designs and statistical tests we typically use in nutrition/medicine/psychology etc. assume that people are all the same and differences are random noise. They’re designed to find out the properties of “the generic human”, but if that human doesn’t exist – the data cloud representing humans isn’t “a center plus symmetric noise” but rather a complex internal structure with clusters and such – those methods eventually stop giving coherent results at a certain resolution.
Maybe we’ve hit a limit and need to work out methods that take such concerns into account.
This is unduly optimistic. We know perfectly well what needs to be done. For population studies, everything must be within-family, or with polygenic scoring with Mendelian randomization, to at least reduce familial/genetic confounding; for individual correlations, use pairs of identical twins; for permanent interventions requiring between-subject designs, randomize pairs of identical twins (since for many traits eg height this requires as little as ~1/20th the sample size due to drastically increased statistical power due to identical twins having such little variance); for temporary interventions, use randomized within-subject longitudinal designs. You can see Bouchard using some of these better methods in OP.
Nutrition researchers know, or should know, all of this, but the incentives are not there to do the high quality studies rather than re-analyze yet another survey to show that soda consumption is as bad as tobacco smoking.
Who are “we” here? It’s clear that you know but I’m skeptical that understanding is universal – by “work out” I meant something more like “make into standard practice” than “invent”. But as you say the incentives don’t seem to be there and we get 100 substandard studies instead of 5 good ones. Too bad.
The key need/challenge here, speaking from the perspective of a clinical trialist (in oncology) is to develop a predictive biomarker – something you could measure or detect that tells you which group you fall into, and predicts the response to a particular treatment. If we can identify people who are most likely to benefit in advance, we can tailor the treatment (or diet) to the patient, and even treatments that only benefit a small percentage of people become valuable.
It would be extremely useful to have better predictive methods for which psychiatric drugs to try on different people in different orders.
Definitely agree with the first part of this (I usually encounter disconnects like this on various political/culture-war-type topics).
But I’ve never understood the idea that a counternarrative is justified in going too far in the other direction as a corrective. Shouldn’t you always try to approximate the actual truth with all its nuance as well as possible regardless of what everyone else is saying? Moreover, aren’t people more likely to listen to you if you don’t ignore the benefits of the prevailing theory, since the inferential gap will be smaller and people won’t have to throw out all of their beliefs at once?
Absolutely. It’s probably one of the more important factors driving “culture wars”.
I totally agree that corrective argumentation isn’t a good thing and that you should try to have as full a picture as possible. But it’s hard to avoid in practice* and I think it’s less damaging in a relatively culturally homogeneous environment when at least everyone understands the background. In combination with filter bubbles it creates a reinforced oscillation of the kind that destroys badly designed bridges.
As to why corrective narratives are more popular than nuanced integrated ones, I think they might simply be easier to understand – they can often be parsed in a “these concepts that have positive affect should have negative affect” way that makes minimal cognitive demands while naturally falling into black-white dichotomies. Also, ideas that lend themselves well to identity formation (clearly distinct from the mainstream) has a head start. Plus, being a “rebel” can be attractive.
If anyone knows about any research or philosophy on this I’d be grateful for some recommendations.
*If I believe “A and B”, and people around me keep saying “A!”, “A!”, “A!”, “notB!”, “notB!”, “notB!” all the time, I’m going to want to say just “B” and not “A and B” because there is a limit to how much time and energy you have for conversation and by saying “B” when it’s underdefended I bring the memetic environment in line with my own preference as effectively as possible. But yes, ideally I should say “A and B”. The likelihood of me saying just “B” probably goes up as the communication bandwith goes down. In a private conversation I’ll say “A and B” but in the cacophounous world of public debate when few people are barely paying attention and you can’t rely on complex information being transmitted with reasonable fidelity most people are going to go for “B”.
My parents got their first microwave oven in 1980.
Food was a lot more work to prepare in the past.
Maybe we should make a fad diet where you are only allowed to heat your food through one of the four means each month, to reduce someone’s reliance on microwave dinners?
I think that the most weight would be lost during the “induction” month.
Eat food with high iron content ? 😀
Although TBH I don’t believe it’s possible to eat food that has been heated without the intervention of conduction. Whatever mean you use doesn’t uniformly heat the whole thing at the same time.
I am curious how the lipostat theory works with fasting. Fasting theory is that you can eat similar kinds of foods as before, but within a restricted window of time. The theory is that this leads to fat burning when your glucose level decreases.
How does the lipostat theory interact with the theory behind fasting/intermittent fasting/similar types of diet scheduling?
There are two sections labeled IV.
And the section after is labeled V, so it needs renumbering as well.
It’s intentional to mess with your reading lipostat, so you’ll read to the end.
I don’t think it worked. I don’t feel sated. I’m shamelessly binge-reading junk comments.
…aren’t we in the middle of a browsing-reddit-all-day-instead-of-working epidemic? One man’s modus ponens is another mans modus tollens. Maybe the analogy to obesity means we should be taking internet addiction more seriously. Feeling smug rarely helps.
Yeah, this was my reaction too. We have the same thing going on with deliberately engineered maximally addictive Internet stuff as we do with deliberately engineered maximally addictive food. And if someone (uh, me) has more trouble than usual moderating one’s intake of one or both, I guess that’s part of their “character” in some sense but it’s also not very much under their control and it doesn’t make sense to judge them for finding things hard.
A scary question: for how many of us commenting here, this blog is one of those things?
yup
Paul Graham has an essay about how (basically) everything in society is becoming more addictive
http://www.paulgraham.com/addiction.html
Eating too much makes you fat. Browsing reddit all day instead of working makes you…? Productivity isn’t down (it’s flattening a bit), so it appears overall it’s fairly harmless. Probably reddit is just substituting for hanging around the water cooler, making rubber band balls, taking frequent smoke breaks, and all the other ways we were unproductive at work before.
Unemployed, in the worst case.
There has been an economics puzzle as to why we didn’t see much productivity gain from mass computerization, when computers are obviously really really good. It seems plausible that there was a huge gain, and it was just offset by a huge loss due to functional internet addiction.
Wouldn’t this predict peaks and troughs of productivity, where people implemented computers in areas where they also needed internet connection, so no gain, but certainly lots of computers are also implemented in areas where we restrict internet access, so they should be seeing the huge productivity spike from computers.
What if people have a work ‘set point’ at about how much work they think they should be doing. When you give them tools that will make them more efficient they will just take their new found free time and waste it.
You may not recall this, but computers predate the internet, never mind the commercial and social internet.
Which is probably why you heard a lot more about Solitaire and Minesweeper back then.
To be fair it wasn’t really common for every single office worker to have a computer on their desk until right around the time the commercial internet took off.
OK, but assume you manage to get enough work done to remain employed. Then what harm does it do?
I think more plausible is that computerization moved the productivity bottleneck from paperwork to other things (or it never was paperwork). This left workers with free time at work. If they’d let on, this would have resulted in more makework (by Parkinson’s Law), or on layoffs (which might not have worked to increase productivity, depending on what the bottlenecks are), so instead they recaptured some of that surplus time by wasting it on the Internet.
It’s just generally an inefficient use of time. If that’s something you think matters. Fat or lazy or whatever, we’re all going to die and nothing matters in the end, so nothing can possibly do any harm, from that perspective.
I am. I can’t get out of bed without an hour of 4chan every morning. Putting the phone far away just makes me go get it and bring it back to bed.
This largely squares with what I’ve been thinking, and believe it or not, McDougal and co. have, actually, kind of invented the “bland food cookbook,” based on their somewhat somewhat similar “pleasure trap” idea (the problem is hyperpalatable/calorically dense food in general). Of course, they don’t call their diet “the bland food diet,” they call it “the Vegan SOS-free diet” (where SOS stands for “sugar, oil, salt,” i.e. all the things that make things delicious).
The big question this leaves for me is: didn’t we know how to cook 100 years ago? I have a lot of pretty old cookbooks. Like early 20th c. cookbooks (admittedly, they tend to be from Louisiana, which may not be a typical food culture), and they are, if anything, even worse, seemingly, than today’s cookbooks. A typical recipe from 100 years ago seems to be something like: “melt one stick butter over medium heat; add fish fillets and fry until brown. Remove fish and set aside. Deglaze pan with brandy and add four egg yolks. Season with salt and pepper to taste and serve with potatoes au gratin and creamed spinach.” It’s not just more fat; it’s just like the type of cookbook you’d expect people to write if everyone was super skinny and had never heard of cholesterol.
My best guess is that this was “special occasion food” and people went back to eating boring stuff the 350 days out of the year that wasn’t Christmas, Thanksgiving, or guests for dinner. And of course the variety was less and the price higher and the convenience lower, etc.
But makes me doubt that hyperpalatable is the only culprit. Cheap, easy availability of a wide variety of foods may be worse. Which confirms my sense that the “food pyramid”-type charts are more harmful than helpful: looking at these things gives you an impression that you need to eat a really wide variety of foods every day or suffer potential malnutrition. Yet these native populations eating only nuts and bear fat do better than us in many cases.
And then there’s everyone quitting smoking…
They may have had fattening recipes and fattening ingredients 100 years ago, but they also had like four spices and six ingredients in the cupboard, as well as no possibility of Mexican tonight, kebabs tomorrow, Chinese the day after, and Italian the day after that.
Personally, if I had to eat only Mexican food this month and only Italian food next month, I’d probably find it harder to gain weight than if I were allowed to freely alternate them. You get tired of a certain set of ingredients, but life today is an endless, multi-ethnic buffet.
Maybe I should write a cookbook, capitaling on the minimalism trend, called the “10 ingredients per month” diet, or something. Since pretty much any weird way of restricting one’s diet works for a little while, I predict it will be a big hit.
I can’t speak to a hundred years ago, but a thousand years ago they had quite a wide variety of spices, and continued to do so for at least the next six centuries, that being roughly the span of my historical cooking. Of course, that describes the situation for the upper class, which is where most of our early cookbooks come from. Were medieval aristocrats typically fat?
They had a pretty wide variety of ingredients too, but more of a seasonal restriction than we have.
AFAIK, yes.
(To be clear, they would be ‘mildly overweight’ by today’s standards.)
I don’t know about medieval aristocrats, but starting from the Renaissance, when realistic painting became popular, aristocrats often look fat. And there are historical records of them suffering health problems (e.g. gout) due to unbalanced diet.
Some Egyptian mummies show signs of diabetes, such as clogged peripherial arteries and amputated toes.
Anyway, at least during the early Middle Ages, where religious dietary restrictions were strictly observed, aristocrats might have fared better.
Why did you reply to yourself?
Also, I think “bland” may be insufficiently precise terminology. as the anecdote about paleo dieters notes, the various diets people embark on can still contain plenty of pretty tasty food like steaks and butter and whatever, but as nice as those foods might be they still won’t compare to the engineered deliciousness of a mcdonalds french fry, or an ice cream sundae, or a dorito or suchlike. Bland doesn’t mean tasteless, it means not ruthlessly optimised for taste. If you think to food that you have cooked, has it ever been inescapably moreish? If I cook a lasagna, it might be delicious but I’m only going to have one piece before putting the rest in the fridge. Not so with snacks you might buy at a supermarket.
I’d imagine that some of the factors you identify, like variety, price, convenience and occasion all played some role in low incidences of obesity as well
I replied to myself because I was unable to edit the original response. It was within the window, but I had switched to another computer.
I am using “bland” here ironically/jokingly to mean “food which hasn’t been optimized for deliciousness.” There are many fresh fruits I enjoy quite a lot, and which possess many interesting flavors, textures, etc. but it’s still hard to compare them, in terms of pure eating pleasure, to say, a chocolate chip cookie. On this definition, the fruit is “bland” and the cookie “optimized for deliciousness,” even if the fruit actually has more complex flavors than the cookie on some objective level.
The food I cook for myself is at least as addictive, to me, as most fast food. But then, I have optimized my recipes for deliciousness as perceived by me.
Still, I’m probably healthier when eating my own cooking, since I am more conscious of what I put in it: restaurants tend to “cheat” by adding more butter, salt, and sugar than I would, in good conscience, usually add to food myself.
Thinking recently about what it means “to optimize for deliciousness,” I was interested to learn that many of the condiment-type items world cultures add to food to give it that extra, savory kick are actually high in glutamate, i.e. natural MSG: parmesan cheese, worcestershire sauce, Thai fish sauce, and, of course, the original source, Japanese seaweed-bonito broth.
Those who worry about MSG claim it is an “excitotoxin”: almost like it “burns out” your taste receptors like loud music. But if that were true we’d expect obesity to be worse in Asia, at least if “burning out your taste buds” had any effect on weight set point.
I would also rate the food I cook as being superior to eat than various snack foods, but my point remains that with the former I simply cannot eat than a standard serving. If I made a chili to a recipe of 6 servings, then chances are I would get 6 servings from it even if I ate it myself over several days. I could not imagine forcing myself to consume the entire thing within one day.
Conversely, I can and have eaten an entire packet of oreos in an afternoon, when they should ostensibly last several days. I don’t even particularly like oreos against any other biscuit or confectionary item, but something about them makes it easy to consume again and again.
Personally, I find it much easier to rapidly consume a large number of home-made cookies as compared to any pre-packaged cookie.
The one exception is those little powdered doughnuts. Those are made of crack or something.
@onyomi: I’m glad I’m not the only one. I can’t buy them anymore, they’re gone within a couple of days.
Snacks are not only optimized for high deliciousness, they are also optimized for low satiating power, so you can eat a ton of them and let the snack companies make big bucks.
Homemade food, when highly delicious, is often also highly satiating.
@vV_Vv
To second your point. It is not about snack foods being particularly delicious, it is a combination of not being very satiating, being pretty tasty, variety of flavors, and I think very important, but kind of glossed over here, ease. I would eat my own cooking over almost any fast food/snack product, but it is dramatically easier to eat fast food/snack products, which is another axis they have been optimizing on.
I spent my early 20’s on a steady diet of junkfood. Mostly sonic double burgers. Naturally, there was weight gain. However, eating the same thing for lunch and dinner day after day meant there was relatively little variety. Why didn’t my brain get brain get used to sonic burger and stopped thinking of them as a trap?
My grandma’s recipes from the mid-20th century did tend to be calorie-dense (plenty of butter, corn syrup, Crisco), but they were also designed to feed six boys on a middle-class salary with mid-20th-century food infrastructure, so they usually used canned or bulk ingredients, didn’t take much individualized preparation, and didn’t use spices or, for much of the year, many fresh fruits or vegetables. They were good in a sticks-to-your-ribs way, but very much not flashy; breakfast Monday through Saturday was plain oatmeal with a pat of butter and a peach or plum in season, for example, with pancakes, sausage and bacon on Sunday.
This doesn’t fit very well with the fat or carbs superstimulus theory, but it fits reasonably well with the flavor superstimulus theory, I think.
Probably because everyone was super skinny and hadn’t ever heard of cholesterol.
But seriously, part of me thinks that the average person 100 years ago just did so much more physical activity that the “excess calories” would probably get used, especially since many people did manual labor for work. This reminded me of a scene from this video about Maine log drivers from 1930.
I’m interested to know how does fasting come into play in the lipostat model. I haven’t read a lot about fasting, but it seems that some nutritionists and doctors do recommend fasting as a weightloss strategy (i think its called “intermitten fasting”).
Obesity is, as always, a very complicated issue. If “not hyperpalatable” food is one of the keys to combat obesity, how should any government legislate policies to advocate that? Are existing policies futile?
Obesity, of course, brings a lot of health problems, and medical expense (although some dispute whether the extra expenditure is more than the amount their earlierdeaths cut), and “reduce competitiveness”, “lower quality of life”. So should governments “intervene”? If governments do ought to maintain the quality of public health, and even improve it, what can governments do?
I have travelled a few times to the US and still can’t wrap my head about how incredibly tasty is the snack food there. Every time I try an american Dorito is like an explosion of flavour in my mouth and nothing I can buy in an European store can compare. The same happens in different ratios with fast food and pre-packaged food.
So, whats happening?
1) Is a cultural thing? Maybe at some point the American snack companies tried to introduce this kind of thing into Europe and the test groups were like “nah, too tasty”. It sounds like an un-human thing to do. I kind of got weirded out the first time I tried some, but I got used to it really fast, like, by the time I finished the first bag I already loved them (it helps that the American servings are just huge).
2) In Europe is already regulated? Maybe the chemicals that make the American snacks taste so good are banned in Europe, or there is a maximum of salt you can put in a serving, or something.
I’d love to get lost in the internet looking for an answer, but I don’t have the time and a quick google search does not reveal anything but buzzfeed-like anecdata, so if anyone is willing, looking for the European vs American differences in snack food might be a lead.
Good question.
I knew people who worked at the Frito Lay Corporation and they would have appreciated your appreciation of Doritos. A lot of effort is put into flavor engineering American foods.
In general, American foods seems tastier today than when I was young. For example, pizza in Los Angeles is much better than in 1975.
I’ve noticed the same thing with desserts. Europe seems to have a set limit on how good a dessert they are willing to serve.
Maybe they need more growth mindset.
This might be the nost SSC comment ever
Girth Mindset?
The longest I’ve ever been outside the US was a semester in Israel. By the end I had this intense, persistent craving for peanut butter Ritz Bitz. Which is weird because I hadn’t eaten any for at least a year before leaving the States. But I would daydream about them, and I could practically taste the salt.
Also there were no brownies. Mostly there were bland dry cakes.
Not just Europe, either. I’d long heard that the only country to have completely lapped the USA in snack food technology was Japan, and it’s true that if you can find a Japanese grocery you’ll step into a Wonkan cornucopia, an insane profusion of brightly colored foil packages, each with their own kawaii mascot.
But most of the stuff I’ve tried, shrimp puffs to mochi, just seems so… subtle. Nothing like the brisk slap across the face you get from a Spicy Sweet Chili Dorito.
This is my experience as well, but to be fair, if I let myself I could probably eat shrimp chips all day. I find them much more appealing than most American snack foods.
On the other hand, I seem to have a significantly easier time regulating my weight than many people do (I gained significant amounts of fat early in college with a transition to dramatically worse eating habits, but manage to lose it all relatively quickly when I put my mind to it, although it took hard work.) Maybe the facts that I find shrimp chips more appealing than Doritos, and that I generally don’t struggle to maintain a healthy weight, both have a common cause.
When I am eating a bag of doritos they are the best thing ever and I can’t wait to have another one. But I don’t have any cravings for them on a day to day basis. In fact, right now the idea of eating one seems vaguely gross.
That’s not the same thing with say ice cream, which I have a steady desire for that is sometimes resisted and sometimes not. I don’t know why the difference exactly.
This is my experience. Doritos aren’t something I crave. I don’t really crave processed snack foods in general. But if you put them in front of me I will just slam them down.
If I open a bag of barbeque Fritos, I am eating every last one of them, including the dust, including your fingers if they get in my way.
I don’t buy them any more.
I have close to precisely the same experience with the chips they serve at Mexican restaurants – it’s not even that they taste good (I have yet to actually try the salsa they come with), but after starting it’s difficult to stop.
On the other hand, after noticing this I elected not to start eating them on subsequent visits, which has worked pretty well so far. It has yet to generalize to restaurants that serve dinner rolls, though.
There’s exactly one flavor of Doritos I can stand, and the rest taste like snorting concentrated flavor powder through a rolled-up hundred-dollar bill. It’s not pleasant. Maybe whatever makes me feel this way is more common in Europe?
That’s funny. When I travel to the States I generally eat eat healthier than I do at home because I can’t stand how sweet most of the processed food is, (excluding New York bagels), and thus wind up living off salads and raw nuts and the like (and bagels). When I was there for three months I actually dropped a couple of dress sizes.
Also Americans don’t do salt &vinegar crisps. (Or at least I have never found any). You can’t be at the forefront of snack food if you don’t do salt & vinegar crisps.
They don’t? They’re common in Canada.
They do show up sometimes, but my impression of the “standard” flavor options has been “barbecue” and “sour cream and onion” (note: I do not buy potato chips, so take the anecdata for what it’s worth).
Contrast with New Zealand, where “lamb and mint” chips were ubiquitous.
They also don’t have ketchup chips. Or all-dressed chips.
The potato chip gap between Canada and the US is surprisingly large.
Which makes me think that in terms of “explosion[s] of flavour”, Canada is way ahead.
Frankly, ketchup chips should not be legal. They’re like crack but without the barest possibility of health benefits.
I actually saw all-dressed chips in my grocery store for the first time last weekend. I’m not much of a chip-eater, and I try not to be taken in by flavor novelty marketing, so I passed them by, but if some Rand on the internet says they’re good…
Bagged salt and vinegar potato chips are pretty common, at least where I’m from in the States. Delicious combination.
Yeah same here. WalMart has I think literally a dozen flavors of regular Lays, not including the wavy, kettle chip, and ruffled varieties.
Best ones are the Mexican flavors, particularly Chile Limon. Those may not be available nationwide. Salt and Vinegar isn’t the most common, but it’s hardly rare. Without looking it up I’d guess the ranking goes plain->bbq->sour cream and onion->salt and vinegar. Cheddar cheese is probably in there somewhere, and jalepeno is a popular newcomer.
Lays does a flavor contest every year or so, often with some oddities (e.g. chicken and waffles). Out of the last batch, the “reuben” flavor was pretty good I thought. Not much “beefy” but definitely pickled/sauerkraut flavors, caraway, and a bit of swiss cheese.
I thought the biscuits-and-gravy chips Lays was testing a couple years ago were pretty good.
@gbdub
“Lays does a flavor contest every year or so”
I wonder if they turn around the
“Then, almost by accident, someone tried feeding the rats human snack food, and they ballooned up to be as fat as, well, humans.”
– and do a preliminary screening of possible flavors with
rodent weight gain as the assay criterion? 🙂
Why bother paying for rats when you’ve got so many human volunteers?
Salt-and-vinegar was a something you could get in the Midwest 20 years ago and is gradually spreading to the rest of the US.
Salt and vinegar was certainly available on the east coast over 20 years ago. Well, at least Maryland, which may have been considered a good market because of the popularity of vinegar fries. But they’ve been available in Philly and NYC areas for a long time as well.
BTW, salt and vinegar chips might be better called sodium diacetate chips, but no one would buy them if they were. Though perhaps “salt OF vinegar” would work.
I eat salt and vinegar chips all the time. They seem to be a love-it-or-hate-it thing among Americans, but there’s a high enough “love it” fraction that they’re easy to find in stores or e.g. delis.
Might be a regional thing, though. I’ve never seen crab chips on the West Coast or jalapeno on the East, for example. Canadians like ketchup chips, which is just bizarre to me.
Jalapeño chips are fairly common in Philadelphia, or at least south Philadelphia.
I haven’t tried ketchup chips (actually haven’t noticed them for sale), but people put ketchup on french fries, so it doesn’t seem totally unreasonable.
I love them right up till they strip the skin off the entire inside of my mouth.
Philadelphia also has a brand called Herr’s that does the best salt and vinegar chip I’ve ever found: it’s got unbelievably strong flavor, almost to the point of burning as you put it on your tongue (this is more delicious than it sounds)
I had to quit buying them because I couldn’t stop eating them.
Are Miss Vickies common in the US? Their salt and vinegar chips are good.
Ketchup chips are great. I don’t know why they’re an only-Canadian thing.
Based on comments here, my opinion of American snack food has just gone up sharply. So hey, I learnt something today.
Interesting, I don’t like most of American snacks (also not born in US, though living here for a while). The Doritos and other things like that are kind of addictive, and it can be hard to stop eating them if they are laid out in front of you on a table, but I don’t really like them and never buy them for myself.
Same for many other US foods, especially fast foods – they seem too salty, too sweet, too spicy, too… well, many things, for me. Fortunately, the variety of flavors, especially if you are willing to do a little internet searching, is awesome, so it’s possible to find one for virtually every taste.
But I don’t think this kind of preferences is exclusively European, I’ve never lived in Europe (at least Western Europe) for long. Though when I’m there I tend to like the food. But maybe indeed Europeans prefer less “American” foods (no idea how to define that term).
Fasting is one of the (many) things that make me throw my hands up in desperation at reading nutrition advice. The advice I used to hear was that one should eat small meals often, to the point of splitting the three traditional meals into 5-6 smaller ones. Then starting last year I start seeing praise for exactly the opposite approach, fasting for 24+ hours. I guess they can be reconciled if you don’t gorge at the end of each fast, but you see what I’m getting at.
There’s so much conflicting advise that my current course is just “do what you’ve been doing so far and hope it never stops working because you’ll be doomed”.
It might be the case that any change causes people to be more aware of how much they eat and thus makes them overeat less.
“A change is as good as a rest” strikes again.
I don’t think the evidence in favor of fasting falls into that bucket, if I’m recalling it correctly. Mostly because there are a bunch of health benefits that have come up in animal studies, as well as certain biomarkers in shorter-term studies where food intake was fully specified. In neither case the level of mindfulness about one’s food all that relevant.
I wonder if fasting (as in, actually spending a significant amount of time hungry, not just eating less) regulates the lipostat by building a tolerance for low leptin, just as overeating builds a tolerance for high leptin?
I did an “intermittent fast” which basically consisted of 3 days a week of eating nothing for breakfast and lunch, and then a modest (~500 calorie) dinner. Ate normally the other days, not particularly trying to be healthy / restrict calories. I did lose about 20 lbs over 3 months on that program, and it was relatively easy to avoid gaining back after I stopped fasting.
The first couple weeks were the hardest and I had hunger headaches and some fatigue. I adjusted partly just by getting used to it but also by adding a small snack (handful of almonds) at lunch time, and that made it pretty easy.
One thing I noticed was that I became acutely aware of actually being hungry, and realized how infrequently I was hungry otherwise. The small dinner at the end of a fast day was still satisfying, because I was very aware of the satiety signals coming through and the ravenous signals going away.
That I think helped with the sustainment – my body and mind got used to being hungry, and “hungry as the new normal” carried over after the fast period and I noticed fewer (or at least easier to ignore) cravings.
Hm — how clear is it that the problem is just food reward, though? I mean, yes, one of the hypotheses for what’s damaging the hypothalamus is that it’s just overeating, but it could also be something more specific (such as low fiber content). Actually, I don’t really see how the “it’s just due to overeating” idea is consistent with the “there is some second hit that is necessary” idea. If the second hit is the hypothalamic damage, but the hypothalamic damage is caused by overeating…? Well, I guess depending on what exactly the “second hit” hypothesis is, I guess it could still be technically a “second hit” if overeating causes the damage by means other than leptin, but a bit confusing terminology then. And the fact that lab animals have been getting fatter over time despite their diets remaining the same, as has been mentioned on this blog before, would indeed seem to suggest that there is another factor beside genes and overeating — which could be (or be one cause of) the “second hit” discussed above, perhaps?
Could it be something related to the generational testosterone decline in Western males?
If I understand correctly, the causes for it are unclear, but if there is some environmental factor (some kind of industrial pollutant/flavoring/additive that somehow gets into junk food?) that can have significant endocrine effects then I wouldn’t be surprised if it was involved in disregulation of the lipostat, whether through testosterone itself (which is involved in fat balance) or other hormones that affect and are regulated by the hypothalamus.
Women are still obese too, so it can’t be through testosterone – women normally have near-zero levels of that, so there’s nothing to disrupt by lowering it. If T is involved, it has to be as a symptom rather than cause.
Good point. Seems like it could easily be a symptom: some background pollutant could simultaneously be decreasing testosterone and damaging hypothalamuses (hypothalami?). Or, there could of course be two pollutants.
Endocrine disruptors as a class might still be involved, even if the pathways affected differ between men and women. Women have much less testosterone than men, but it still plays a role in the female endocrine system. While low testosterone is positively correlated with obesity with men, and may have a weaker correlation with overweight in women, female obesity is often associated with a hyperandrogenism in a feedback loop where increased adiposity generates higher androgen levels. Some researchers are investigating the role of sex hormone binding globulins – the bound/unbound hormone fraction may influence adiposity in both sexes. Many common forms of hormonal birth control affect SHBG levels.
Good point.
Xenoestrogens can decrese testosterone in men and they can cause endocrine distruptions in both genders.
Indeed, the age of onset of puberty in females has progressively lowered in the last centuries, and although many confounding factors, such as nutrition, may play a part, some studies have implicated xenoestrogens. (Wikipedia).
Potatoes are a diet food?
Maybe that’s why I lose weight during Passover.
I’m delighted to note that fries are made of potatoes.
Potatoes soaked in fat…
But apparently it’s not the fat that’s bad; it’s the tastiness itself.
Well, it’s both tastiness and caloric density, right? French fries have both, to a much greater extent then potatoes do.
Passover seems like the ideal weight-loss ritual based on this book. All my jewish friends find matzos hyper-unpalatable, and food variety is restricted.
Considering the Wall Street Journal article a couple weeks ago about all sorts of fancy matzo-flavored foods, I’m guessing not everyone agrees with your friends? When I tried matzo myself (I’m a gentile, so it’s pretty rare for me) I found it fairly good-tasting as crackers go.
I’ve gotten the same response from some goyim I know. I think the disparity of feelings between Jews and non-Jews largely comes from Jews associating it with periods of practicing highly inconvenient food restrictions during which we have to (by tradition, if not necessity) use matzoh as a bread replacement. Many things taste worse than matzoh, but few things taste worse in the moment than shmurah matzoh covered with sauce and cheese when you really want pizza. It probably doesn’t help that we also participate in religious rituals in which we sit at a dinner table for up to two hours without eating anything substantial, after which we’re compelled to eat (according to some) a whole matzoh plain as the first thing.
(Followed, of course, by more matzoh with horseradish and apples).
Out of curiosity, if Jews don’t like Matzo during Passover, then why not other forms of unleavened bread that are more soft or moist, like tortillas, or roti?
@Alexp
It’s seems to be against the spirit of the holiday. But kosher restaurants do use non-matza bread replacements.
I love matzos. And if you add haroset to it… Very, very palatable. Don’t eat much bread normally, btw, so it’s not super-inconvenient for me. Wouldn’t probably enjoy eating the whole leaf plain… though if it’s the fancy one, with eggs, also is very palatable. Same goes for matzah brei.
I don’t really get this argument. We don’t have to exactly match energy intake and expenditure every single day, because what determines the weight gain over a year is the average amount you ate over the entire year. Can’t it just be that people eat slightly random amounts every day, and exercises random amounts every day, and on the scale of years it averages out until we reach the weight where the negative feedback from caloric requirements matches the amount you tend to consume?
Like, tautologically, if someone’s weight is stable, then (food – work) can not vary very far from zero, but in a purely passive model that could be just because the amount of food they eat does not vary much and the amount of work they do also does not vary much. In order to test if there is any active control by the brain, it seems you at least have to have some information about how much variance there is in food intake and work, so we can compare it to how much the body weight varies.
Okay, I’ve gotten enough negative feedback about this point (phrased in various different ways) that I’m just going to give up and delete it.
I wouldn’t delete it entirely. The first paragraph is still accurate. Yes, long-term averaging does help some, but the fact that there’s a very good control system in charge of almost everyone’s weight is very important.
I’m against deleting it, because I just saw it quoted in the comments and thought, “what an interesting insight…wait was that in the article?”.
I think it’s an important point.
Sure, what’s important is that they are 98% accurate on average, over the course of the year, not that they are 98% accurate every single day. But even that seems to me to be pretty clearly false. There must be some negative feedback, either in hunger or in energy consumption.
I resisted the idea of calorie counting, until a question I asked on an open thread (“how can I tell when I eat enough food?”) suggested it anyway, and I’ve now been tracking calories for nearly a year, skipping times when I cannot due to travel.
I have a pretty good idea of how many calories I need to eat to lose, maintain, or gain weight. It took a few months of trial-and-error but I’m there. I am slightly nervous that when I next go back into weight-cutting mode that It Won’t Work Any More, but so far it seems like I can choose my weight.
I read Scott’s wonderful essay so I’m not saying this will work for everybody.
We’re talking about the accuracy of people who aren’t consciously trying to count calories, who haven’t even heard of a calorie.
Of course, but noting that it is “either” doesn’t help much—the rest of the article wants to talk about feedback in the form of hunger/fidgeting/etc, mediated by the brain. But (as quoted text acknowledges), there is also feedback from increasing energy consumption (which does not need to be mediated by the brain). In order to talk about the lipostat you need to distinguish those two mechanisms, and this argument doesn’t do that.
I tried MealSquares a while back, based on the sidebar advertisement, and liked them pretty well (“liked” in the “this works well for me” sense, not the “food reward” sense). But I don’t see how anyone who’s tried one could call them “hyperpalatable”.
Seconded. I’d rate them as solidly “dry vegan cafeteria scone”. (Although they aren’t, to be clear, vegan.) Not bad, but also not something you’d buy if you enjoyed eating.
That’s exactly the point. I too have had them. Note that it’s “not hyperpalatable”.
I enjoy food, a lot. But when travelling (which I do quite a bit for work), significantly less so – the options easily available to a weary traveller in a business district hotel (ie, room service, hotel restaurants and fast food) tends to be of the “hyperpalatable” kind, and is also high-calorie and have other properties that are commonly (but possibly incorrectly), considered “unhealthy”. And that’s before the temptation of dessert and a glass of wine or two kicks in. It’s also typically quite ridiculously expensive, and even when I don’t pay for it myself, I can’t help but recoiling a bit at what they get away with.
Long story short(er), I’ve taken to “Jake” which is a meal-shake. Same general concept as MealSquares as far as I can tell, except it’s a shake which does add a tiny bit of logistics. It’s, well, as bland as you could imagine a colourless powder mixed with tap water would be (it has a very faint vanilla flavour), but I get perfectly satiated, and I’ve been able to cut out “travelling-food” entirely. Last week I even brought my shake to the gym and drank it on the stationary bike while watching Netflix on my phone #lifehack 🙂
I couldn’t imagine replacing pretty much any “real meals” in my life with Jake (weeknight “can’t be bothered to cook” take away is probably next on the hit-list, though), but it’s definitely very powerful for on-the-go scenarios where “real meals” can be hard to come by (and, again, it would seem MealSquares could be used in the same way).
I’ve replaced my work lunches with mealsquares and an apple a few months ago, after reading about them on this site. I’ve dropped somewhere around 15lbs during that time. I credit the mealsquares lack of deliciousness. They taste acceptable, but they aren’t tasty. There is something about them that is very filling, and the apple is there to occupy me long enough for the satiation to kick in (mealsquares are small and it doesn’t take long to eat one).
I’ve always imagined mealsquares as low-quality lembas bread. Would this be accurate?
Funny, that’s what my wife calls them. I’m not sure how to answer the quality part. They taste vaguely like some foreign pastry that you’ll try once but wont reach for another unless you are really hungry. Chocolaty/whole bready/nutty substance that’s a bit too dry, and very thick. So the very opposite of angel cake. They are very filling. I’m not hungry for hours after eating one, despite it being slightly smaller than a slice of bread. I am not a light eater.
There’s a Tolkien word for that! Cram, made by the Men of Dale: it gives you the strength to keep marching for a day, but unlike lembas, it’s very much not tasty.
Well, now I know where cram rations in Nethack came from.
Exactly! MealSquares are closer to lembas than cram, but not by all that much.
Kinda, except they don’t have preservatives, and if you don’t keep them sealed and/or in your fridge they go bad pretty fast.
Last year I switched to eating a *very* regular diet for lunch and dinner. Breakfast was a single hard boiled egg and 2 pieces of sausage plus black coffee. Lunch was 8 to 10 ounces of plain or vanilla yoghurt with a scoop of coco flavored unsweetened whey powder to up the protein level.
This is pretty satisfying, and depending on workload (I do a combination of Linux administration, shell programming, and some sort of low to mid level management work, which is to say lots of brain engaged which sucks up glycogen) I get a little hungry about 3:30 or 4 PM. I’ve shifted my lunch time a bit to try to push that out to “quitting time”, but that’s not worked well.
These are also things that are readily available when I travel (which I’m doing a lot less this year than last).
I lost about 15 pounds of fat (and picked up some muscle from exercise) last year. Some of the fat came back, and the muscle stayed.
I thought I tended to get hungrier on brain-heavy days. Nice to know I wasn’t just imagining the effect.
I also tried the meal squares based on the sidebar ad here, and found them completely unpalatable. After failing to eat more than a couple bites or to convince anyone in my family to eat more than a couple bites, they ended up in the compost heap.
I’ve also tried soylent, and found it similarly unpalatable, though my spouse found soylent to be acceptable.
If I’m going to eat bland food, I tend to stick with rice or oatmeal.
I tried them too. I didn’t like them and couldn’t eat more than a few bites, which was disappointing because those few bites were absurdly filling.
On the other hand, I gave the remaining ones to someone else, and she eats them just fine. She uses them mostly as a cafeteria food replacement. So it seems one’s mileage may vary.
Strange, unlike apparently every other commenter so far, I found meal squares to be way too sweet. It’s more like (dry) cake than something I’d eat as a meal. It’s certainty sweeter than…noninvented(?)… food, aside from fruit and some outliers like sweet potato.
I drink soylent, which is also sweet, but not quite as bad.
It’s so interesting that most people here don’t find MealSquares hyperpalatable! I ordered them a couple of times and ended up binging on them. They were so convenient and tasty. I wish they could make a version without any sweeteners added. As it is, I find it hard to resist eating too many of them at a time!
As a not-quite-counterpoint but still related; I put in for an order of MealSquares based on this post, despite having seen it in the sidebar a number of times before. Partly it was just convenient timing as I’ve been getting interested in meal replacements again (my previous experience with Soylent was… not great), but also admittedly because there’s something deeply appealing to me about pitching one of your sponsors as “not hyperpalatable” and (justifiably!) expecting that to be effective.
If you’re hungry enough – perhaps because you have eating problems – just having everything in sufficient quantities tastes hyperpalatable. (Speaking from personal experience.)